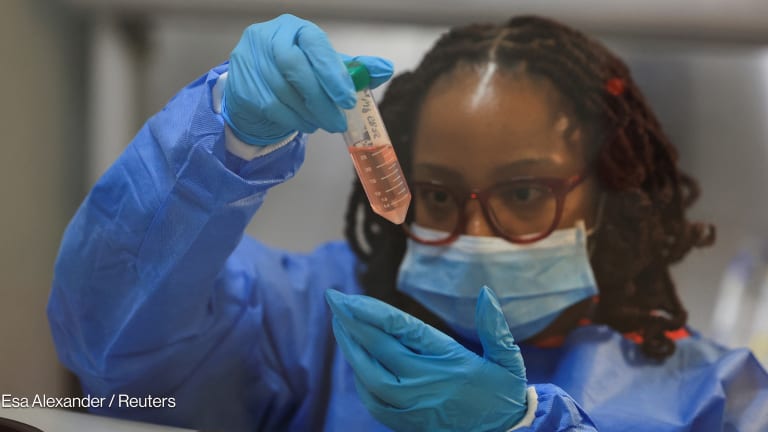
Africa's attempt to regulate traditional medicine fails to gain traction

Last year, Madagascar’s President Andry Rajoelina announced that the country had discovered a cure and treatment for COVID-19, a tea containing traditional Malagasy plants including artemisia. The announcement pushed African traditional medicine into the spotlight, with a renewed interest in the potential that such remedies may have and the dangers that untested cures may carry.
Though the exact composition of the remedy promoted by Rajoelina is still unknown, artemisia has been used in Chinese traditional medicine to treat malaria. Madagascar has continued to use what’s known as COVID-Organics, or CVO, in tea and pill form in its fight against COVID-19 — and exported it to other African countries, including Equatorial Guinea, Guinea-Bissau, the Republic of Congo, and Tanzania.
In a bid to enhance research and development of traditional medicines like CVO, the World Health Organization and the Africa Centres for Disease Control and Prevention established a Regional Expert Committee on Traditional Medicine for COVID-19 in July 2020, hoping to test traditional therapies and provide independent advice about their safety and efficacy. But six months after its formation, it appears that this attempt to regulate has failed to gain traction: None of the proposed remedies has yet progressed beyond phase II clinical trials.
“If we want to hold traditional medicines to the same regard [as modern medicine] … we should then hold them to the same standards.”
— Sarah Bosha, global health specialist, Eck Institute for Global HealthWHO estimates that more than 80% of Africans rely on traditional medicine for their health care needs. However, despite the widespread use and claims made by Rajoelina, Madagascar still continues to record cases of COVID-19. At the time of publication, the country has recorded just under 20,000 cumulative cases and 279 deaths.
The need for more investment
Information provided by WHO on ongoing clinical trials for traditional medicines indicated that research institutions looking at traditional medicines are largely stalling out during phase 1 and 2 trials, “due to lack of financial resources to undertake phase III clinical trials which will accumulate enough data and generate scientific evidence on the safety and efficacy to allow wide use of the products.”
Africa CDC Director John Nkengasong, also confirmed that though the committee is available and ready to test products, no traditional medicine group has yet approached the committee to assist in a large scale clinical trial.
When modern medicine flounders, should traditional healers fill the void?
Traditional healers are often the first people many South Asians turn to when health problems arise. Given the uncertainty about how to best manage COVID-19, how can clinically trained health workers and traditional healers work together — and should they?
Professor Nceba Gqaleni, a traditional medicines specialist at the Africa Health Research Institute said he believes that though COVID-19 presented an opportunity to invest in traditional medicine, countries failed to make the necessary investments to fast track the process.
“Clinical trials are really expensive so it does need to take governments who think differently, to develop the pharmaceutical industry,” he said, adding that government investment will be key to kick-starting a self-sustaining pharmaceutical industry.
“There is so much potential that if we took it more seriously and we made sure to have greater protections, we would plough more resources into developing our own scientific bodies that develop these traditional medicines,” said Sarah Bosha, a specialist in global health with the University of Notre Dame’s Eck Institute for Global Health.
While she said she sees a huge benefit for both Africa and the world in the development of these medicines, she said testing is key. “If we want to hold traditional medicines to the same regard [as modern medicine] … we should then hold them to the same standards.”
The trust gap
Dr. Jean-Baptiste Nikiema, a regional adviser on essential medicines at WHO Africa and a member of the committee on traditional medicine, believes that some of the problems with regulation are related to political interference and transparency.
Though the committee had indicated that it would work with the Scientific Committee of Madagascar to prepare to conduct a phase 3 clinical trial of COVID-Organics, Nikiema explained the country hasn’t submitted results for its phase 2 trial, and that information submitted after phase I trials “did not include any comprehensive data.”
“Some researchers may feel that someone may steal the information and this may take the entire process to some very difficult situations,” Nikiema said. “The capacity [to regulate] is already in place but some researchers try to bypass [it].”
Bosha added that in some instances, “for political mileage and maybe out of genuine desperation or out of greed,” politicians push cures that are not scientifically sound.
Bosha cited examples of former South African Deputy President Thabo Mbeki pushing Virodene, an industrial solvent later found to be unfit for human consumption, as a breakthrough treatment for HIV, in 1997. Ten years later, then-Gambian President Yahya Jammeh promoted a secret herbal blend that he claimed was an HIV cure. He’s currently being sued by survivors in the Gambian High Court.
Improved communication and self-regulation
For Gqaleni, the solution may lie in communication: By explaining the scientific process to traditional practitioners, institutions might empower them to regulate their own practices.
“Traditional health practitioners are not scientists and they do not understand science; they work in their own way, within their own philosophy so they may not understand what we are talking about in terms of scientific research,” he said. “But when it is explained properly I have not seen any traditional health practitioner opposed to good scientific research.”
In Bosha’s view, regulation would be more effective at the local level in each country as there can be a swifter resolution of issues like medicines that turn out to be harmful. Still, that depends on each national regulating body being “equipped and educated” to handle the task.
Nobongile Kakayo, a traditional practitioner and member of the Traditional Healers Association in South Africa, agreed that there is a need for better communication and consultation, but is skeptical of some pharmaceutical solutions that have undergone extensive trials proving their efficacy, like vaccines.
“We should have been involved from the beginning [of the pandemic] when people got sick and we could have helped them,” Kakayo said. “We believe that our traditional medicine can help but we know nothing about a vaccine that comes from outside the country.”

Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5