The announcement by Facebook that it will no longer allow anti-vaccine advertisements on its platform is welcome as measles cases surge in the U.S. Pacific Northwest and double in Europe. But this measure alone is not enough to address the growing global spread of “vaccine hesitancy” and rising rates of disease and death caused by undervaccination.
Facebook has pledged to address some of the amplifying algorithms and other technical mechanisms that inflate and cluster misleading information. The company also says it is exploring ways to give users more context about vaccines from “expert organizations” — a positive step for those of us focused on the communication of science-based facts.
However, the answer to combating today’s currents of vaccine dissent is far more complex than addressing the needed technical fixes and must be part of a wider effort involving multiple partners, including citizens. If the moves of tech companies are perceived as censorship, they may only harden the views of those who feel they already have no voice.
Communicating noncommunicable diseases
The terms "noncommunicable diseases" or "NCDs" don't exactly lend themselves to snappy and exciting communications campaigns. Devex speaks to experts in the field to find out how to communicate the noncommunicable.
In spite of being among the most effective tools we have to protect people’s health, public confidence in vaccines is under threat as never before. So much so that the World Health Organization recently called out vaccine hesitancy as one of the top 10 threats to global health in 2019.
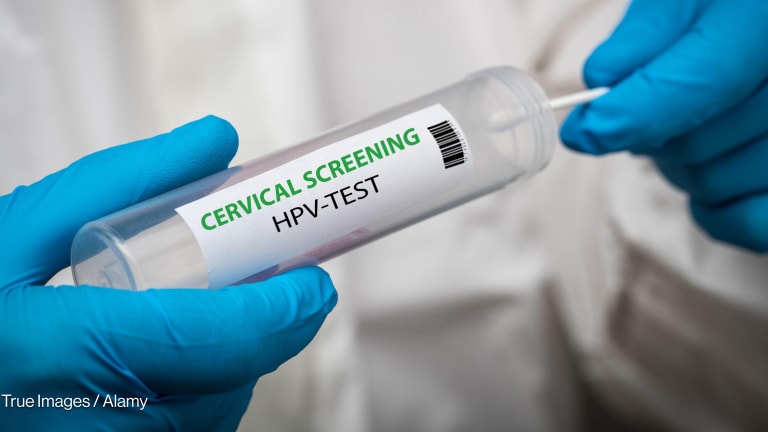
The fallout is being felt worldwide, not just in terms of measles cases. In Japan, young women and their parents are turning away from a vaccine that could prevent cervical cancer, partly due to the health authorities’ hesitating and not standing up for the science and global health consensus on the safety of the human papillomavirus vaccine.
In remote corners of Pakistan and Nigeria, the last handful of polio cases are proving stubbornly resistant due to political and cultural obstacles and are a key obstacle to eradicating polio globally.
For some years now, groups of vaccine questioners and refusers have been connecting via social media networks around the world. This is having an irrefutable impact on public health. The “State of Vaccine Confidence in the EU 2018” report highlights how decisions to delay having vaccines or refusing them altogether are contributing to declining immunization rates in a number of countries and to increases in disease outbreaks.
Clearly, the problem is greater than the role of Facebook and other social media platforms that amplify the spread of negative sentiment. Public anxieties are being driven by a mix of misinformation, distrust in experts and officials, and strong beliefs in alternative health approaches — and we need new modes of engagement rooted in a deeper understanding of the key constituencies and their concerns.
Take time to listen
If we are to change the conversation and start to reverse the negative trend in public trust in vaccination, the first step is actively listening to people’s concerns. Many of these fears come up repeatedly in patient surveys. Are vaccines safe? Are they right for my child? Should I wait to vaccinate or spread the vaccines over a longer period? What about adverse side effects?
Many people say their concerns are not taken seriously by health professionals. That may be because, in a busy health facility, there is little time for discussion. Or it may be because a vaccinator does not have the information to respond. One part of the problem is that anyone with medical or health training finds it hard to understand why people question vaccines at all.
We need to start by being open to discussion and making information available in a language and context relevant to those we are communicating with. Topics such as how the immune system works, how vaccines are developed, and how they work are not widely understood. Too much of the information currently available needs medical training to decipher. On the other hand, many vaccine critics are extremely good at communicating simple ideas using emotive language.
We also need to get much smarter about social media engagement. A lot of the information about vaccines available online is inaccurate or simply wrong. Much of it is not even deliberate misinformation, but misunderstood information. Countering rumors, myths, and falsehoods requires investments of time and technology to engage effectively. This includes communicating transparently around incidents where vaccines have caused adverse effects.
Countries are trying to work out how to provide the right level of leadership and information to mayors, community leaders, teachers, and other respected voices so they can help to listen, build trust, and spread accurate information to counter rumors and myths before they take hold.
New champions are needed who can communicate the importance of immunization at a human and emotional level. Teachers, educational toy companies, social networks, and the music and entertainment industries all have a role to play.
Addressing the role of algorithms in spreading misinformation and anxiety is important, but there is much more that needs to be done to rebuild public trust in vaccines. We should not shut down questions, but hear them.
This demands a greater collaborative effort, bringing together public health professionals, technology experts, and some members of the public to sit around a table, with the best information available, conveyed sensitively, through honest, not manipulated media.
This open and participatory approach is the only way forward in this matter of life and death.