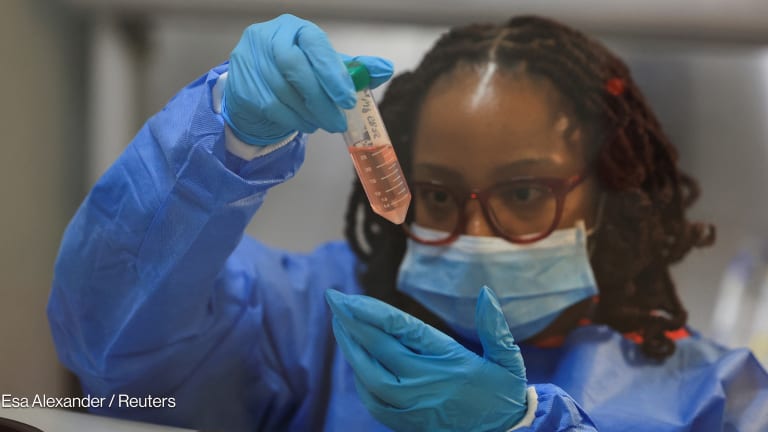
Ebola in Tanzania? A question on global governance for infectious diseases

MANILA — Last week, the U.S. government warned travelers of “probable Ebola” in Tanzania, even as the Tanzanian government and the World Health Organization engage in discussion after the latter’s public accusation of the government’s refusal to share information on suspected Ebola cases in the country.
Questions now arise on the state of the International Health Regulations as a global governance structure for infectious disease outbreaks.
IHR is an international, legally-binding instrument agreed to by 194 countries in monitoring and controlling the international spread of diseases. The present version, which entered into force in 2007, has a more expanded scope and clearer mechanisms in place for the coordination and reporting of diseases. Today’s IHR covers existing, new and re-emerging disease pathogens, versus the 1969 version that focused only on three diseases: cholera, the plague, and yellow fever.
But the current version also reflects lessons learned from previous disease outbreaks, in particular, the SARS pandemic of 2003. That outbreak, which spread across five continents, underscored the importance of countries’ timely reporting of unusual or unexplained health events and led to WHO being given authority to consider unofficial reports of public health events and obtain verification from countries — which the U.N. aid agency did in the case of Tanzania.
Several international experts applauded WHO’s public statement, which they described as a rare and extraordinary move by the health agency.
“This is not something that WHO does without a great deal of thought,” said Rebecca Katz, professor and director of the Center for Global Health Science and Security at Georgetown University.
David Fidler, adjunct senior fellow for cybersecurity and global health at the Council on Foreign Relations, said countries not forthcoming about disease events within their territories is not new. It happened during the MERS outbreak in 2013 in Saudi Arabia, for example. But in the present situation, a declaration of a public health emergency of international concern is in place, he explains.
“I think in MERS we had lots of discussions between WHO and the various governments, a bit more under the radar if you will, rather than WHO having to call out any specific country. And of course that was probably happening before WHO made this statement at Tanzania and I'm absolutely sure that's what's going on right now,” he said.
IHR: A treaty with little enforcement mechanisms
But beyond the public call-out, there’s not much WHO can do to compel countries to report public health events under IHR.
It is a treaty with “very limited sticks,” Katz said.
“There's limited enforcement on [the treaty]. And one of the reasons is I think the assumption going into creating this was that, there's kind of a baseline assumption that all countries want to protect their population health,” Katz said.
The expert noted how no country has really been punished for not building its core health capacities, even though it’s part of countries’ obligations under the treaty. Again, this is under the assumption that countries want to, but just don’t have the resources, she said.
But it then begs the question: How to compel countries to report?
“Although the IHR (2005) do not include an enforcement mechanism per se for States which fail to comply with its provisions, the potential consequences of non-compliance are themselves a powerful compliance tool. Perhaps the best incentives for compliance are ‘peer pressure’ and public knowledge,” according to a WHO FAQ on the IHR.
The assumption is that with the availability of electronic media, “nothing can be hidden for very long.” Countries that fail to comply with IHR could face a number of consequences, such as economic isolation and increased health risks for the affected population.
“I think what they would risk, if this goes on, is the loss of confidence of neighboring countries … They could risk countries around them, or other countries in the world, instituting measures, of putting ... some kinds of restrictions in place, because of the uncertainty of what's going on in Tanzania,” said Thomas Inglesby, director of Johns Hopkins Center for Health Security.
“Obviously, I think [this] would be a terrible, terrible move. And I really hope that no countries take those kinds of actions,” he added.
Last Friday, the U.S. government updated its travel warning for Tanzania, telling visitors to “exercise increased caution” because of a “probable Ebola” case in Dar es Salaam.
If a state wants to file a dispute against Tanzania for not reporting, the treaty has a mechanism in place under Article 56, which states that disputes between state parties in the interpretation or application of the regulations can choose to settle it through negotiation or other peaceful means.
If this fails to resolve the issue, the state can seek the help of the WHO director-general for arbitration, or seek dispute settlement mechanisms of other intergovernmental organizations.
WHO can also issue travel and trade recommendations, which could have massive economic consequences for the country in question, Katz said.
But the likelihood of that happening is low compared to countries violating the aid agency’s recommendations to keep borders open. Countries were fast in calling for travel bans during the 2009 swine flu outbreak despite WHO’s advise against one. Rwanda closed its borders for a few hours on Aug. 1 after the third case of Ebola was confirmed in the city of Goma in the Democratic Republic of the Congo, against WHO advice.
“Closing borders could have disastrous consequences for the lives and livelihoods of the people who cross the border every day for trade, education, or to visit relatives. Such restrictions force people to use informal and unmonitored border crossings, increasing the potential for the spread of disease,” WHO Director-General Tedros Adhanom Ghebreyesus said after declaring the outbreak in DRC a public health emergency of international concern.
A question on global governance structures for disease outbreaks
The fact that IHR does not have enforcement mechanisms in place is not unusual, Fidler said, an expert on international law and global health.
The United Nations doesn’t have enforcement powers, and that’s how international law works, he said. Even the dispute mechanism under IHR is not unique, he said, as every single treaty has one. But even if a country has any issues with another country in the application or interpretation of the treaty, the dispute mechanism has not been and would not be the best strategy to pursue, he argued.
Most disputes don’t get resolved in international courts, but through diplomacy, pressure, dialogue, incentives, and other things, he said.
“No country is going to bring a case against Tanzania to go through the formal dispute settlement mechanism or dispute settlement process set up in the IHR. It just isn't gonna happen. And it would take years for that to resolve itself, which isn't going to help us deal with the problem, right? We have a crisis going on and we need to know whether there are Ebola cases in Tanzania,” he said.
But what’s unusual and rare in international law was WHO member states giving the director-general the authority to declare a public health emergency of international concern under IHR, even against the objections of the affected state, he said.
“The ability for WHO to call out a country over its objections, release information that it obtained from other sources rather than the government of Tanzania, that's an unusual ... extraordinary authority,” he said.
The approach is meant to get countries to understand that releasing information early and cooperating with WHO on serious disease events is the best approach politically, economically, and from a public health perspective, although that doesn’t guarantee states following through.
“But that means WHO can keep coming back to Tanzania and say, 'you know, we've got more information you need to verify.' If they don't hear anything back, WHO can share that information with the rest of the world that cranks the pressure on Tanzania,” he said.
But he underscored the need to engage in a dialogue about IHR and the state of global health governance, particularly on disease outbreaks — an issue Katz also pointed out, especially as experts predict the frequency of disease outbreaks in the coming years.
“I think the past year plus … in addition to just measuring the morbidity and mortality that's been horrible from this outbreak, it's also raised a whole bunch of questions about the importance of governance structures and the role of the WHO and how the global community works together, from the debates over when a PHEIC should be declared, to the challenges of responding to public health events in the midst of conflict that we're only going to see more often,” Katz said.
Fidler, in an article he wrote back in July and shared with Devex, argued IHR has been “battered and bruised” with the push and pull over declaring a public health emergency of international concern in the current Ebola outbreak in DRC. He accused the emergency committee of “abusing its authority” by making recommendations on the basis of whether or not they think declaring a PHEIC will have positive or negative consequences.
“They're bending over backwards not to recommend a declaration … that's where I think they get into trouble and they abuse their authority because they play with the definition of a public health emergency of international concern in such a way that it's absolutely clear they're trying to do everything they can not to recommend a declaration. And that's interesting, right? So that really goes to the heart of, ‘what's the point, what's the purpose of this authority in the IHR today?’” he said.
He underscored that IHR remains an important framework, but fear of the repercussions if confidence in some components of IHR, such as the declaration of a PHEIC, starts collapsing.
“I'm just really worried about that because I think that's in fact what we've seen in the past with the previous versions of the IHR. States eventually just didn't care anymore and didn't even bother to implement it,” he said. “And I just don't think we want to regress in that way. And that's why I think we need to step back and have a broader conversation about where we are with the IHR.”
Asked whether the international community has any alternative mechanisms from IHR, Fidler said: “Well, I don't know, frankly, and that's what worries me because I don't see plan B.”
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5