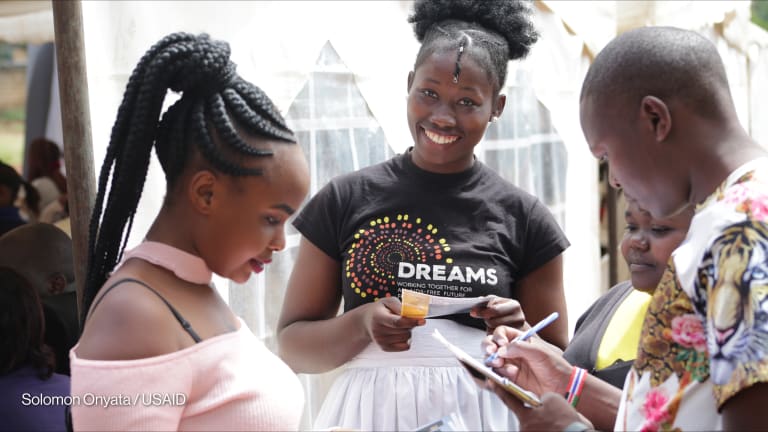Centering the HIV response on adolescent girls key to meeting targets in Africa

Last year, UNAIDS proposed a new set of bold HIV targets for 2025 in order to get the HIV response back on track to meet the Sustainable Development Goal of ending the AIDS epidemic by 2030. Currently, new HIV infections continue in certain regions and among key populations. In sub-Saharan Africa, nearly 1 in 4 new infections are among adolescent girls and young women aged 15–24 years old, who make-up only 10% of the population.
A report by the organization found that five years after a global commitment to fast-track the HIV response and end AIDS by 2030 was made, the world was off track as agreed milestones for 2020 have been missed.
Some of these missed milestones include reducing new HIV infections and AIDS-related deaths to fewer than 500,000 and eliminating HIV-related stigma and discrimination by 2020.
Though UNAIDS says that the global AIDS response was off track before the COVID-19 pandemic hit, the organization found that the spread of COVID-19 has created additional setbacks. As a result, there could be an estimated 123,000 to 293,000 additional new HIV infections and 69,000 to 148,000 additional AIDS-related deaths between 2020 and 2022.
“We really need some kind of concerted effort ... on the adolescent ... If you have an adolescent coming to a primary health care center, a lot of care can be very judgmental.”
— Professor Ameena Goga, director, HIV prevention unit, South African Medical Research CouncilThe new targets focus on increasing HIV and sexual and reproductive health services, removing negative laws and policies, as well as reducing stigma and discrimination. They also aim to “address the inequalities on which HIV, COVID-19 and other pandemics thrive and put people at the centre, especially the people most at risk and the marginalized.”
In sub-Saharan Africa, health experts believe that in order to achieve these goals it will be essential to center both the HIV and COVID-19 response on adolescent girls and young women — who are disproportionately affected by HIV — by increasing and improving interventions targeting this key population group.
Disruptions due to COVID-19
Data from sub-Saharan Africa published in The Lancet has also shown that the COVID-19 pandemic has eroded progress made in improving the health and well-being of adolescent girls and young women and caused a reduction in HIV treatment access.
More on HIV/AIDS:
► Cabotegravir also works for women, HIV prevention study reveals
Professor Ameena Goga, director of the HIV prevention unit at the South African Medical Research Council, explained that a combination of effects, that include limited access to health care, contraception, mental health services, schools, and the services offered there, has put adolescent girls and young women at a particular disadvantage during the COVID-19 pandemic.
“The effects [of COVID-19] are being measured and more and more it shows a combination of effects; … [putting] adolescent girls and young women in particular at a disadvantage,” she said.
Aeneas Chuma, interim director for the UNAIDS Regional Support Team for Eastern and Southern Africa, agreed. According to Chuma, before the COVID-19 pandemic, the uptake of biomedical interventions such as pre-exposure prophylaxis had been encouraging among this group, yet “under COVID-19 things were disrupted a little bit in terms of access to services.”
Centering responses on adolescent girls and young women
“What we have learned is that the solution lies with the concerned population group itself. The adolescent girls and young women, I think they have to be at the center of any decision-making about their own lives.
“This has to be recognized formally through the education system and in society and culturally and even at home, but this requires huge behavioral and cultural change and ... a lot of investment,” Chuma said.
Goga agreed, adding that there is a need to reimagine interventions that cater specifically for adolescent girls and young women. She explained that currently adolescents fall in between groups, as they are too old to fall within child health guidelines — which usually include children aged 12 years and under — but are too young to be included within adult services.
“We really need some kind of concerted effort, whether it be permissions or recruiting people who focus specifically on the adolescent ... If you have an adolescent coming to a primary health care center, a lot of care can be very judgmental, depending on what the need of that adolescent is and depending on who is attending to that adolescent. There is a lot of judgement about requests for contraception, requests for abortions, and mental health needs are not really taken care of,” she said.
Chuma further noted that there is also a need to remove policy and legal constraints to adolescent girls and young women accessing sexual and reproductive health services. In some countries in the region such as Zimbabwe and Zambia, the age of consent to access sexual and reproductive health services is between 16-18 years.
“If girls, for example, are engaged in sex before the age of 15, it makes no sense to have laws which prevent girls to access sexual and reproductive health services if they are under the age of 15. So laws and policies first of all should be a little bit more responsive to the special needs of this cohort of the population and make sure that the barriers that affect access, both legal and policy, are removed,” he said.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5