NAIROBI — In a laboratory in Dar es Salaam, Tanzania, rats are led through a narrow cage sniffing, one by one, samples of phlegm from the lungs of potential tuberculosis cases. If one of the rats sniffs out a match for TB, it will hover its nose over the suspicious sample for three to four seconds. It is then rewarded with a mix of crushed bananas and peanuts.
While rats have been typecast as filthy, disease-ridden sewer-dwellers, this team of rodents are working to defy these stereotypes with their efforts to reduce the global burden of TB, which is the leading infectious disease killer in the world. Far from being the villain of the fight against a killer disease in humans, these rats could be the heroes.
The rats are part of a research program between APOPO, a Tanzanian-based nonprofit organization, and the Tanzanian government’s national TB program. The laboratory is using rats because they are quicker and suspected to be more accurate than the traditional method of testing samples at the clinic-level. Last year, the national health authorities expanded the research program to test samples from another 29 clinics.
Misdiagnosed
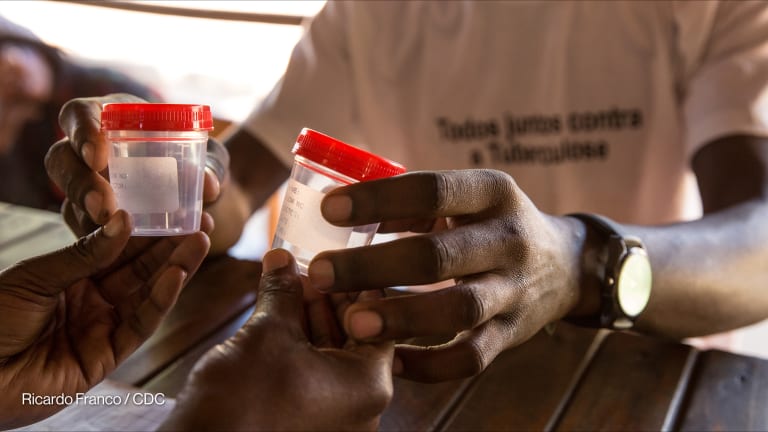
Tuberculosis is preventable and curable, but it is difficult to detect. Because of this, many clinics in resource-stretched settings are misdiagnosing the disease. The most common test for diagnosing tuberculosis is sputum smear microscopy, according to Médecins Sans Frontières. This involves a patient coughing up sputum from their lungs, which is the phlegm that comes from the lower respiratory tract when coughing. The sample is then investigated under a microscope.
For diseases like malaria or HIV, an antibody test is used, which includes identifying whether the body has created antibodies to fight the disease. With TB, you need to test the actual organisms instead, James Pursey, head of communications for APOPO, told Devex. But the bacteria from TB is not always easy to spot. Because of this, sputum smear microscopy detects less than half of all active TB cases, according to MSF.
In resource-stretched contexts, clinics also have limited capacity. They are only testing around 15 to 20 samples per day and are often sending patients home with a misdiagnosis, to infect others, said Pursey. There are some 4.1 million cases of TB that went undetected in 2016, according to the World Health Organization.
“There is a big gap where the clinics are slow, and they can’t cope, and they are not entirely accurate, because it’s difficult for them to find that bacteria in the smear test,” he said.
In some cases, countries are collecting samples, but the equipment cannot process the samples as quickly as needed, Cynthia Mwase, head of the Africa and the Middle East department grant management directorate for The Global Fund, told Devex.
“Our biggest issue in TB is that we need to find the 40 percent of cases that we aren’t finding. Then we could possibly reduce incidence,” she said.
Speedy and accurate
See more related topics:
► 3 innovations that could transform TB diagnosis and care
► In the year of TB, advocates want more than a political commitment
► Advocates to seek TB funding targets at 2018 high-level meeting
This is where the rats step in. The rats are quicker and suspected to be more accurate than the tests that are happening at the clinic level. A single rat can test around 100 samples in about 20 minutes. These rats, which are trained through a click-and-reward system, are about 75 percent accurate, according to the organization. APOPO’s research suggests that the organization can increase TB detection rates by about 40 percent.
Tanzania was the first country to partner with APOPO on a research moratorium of understanding. They started testing samples of sputum in 2007. Last year, the nation’s health authorities expanded the program to 29 new clinics, to a total of 57 nationwide.
When a patient is examined by doctors at a participating clinic in Tanzania, and TB is suspected, sputum samples are taken and tested by the clinic. Each day, APOPO then collects samples by motorbike from 51 clinics in Dar es Salaam, and six more in the Morogoro region, where APOPO’s main partner in the research program, Sokoine University of Agriculture, is located. They are then brought to the APOPO facility for overnight testing to get the results back to the clinics by 8 a.m. the next day. Samples marked as positive by the rats are then re-tested, using World Health Organization-endorsed methods.
Beyond their work in Tanzania, APOPO also works with 14 clinics in Mozambique, and will soon be opening a research facility in Addis Ababa, Ethiopia. The organization’s strategy is to build in cities where there are influxes of people from rural areas, living in close quarters. The rats are seen as good candidates for the work because they are easy to transport, have a cheap diet, and are resistant to heat and local diseases.
The organization has also found other ways to use them. APOPO is using rats to detect landmines, because they are too light to set off the landmine, and it is working on developing the expertise to use them to detect endangered wildlife trafficking of animals and hardwoods. The organization is currently using pangolin scales it collected from the Dar es Salaam zoo to train the rats to protect the species from smuggling.
Lingering questions and scaling up
There are still many questions about how exactly these rats can sniff out TB and how to improve their performance.
In some cases, all of the rats fail to flag a sample that the clinic deemed positive for TB. In others, all of the rats indicate that a sample is positive, but the clinic says it is negative.
APOPO thinks the rats could still be on to something. There is a theory that the rats might be finding early-onset TB in the cases where they say a person is positive and the clinic disagrees, said Pursey.
Researchers also want to dig into questions such as how nutrition impacts their performance and whether there is a time of day when they are at their peak performance.
APOPO expanded its research and development efforts last year, which included establishing a research and development scientific advisory committee. But their growth in both areas of research and scaling up the project into other countries faces funding shortages.
For now, starting a program using the rats involves start-up costs including building and staffing facilities, as well as training the rats. But APOPO is hoping that deploying the rats could lead to economies of scale if the programs are expanded.
Dr. Suvanand Sahu, deputy executive director of the Stop TB Partnership secretariat in Geneva, told Devex that APOPO’s research program is an example of “excellent innovation which challenges the status quo of using sputum microscopy for TB diagnosis.” The Stop TB Partnership is hosted by the United Nations Office for Project Services and brings together 1,600 partner organizations working to end TB.
But before scaling up, more research is needed, he said. This includes identifying the substance in the sputum samples that the rats are able to smell in order to mark the sample as positive for TB. The next step could be to create an “electronic nose” that could detect the TB bacteria and result in a breathing test for patients. This device could potentially be scalable to other countries.
“If we can develop such a device, then it can help overcome the inability of current diagnostic tools to scale up to billions of people in need of screening for TB. Such a breath test can be used as a screening test or even a diagnostic test depending on the accuracy of test results,” he said.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5