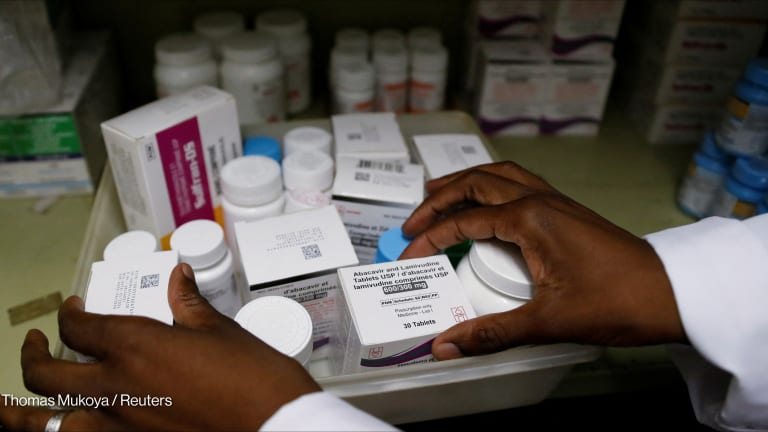
The World Health Organization recently announced that it was seeking input on the three global health sector strategies — HIV and AIDS, viral hepatitis and sexually transmitted infection — it was drafting until April 30. The strategies, which will cover 2016-2021, will be finalized at the 69th World Health Assembly in 2016.
Among the three health issues, viral hepatitis has arguably received the least attention. According to Jennifer Johnston, executive director of the Coalition to Eradicate Viral Hepatitis in Asia Pacific, viral hepatitis is the eighth highest cause of mortality around the world, causing around 1.4 million deaths from acute infection and hepatitis-related liver cancer and cirrhosis every year. It is a toll comparable to that of HIV and tuberculosis, and yet funding to combat viral hepatitis has significantly paled.
In the most recent report on donor funding for global health released by the University of Washington’s Institute for Health Metrics and Evaluation, viral hepatitis is not included among the diseases that donors have addressed.