India rolls out new TB diagnosis aimed at catching child cases
KATHMANDU, Nepal — Newly published estimates on child mortality from tuberculosis paint a dismal picture. Almost 200,000 children under 5 died of TB globally in 2015, a far higher number than previously thought and enough to place TB among the top 10 causes of child mortality worldwide, according to the September 2017 issue of the Lancet. Yet, nearly all the children who died from the disease did not receive treatment, indicating a “substantial scope to reduce this burden,” the article said. Therefore, despite the currently dire situation, there is a silver lining for countries that are bearing the heaviest burden of the disease.
India is among these countries. The nation hopes to utilize an opportunity in combating this pediatric epidemic. India will soon roll out a national program aimed at speedily spotting cases of TB and drug-resistance in all suspected cases. TB has often gone untreated in children because it has also gone undetected. But if children get the drugs they need, the outcomes are often better than those of adult patients.
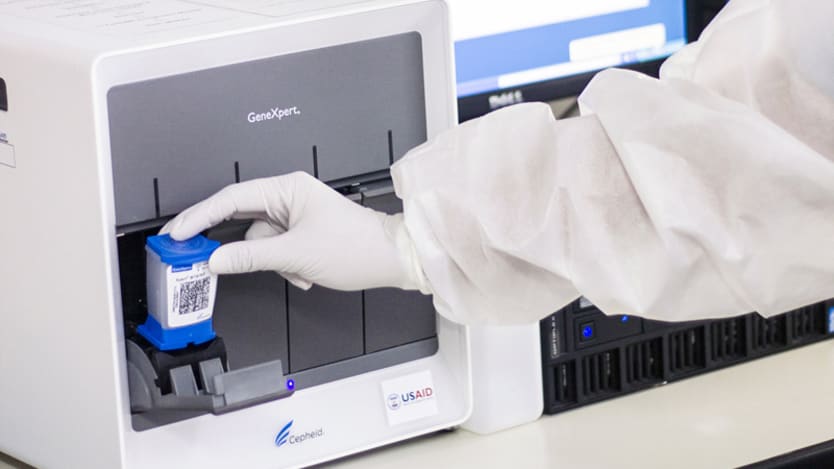
India’s Universal Drug Sensitivity Test, which begins this September, will exploit a relatively new technology called GeneXpert, a molecular diagnostic test for the early diagnosis of TB. This device allows for diagnosis within 100 minutes — far faster than conventional tests, which take days or even months.
See more stories in this series:
▶ Opinion: How public-private partnerships can wash away poor sanitation
▶ Ghana turns to community health workers in bid for universal coverage
▶ Opinion: Universal health coverage and the power of partnerships
▶ 3 things putting Rwanda on the path to UHC
▶ How to achieve universal health coverage? Focus on primary care
“Because of the speed of diagnosis, we’re able to reduce loss to treatment. That’s one of the reasons why we’re able to link more than 90 percent of children with treatment,” Sanjay Sarin, India lead at the Foundation for Innovative New Diagnostics, told Devex. FIND co-developed GeneXpert (also known as Xpert MTB-RIF) and has supported its rollout across India.
If it succeeds, the program could both significantly reduce child mortality from TB and serve as an example for other countries looking to reduce child deaths. Some 70 percent of pediatric deaths from TB occur in Africa and Asia, according to the Lancet study.
“The death toll is mostly preventable,” Dr. Madhukar Pai, TB expert and professor of epidemiology at McGill University in Montreal, told Devex. “Improving pediatric TB diagnosis is one key intervention to reduce mortality.”
Missed cases
Prior to the newest Lancet data, TB statistics have generally underestimated the burden among children. There are few global data sources available to monitor the prevalence of TB in children and many of the clinical symptoms overlap with other common childhood diseases. This means cases can easily be overlooked. Finally, health workers have had few and poor diagnostic tools to confirm cases.
That underestimation has had real policy implications, drawing attention and funding away from pediatric treatment. Due to lack of data, TB has not been on global public health institutions’ radar “the way it should have been,” Lancet study lead author Pete Dodd, a research associate in health economic modelling at the University of Sheffield, told Devex.
“There’s no doubt that under-five mortality estimates are influential in shaping thinking and spending around public health strategies,” he added.
What has been happening is a vicious cycle: Poor diagnostics mean a dearth of data and uncertainty about childhood cases, which leads to inadequate global investment in improving detection and care.
“There’s been a global push to improve diagnostics for TB, but they’ve failed to address the challenges in children,” infectious diseases specialist Dr. Jay Achar, who works as a TB/HIV program and research adviser at Médecins Sans Frontières, said. “Without information, it’s difficult to advocate for more resources and focus attention to this problem.”
Most low- and middle-income countries’ health systems rely on X-rays and sputum smears to diagnose TB. The latter requires patients to cough up phlegm, which many young children aren’t able to do. Even if they can, the amount of bacteria these samples produce is too low for microscopy to detect.
In addition, up to 30 percent of children have extrapulmonary TB, which means the disease spreads beyond the lungs to other parts of the body. Smears fail to detect this.
New diagnostics
With better diagnostic tools available, India is now among the countries looking to expand their roll out.
In 2010, the World Health Organization endorsed the GeneXpert machine, as well as multiple-drug resistant TB (MDR-TB) and TB complicated by HIV, both of which are more difficult to diagnose. The machine was co-developed by the University of Medicine and Dentistry of New Jersey and FIND. It is fully automated and requires minimal training to use.
Machines have been slow to reach the countries where they are most needed, often because of limited national TB program budgets, Pai said. By the end of 2016, some 23 million GeneXpert cartridges had been procured by the public sector in 130 countries at concessional pricing, but smear microscopy continues to be the most widely used test for TB, a recent study published in the European Respiratory Journal said.
“While all National TB Programs do have GeneXpert machines, they are underusing them by rationing the test only for a few select groups rather than making them freely available to all TB patients,” said Pai, who was part of the team that conducted and published the study.
India’s new push aims to make GeneXpert a first-line tool. Some 639 machines are now in use throughout the country, according to FIND’s Sarin, which is partly due to an initiative the organization began in 2014. It advocates for the use of GeneXpert to rapidly diagnose pediatric TB in 10 high-burden Indian cities, including Delhi and Kolkata. The initiative — a collaboration between FIND and the Revised National Tuberculosis Control Program and funded by the U.S. Agency for International Development — works to enable rapid linkage to treatment for children in order to reduce mortality and transmission.
FIND has built a network of local doctors working in public and private facilities to aid and expedite diagnosis and treatment. When a child comes in with suspected TB, a courier can come and pick up the sample from the patient and transport it to a government facility where FIND’s specialized laboratories dedicated to pediatric TB are located. Project staff members inform the health provider of the test results via text message or email within 24 hours, enabling the doctor to immediately start the child on treatment.
“We’re basically trying to mimic what’s happening in the private sector, but much faster and for free,” Sarin told Devex.
Once on treatment, children generally respond better than adult patients, according to Achar.
“When children get TB, they get it very aggressively,” he said. “But on the flip side, if you start them on appropriate treatment, they tend to do really well — they have better outcomes than adults with fewer side-effects.”
Given children’s ability to combat the deadly disease, improved diagnostics give experts hope. If cases and be treated, and contact tracing aggressively pinpoints other children at risk, many children may live.
“Our work has demonstrated a very simple and uncomplicated operational service delivery model, which can certainly be leveraged in other countries with high-disease burden,” Sarin said.
A working model for diagnosis and treatment in combating pediatric TB will require lobbying for more and better resources.
“It’s important to focus on children,” Sarin said. “They are very vulnerable and the longer the delay in diagnosis, the higher chances of mortality.”
How do we ensure that people worldwide get the care they need without the risk of being pushed further into poverty? Devex explores the path to universal health coverage. Join us as we ask what it will take to achieve UHC for all by visiting our Healthy Horizons site and tagging #HealthyHorizons, #Health4All and @Devex.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5


