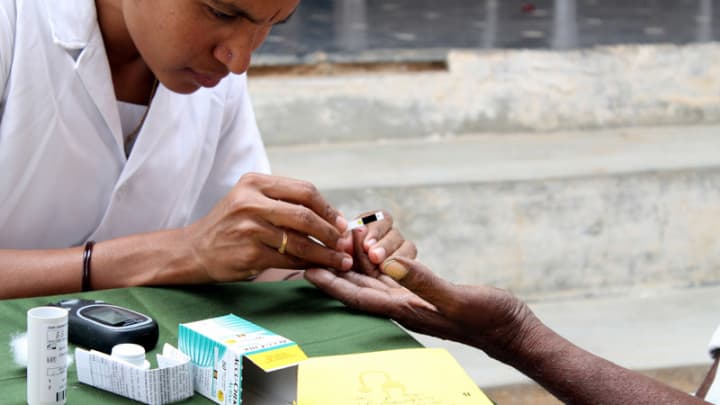
The largest-ever study of national diabetes patterns has uncovered a troubling trend. In the most affluent states, diabetes now mainly affects the urban poor. Diabetes can no longer be thought of as a “wealthy disease.” Rather, as prosperity increases the burden shifts from rich to poor.
The same study also found higher-than-expected rates of diabetes in rural areas. This translates to millions more people who will require care and likely leave the workforce — all of which we simply cannot afford.
Fortunately, there is hope in addressing diabetes by looking to solutions found with tackling other diseases.
The gains we’re making against tuberculosis can be leveraged to improve care for diabetes as well as hypertension, which a third of city dwellers and over half of our doctors live with. Working together with primary care clinics and private sector pharmacists, we can integrate chronic disease care into a growing network of trained health providers who can refer patients and encourage lifestyle changes.
See more related topics:
► Opinion: In India, eliminating tuberculosis isn't just a health issue — it's an economic one
► India turns to private sector to boost health coverage
► Opinion: How technology is helping India move toward smart service delivery
Chennai is showing us the way. Public officials have launched the “TB Free Chennai Initiative” to improve TB care. Their focus has been on drawing in private resources and new partners to forge creative solutions at critical stages of care, from TB screening to service provision and treatment support for the disease. The aim is to bring care as close as possible to where people live and work, making it both simple and affordable.
At present rate, officials expect to eliminate TB in Chennai by the end of the decade.
We must use this model to do the same with diabetes and hypertension. These diseases are taking a toll in Chennai as they are across India. A recent study in Chennai found that 62 percent of the population has diabetes or pre-diabetes, and 1 in every 5 adults over age 20 has some degree of hypertension.
Drawing on global TB gains, here are four lessons we can apply to treating diabetes.
1. Integrate diabetes screening and care into existing networks.
By integrating care for diabetes and hypertension into the TB networks we have built, we can quickly make progress against these diseases. The first step is strengthening referrals pathway in the private sector at the primary health clinic level. Just as with TB, doctors, nurses and health care professionals need training and guidance to spot signs of diabetes and hypertension and refer patients early. Opportunistic screenings must become the norm.
2. Empower pharmacists to talk to patients — or potential patients — about diabetes care.
About 70 percent of Indians seek health care first at the pharmacy. We need to train pharmacists to deliver health care advice on diabetes and hypertension, and encourage people to seek preventive care. A persistent cough might prompt someone to seek care for TB. But a person with diabetes or prediabetes may not even know they are sick. One simple way to solve this is to ensure pharmacists have a glucometer on hand. It’s a moneymaker for the pharmacist and an effective first point of screening. If a high result is present, the person should be encouraged to return for a fasting test, and then potentially be referred for care. For hypertension, having a simple intervention such as a blood pressure cuff on the pharmacy counter would do wonders for catching problems early.
3. Screen for diabetes, hypertension and TB at the same time.
In house-to-house screenings, we should prepare health care professionals to look for all three diseases — diabetes, hypertension and TB — in a single visit. This could also improve TB diagnosis, as it would lessen the stigma associated with screening specifically for TB as opposed to a broader test of health.
4. Support patients navigating the health care landscape.
We must provide assistance to people seeking care. For complex cases in particular, navigating referrals and health care networks can be confusing. Trained support staff can provide direct assistance to patients through informational resources, social support and logistical assistance to ensure they can access all available options as they seek care.
The scale of diabetes and hypertension is daunting. But in Chennai and cities throughout India, we are mobilizing public and private resources to strengthen health care provider networks. We can build on this model by integrating diabetes and hypertension care into these networks, saving millions of lives.
Join the Devex community and access more in-depth analysis, breaking news and business advice — and a host of other services — on international development, humanitarian aid and global health.



