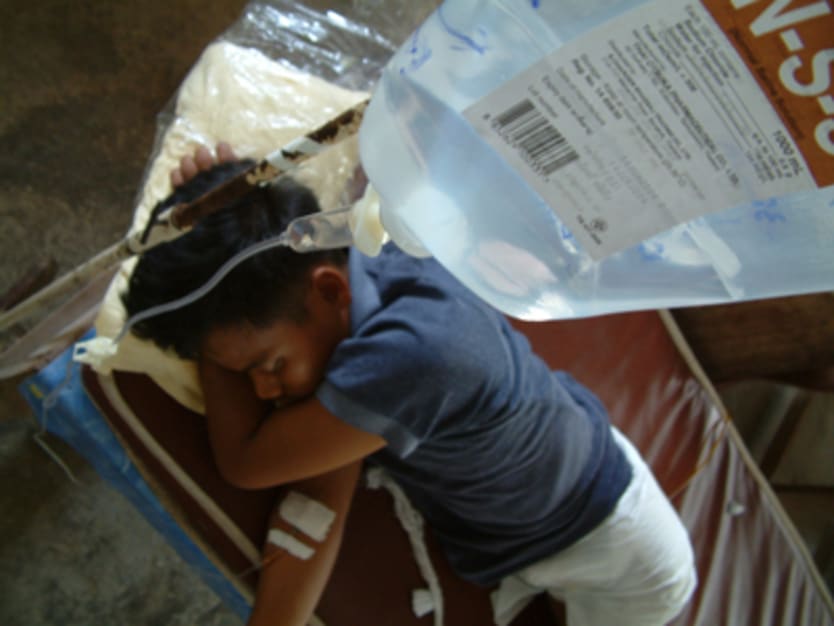
The fight against malaria, one of the world’s most killer diseases, urgently needs an injection of mobile technology.
“Malaria threatens half the globe. By some accounts it has killed more people than any other cause in human history,” Martin Edlund, CEO of Malaria No More, told Devex at the Social Good Summit in New York.
The organization — founded by U.N. special envoy for the disease Ray Chambers — has just launched its new “Power of One” campaign, which links mobile phones around the world with a tracking program for malaria testing and treatment supplies, so individuals can track the impact of their charitable donations.
Edlund is is optimistic about the prospects of eradicating the disease and believes mobile technology can help overcome the “bad” information that has plagued similar initiatives for decades. He also discussed his hopes for a robust replenishment of the Global Fund, a process already underway with major donor announcements in recent weeks.
Here is some excerpts from our conversation in New York:
You are optimistic about the role mobile technology can play in fighting malaria. Why is mobile the missing piece in a global health fight that has gone on for years?
Malaria can be the first disease beaten by mobile. Malaria has always thrived on bad information. Even the word “malaria” is a misnomer. It’s an Italian word that actually means “poisonous or unwholesome air,” because that’s how they thought malaria was transmitted. It wasn’t until 1897 that the guy who would ultimately win the Nobel Prize for this, Dr. Laveran, discovered the parasite from the belly of a mosquito. When you look at the challenges we face in malaria, misinformation is at the core of so many of them. By contrast, good information, enabled by mobile, is how we’re going to solve those problems.
Today, we debuted … a campaign that we call “Power of One.” Every dollar buys and delivers a lifesaving test and malaria treatment to a child in need in Africa. So it’s a really simple consumer proposition.
We’re trying to fill some critical gaps across Africa, starting in Zambia, where our goal is testing and treating 3 million kids for malaria … Through our partnership with the Zambian government and PATHMACEPA … we’re working with 500 community health workers who are reporting on a weekly basis, the number of kids who walk through the door, are tested and treated for malaria.
It’s really about helping people to make an impact in a seamless way, that’s trackable, that you can easily share with friends, and you can see that compounding impact. We have something called your “network impact,” which shows everyone’s effect … In the same way that there’s relentless innovation in Africa around solving problems like counterfeits and stock-outs and health information, we need to be relentlessly devoted here to how we engage the public and shrink the distance between the mobile phone in rural Zambia and the mobile phones that we all use here.
One Achilles heal people might point to — you’re dealing with so many people on a geographically dispersed continent — how rigorous have you had to be in terms of your accountability structures to ensure a dollar really does amount to the kind of impact you say it does?
You only get one chance to win someone over, and you certainly only get one chance to lose someone’s trust. We built the back end of this before we built the front end. We’re working with John Snow International, the world’s leading procurer of malaria tests and treatment, the same group that does all the U.S. government’s, [the U.K. Department for International Development] and the Global Fund’s tests and treatment. We’re able to provide tracking from Novartis, [and] real time in the manufacturing process from JSI, they pick it up and deliver it into the central medical store. And then in Zambia we have the community health workers reporting real-time treatments from the ground … There is one blind spot in that pathway, but it’s after the [supplies] are delivered to the government, who’s guaranteed [delivery] to the rural areas … so we can be sure that every dollar buys and delivers a life-saving test and treatment.
In addition to providing this mobile platform for monetary transfers between individuals and malaria services, what are you looking for at the policy level as the U.N. looks at new development goals and donor countries consider replenishment for the Global Fund?
What’s so innovative about Malaria No More is that we’re trying to solve this problem at the scale of the problem, and that means doing things like the Power of One campaign to engage the public and fill critical gaps, but it also means working hand-in-glove with all of the major funding countries and multinationals.
From a policy standpoint and post-2015, we have to make sure the unfinished business of health gets done. We’re making huge progress … a 33 percent reduction in malaria death on the African continent in the space of ten years, but we’re not going to be done by 2015. So how do we follow through on that historic momentum? How do we ensure that no child dies from a mosquito bite and ultimately sustain that result? It’s no good if you end deaths, but then a year later malaria flares back up. We ultimately have to build the political will, the systems, the information through mobile that’s going to allow us to eradicate malaria.
Ultimately, we need to work with endemic countries themselves to make sure they’re not only doing good for implementers in solving the problems on the ground, but also making the financial commitments to get this done. When we started back in 2006, there was a pretty clear divide between non-endemic countries, donor countries, who were giving money to endemic, recipient countries. In the last six or seven years, we’ve seen the emergence of a variety of middle income countries that are also malaria endemic. So, [we need to know] how … we [can] begin to work with the likes of India, Indonesia, Brazil, to not only be leaders domestically … but also leaders in their regions, because that’s how we’re going to sustain this fight.
Read more development aid news online, and subscribe to The Development Newswire to receive top international development headlines from the world’s leading donors, news sources and opinion leaders — emailed to you FREE every business day.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5








