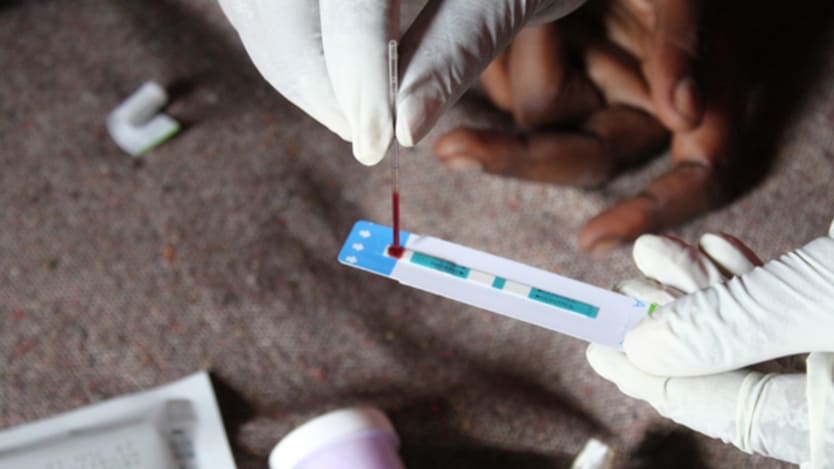
The battle to defeat HIV will be won or lost in middle-income countries.
Significant funding cuts made to MICs by donors like the United Kingdom is a key issue for us and for anybody working on HIV. Only 15 percent of people living with HIV will be living in low-income countries by 2020, which will account for an even lower percentage of new infections.
Countries that talk about ending HIV and at the same time are limiting development assistance solely to LICs are being disingenuous. We have been raising this issue for years, at the Global Fund to Fight AIDS, Tuberculosis and Malaria where I was a board member and with many other donors. We have prepared numerous briefing documents looking more generally at the impact that decisions made on the basis of gross domestic product per capita have on the ability to respond to the HIV epidemic.
Donor withdrawal is one of the more visible consequences of becoming an MIC, but that is compounded by medicines and other health commodities becoming much more expensive. We have been raising the need for more gradual and thoughtful transitions.
We are also pushing for donors to consider the policy space available as seriously as they consider the fiscal space. Many MICs might have fiscal space to buy more drugs and health commodities, but they don’t have the policy space to support the stigmatized and criminalized populations that bear the brunt of the HIV epidemic.
HIV has taught us a lot about the impact of partnerships across researchers, care providers, politicians and affected communities, and the impact of international solidarity. These have been critical partnerships where we hold each other to account.
It is only if that spirit underpins the sustainable development goal on health, and the different targets, that anybody will feel truly accountable for them. The existing global architecture makes systematically tracking the quality of health services extremely difficult, determining who is being “left behind” (or rather “shut out”) a challenge.
Indeed, inequity is on the increase and needs to be tracked — and not just from an income perspective. Who is being shut out of “universal” health coverage? When it comes to HIV it is precisely the stigmatized and criminalized populations who are most critical to curbing the epidemic: sex workers, transgender women, men who have sex with men, people who inject drugs. Specific indicators and social mobilization of these communities is what will keep service providers honest.
While I would argue that a human rights-based approach was missing from the Millennium Development Goals, and is missing from the proposed SDGs, the European Union has traditionally had a set of values incorporating equity and social justice at their core.
It is estimated that in 2020, 70 percent of people living with HIV will be living in MICs. Therefore, the continued withdrawal of funds from these countries will have devastating effects on the progress made in the global response to HIV. The EU must remain a champion for equity, for meaningful participation of affected communities, for sexual and reproductive rights, and commit to ambitious targets.
This piece is part of a series of articles to be published in “Health Matters,” a news bulletin commissioned by Action for Global Health for European Health Month, as part of the European Year of Development 2015. The paper brings together key stakeholders working on health to confront the challenges of the post-2015 framework, provide recommendations on the means of implementation, and raise awareness on the importance of health for all.
Join the Devex community and access more in-depth analysis, breaking news and business advice — and a host of other services — on international development, humanitarian aid and global health.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5








