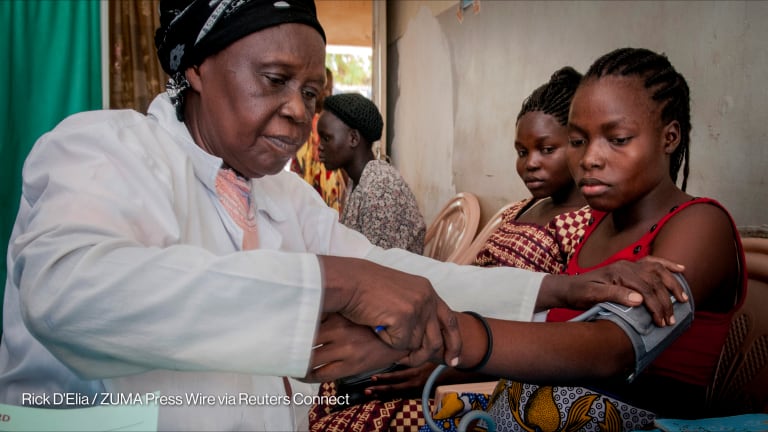Africa's $66B health financing gap requires private sector power, experts say

Addis Ababa, ETHIOPIA — Universal health care is vital to making sure Africa is not left behind in the quest to meet the Sustainable Development Goals, Ethiopian Prime Minister Abiy Ahmed said Tuesday to a standing-room-only audience. It’s the private sector that has a vital role in progressing national health plans, he said.
“Innovation is not coming from governments anymore; it’s coming from [the] private sector.”
— Michel Sidibé, executive director, UNAIDS“Public-private partnerships offer an easy entry point for sustainable health financing, recognizing that PPPs require great interdependence between public officials and private partners,” Ahmed said.
Heads of state, health experts, development partners, and the private sector met on the sidelines of the 32nd African Union summit for the Africa Business Health Forum on Tuesday to discuss ways to improve health care in Africa through public-private partnerships in an effort to achieve universal health coverage.
Under the leadership of the United Nations Economic Commission for Africa, the Aliko Dangote Foundation, and the Global Business Coalition for Health, government officials shared examples of how they have engaged private companies to improve health services delivery in the context of scarce public funds. U.N. officials, on the other hand, enumerated the various challenges facing the African health sector — from the high costs of largely imported essential medicines to the human resources and infrastructure gaps that limit the availability of quality essential health care services.
Statistics from the new UNECA “Healthcare and Economic Growth in Africa” report provide quantitative evidence that life expectancy has increased, infant mortality has decreased, and Africa is now healthier than 20 years ago. But troubling trends in health finance put these gains at risk. Africa has a health financing gap of at least $66 billion annually, the report states, with all but three African governments meeting the suggested 15 percent allocation of gross domestic product for health, as outlined by the 2001 Abuja Declaration.
To address this concern, the Dangote Foundation and GBCHealth launched the African Business Coalition for Health on Tuesday. The new collaboration outlines five primary objectives to achieve in its first three years, including working directly with companies to optimize workplace and community health programs, and advocating for policies and initiatives that drive national and regional change.
“Our call to action through this coalition is to strengthen the effort of our traditional supporters because the few health champions, even a few hundreds is not enough,” said Aigboje Aig-Imoukhuede, co-chair of GBCHealth.
Big business
Business opportunities in the health care and wellness sector in Africa are estimated to be worth $259 billion by 2030, with a potential to create 16 million jobs, the UNECA report estimates.
Still, experts argued that for this coalition to be effective on improving the access to — and the delivery of — health services requires not only more political will, but political choice via policy transformation, human resources strengthening, and innovative financing to close the standing health financing gap.
“You cannot think about health care just through public services,” Executive Director of UNAIDS Michel Sidibé argued. “Innovation is not coming from governments anymore; it’s coming from [the] private sector,” he said, explaining how HIV treatments have gone from 17 pills per day to a single-pill treatment, and which could soon become a self-injection thanks to private sector innovations.
In Botswana, for example, as a result of public-private partnerships, public hospitals are allowed to utilize the intensive care units of private hospitals to increase access to quality care for emergency and specialized services. District hospitals also outsource “soft services,” such as clinical waste removal, catering, and laundry to local companies.
“There are still more opportunities available for public-private cooperation: inpatient and outpatient care, mortuary services, pharmaceutical manufacturing, or human resources development,” Botswana President Mokgweetsi Masisi explained. “This gives just a broad overview of the immense opportunities available in just one country.”
Kenyan Cabinet Secretary for Health Sicily Kariuki explained how PPP interventions are enabling the east African country to improve quality access to health services.
For example, M-TIBA, a mobile health wallet created in partnership with Safaricom, CarePay, and PharmAccess allows Kenyans to save, send, and spend money on health care. Money stored on the app can only be used to pay for treatment and medication at its partner clinics and hospitals, which are internationally recognized for quality care.
The government’s Management Equipment Service project has also helped expand access to dialysis medical equipment, which is outsourced from private providers. In rural areas, telehealth clinics allow patients to interact with medical specialists through video conference.
There must be a focus on shared-value solutions for social impact that are mutually beneficial for governments, private partners, and citizens alike, Kariuki said.
Experts suggested the implementation of “sin taxes,” or taxes to discourage the consumption of products detrimental to health such as alcohol, tobacco, and sugary drinks as a means of filling the health financing gap in Africa. Nontraditional financing sources such as development impact bonds could also serve as a solution, according to Saurabh Sinha, head of UNECA’s employment and social protection department.
Though economic growth will undoubtedly create a greater ability for populations to afford quality health services, access to quality health care remains limited by the scarcity of public resources. According to UNECA’s health and economic growth report, the average annual value of illicit financial flows far exceeds the health financing gap, suggesting that by reducing these illicit flows, governments could finance health care and other social sectors.
“Together, we have an opportunity to demonstrate how investing in health and creating healthier populations can help businesses maximize shareholder value, accelerate economic growth and make entry into new markets more feasible,” Aig-Imoukhuede said.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5