Opinion: How health care systems designed by and for women can save lives
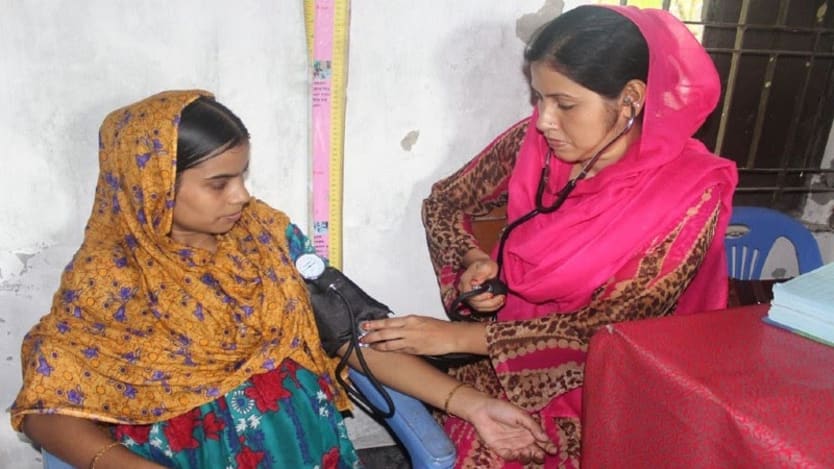
Back in 2010, my mother was hospitalized for a basic operation in Dhaka, Bangladesh. We had no reason to worry. But when she suffered complications, the doctor did not seem to care what our family was going through. He dismissed my mother’s complaints, nearly missing important signs that complications could occur. I knew we had reached an impasse when I had to literally chase the doctor up two flights of stairs to get him to answer my basic questions.
Such dismissiveness is unfortunately all too common in Bangladesh, where the average doctor’s visit lasts 48 seconds. But this story speaks to a deeper problem we have in health care systems across the world: Doctors do not take women seriously.
While individual gender bias plays a role, I see that as a symptom of a much deeper, systemic challenge, which is that health care systems were primarily designed by men. Women account for only 13% of CEOs in health care, and nearly 70% of global health organizations have a man at the helm. This leadership gap creates an empathy gap: How are we to expect male leaders to build systems and invest in solutions that meet the unique health needs of women employees, health care workers, and patients?
The consequences of this design flaw are disparities in health outcomes and poor access to health care for girls and women. In the U.S., women brought to emergency rooms after suffering heart attacks are more likely to die than men in the same situation. In India, only about one-third of women got access to the health care they needed at one of Asia’s biggest hospitals, compared with two-thirds of men.
There is extensive evidence that physicians are more likely to interpret men’s symptoms as “real” and women’s as psychosocial, resulting in women not receiving the same level of care. This is even worse for women of color, who experience intersecting discrimination based on their gender and race.
Since the system was designed by men, most of the medical field is conditioned to equate women’s health with maternal and reproductive health, causing doctors to dismiss some of the other health problems that a woman might face. While deaths during childbirth and postpartum have decreased significantly over the last few decades, those due to noncommunicable diseases such as cardiovascular disease, stroke, and respiratory diseases are now the leading causes of death for women worldwide.
This does not have to be the case. We can build health systems by women and for women.
Starting with “by women,” we simply need more women leading health care companies. Diversity at the top will help improve diversity throughout a business. Companies with female founders hire 2.5 times more women than ones founded by men only. Such diversity improves companies’ financial performance and ensures the health workforce reflects the populations it serves and can bring that perspective to the table. This is not hard to do; my own management team is 40% women, and women are represented at every level of our company, from security guards to doctors to suppliers.
But simply adding more women to the health care field itself will not produce the type of women-centric care needed to close the gap. We need to build care models that listen to women and move beyond the maternal and reproductive health paradigm.
This type of advanced primary care model is starting to take hold in more higher-income countries, which recognize the tremendous health and economic benefits of taking a proactive, whole-person approach to women’s health. One such example is the Tia Women’s Health Clinic, which integrates gynecology, primary care, and wellness into one cohesive experience to provide more continuous care. Evidence shows that this type of integrated care improves patients’ clinical outcomes and satisfaction by enhancing the quality of the doctor-patient relationship and addressing health concerns before they become too severe.
However, it is rare to find this type of care model in lower-income countries, which continue to put women’s health needs in separate boxes, creating a complex maze for women to navigate. My company in Bangladesh aims to move beyond this fractured mentality by providing care for women in interdisciplinary teams, including family health professionals, women’s health experts, health coaches, physiotherapists, and nutritionists. As global health organizations and governments work toward strengthening health systems and improving women’s health, we need them to provide care for women across their life span — in early childhood, through reproductive years, and into later life.
Health care companies can also adopt transformative cultures and systems that support women’s voices and needs. This could include arranging transportation or child care so women have equal opportunity to travel to health care facilities for early morning or evening appointments — because what good is stellar health care if you cannot get to the facility? Additionally, shifting to value-based care can align payments to facilities with women’s health outcomes. If doctors are less worried about billing for services, they can spend more time listening to women and empowering them to manage their health. These practices can be reinforced with workplace training that emphasizes empathy and hospitality so that listening to women becomes the norm, not the exception.
Making these changes will require attention and care from existing health care companies and those who are funding the health care of the future. By elevating women in leadership and treating all women with dignity, we can make sure no one has to run up the stairs to get her doctor’s attention. Instead, we can all thrive on level ground.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5








