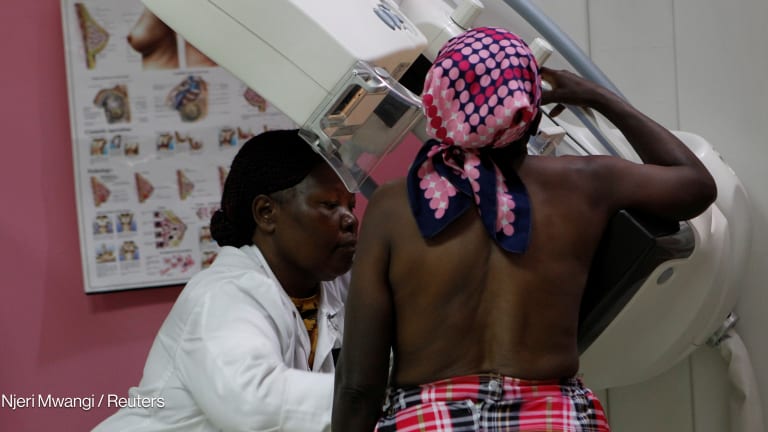
Opinion: 70 percent of cancer deaths happen in developing countries. We need to fix access gaps.
Currently, there are an estimated 8.8 million deaths from cancer every year. Cancer has recently been recognized for the first time by the World Health Organization as the leading cause of global morbidity.
Low- to middle-income countries are bearing the brunt of that burden. Approximately 70 percent of cancer deaths occur in developing countries, which are the most ill-equipped to cope with this burden. The starkest area of inequity relates to childhood cancer — with survival rates over 80 percent in high-income countries and as low as 20 percent in low-income countries. Inequities are also experienced acutely in high- to middle-income countries, particularly within certain demographics, including indigenous, immigrant, refugee, rural, and lower socioeconomic populations.
These inequities are reflected in the rate of premature cancer deaths globally, which the WHO has targeted for a 25 percent reduction by 2025, along with other noncommunicable diseases such as cardiovascular diseases, chronic respiratory diseases, and diabetes. But in order to deliver on this global commitment to decrease the 4.3 million premature deaths from cancer worldwide, the current inequities in risk factor exposure — as well as in access to screening, early detection, and timely and appropriate treatment and care — must be addressed.
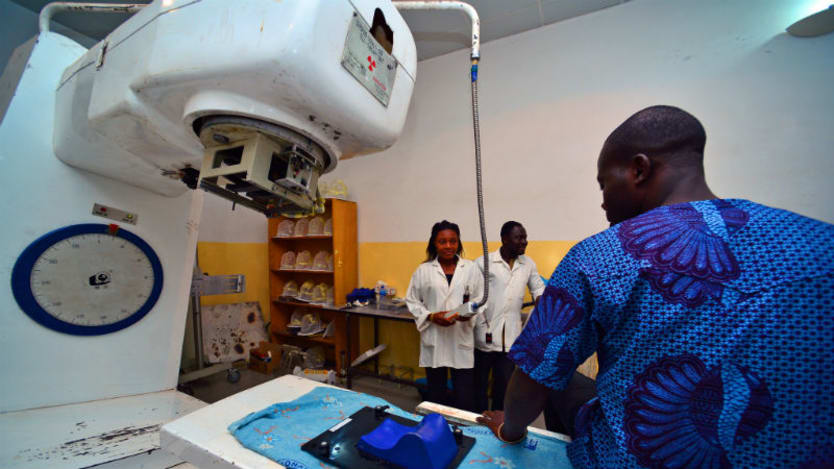
Nowhere is the global gap that affects the underserved and underprivileged more glaring than in access to radiotherapy. As one of the major methods of cancer treatment, radiotherapy is recommended for 52 percent of cancer patients — but 90 percent of cancer patients in low- to middle-income countries lack access to it. Within high-income countries, there are also internal disparities. Depending on where you live in England, patients can face significant variation — anywhere from 20 percent to 70 percent — in accessing Intensity Modulated Radiotherapy, an advanced form of radiotherapy treatment.
Gaps in access to pain relief are equally shocking. Of the 56.2 million people who died in 2015, 45 percent experienced “serious health-related suffering,” primarily due to lack of access to palliative care and pain relief. More than 80 percent of these individuals were from developing regions. The enormous gap between need and availability of opioid analgesics is growing and is increasingly skewed against people living in poverty: The Lancet Commission on Global Access to Palliative Care and Pain Relief estimates that there is a global shortfall of about 48.5 tons of morphine-equivalent opioids, of which the shortfall in low- and middle-income countries accounts for over 99 percent.
If we aim to meet our pledge to avoid so many premature deaths from cancer, a strong committed response from national governments will be key. And that means acknowledging the fact that the cancer burden cannot be alleviated exclusively through prevention to reduce cancer incidence. The tsunami of cancer cases anticipated in the coming decades requires a persuasive and robust response at all levels — global and national — to have any impact on people’s lives.
Treatment for all calls on the international cancer community to address the global equity gap in access to cancer services through strengthening health systems and encouraging governments to improve the provision of information, availability, and access to treatment and care. If one truly believes in the notion that treatment is for all, we need to address the global equity gap in access to cancer services by getting behind four essential pillars of cancer treatment and care:
1. Improving the quality of cancer data for public health use
2. Increasing the number of people with access to early detection and accurate cancer diagnosis
3. Providing timely and quality treatment for early and metastatic disease for all
4. Providing a basic supportive and palliative care service for all
In recent years, we’ve made great progress in putting the business of saving lives and getting people into quality care at the front and center of the political agenda. The inclusion of cancer and noncommunicable diseases in the Sustainable Development Goals in 2015 was a major breakthrough. The successful adoption of a cancer resolution at the World Health Assembly in 2017 was another big step.
We must continue to position cancer in the broader health and development agenda, especially around the issue of universal health coverage, and make the case for cancer to receive adequate funding. These global cancer commitments need to translate into national action. In September, world leaders will gather in New York for a special United Nations High-Level Meeting on NCDs. This is a big moment in global health: Expectations for commitment are high. So are the stakes for the 32.6 million people living with cancer.
Let World Cancer Day draw a line in the sand and let 2018 be known as the year that we began to close the treatment access gap at the national level. Let’s set ourselves firmly on the way to ensuring that at the very least, everyone living with cancer receives basic supportive and palliative care services.
Read more Devex coverage on global health.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5