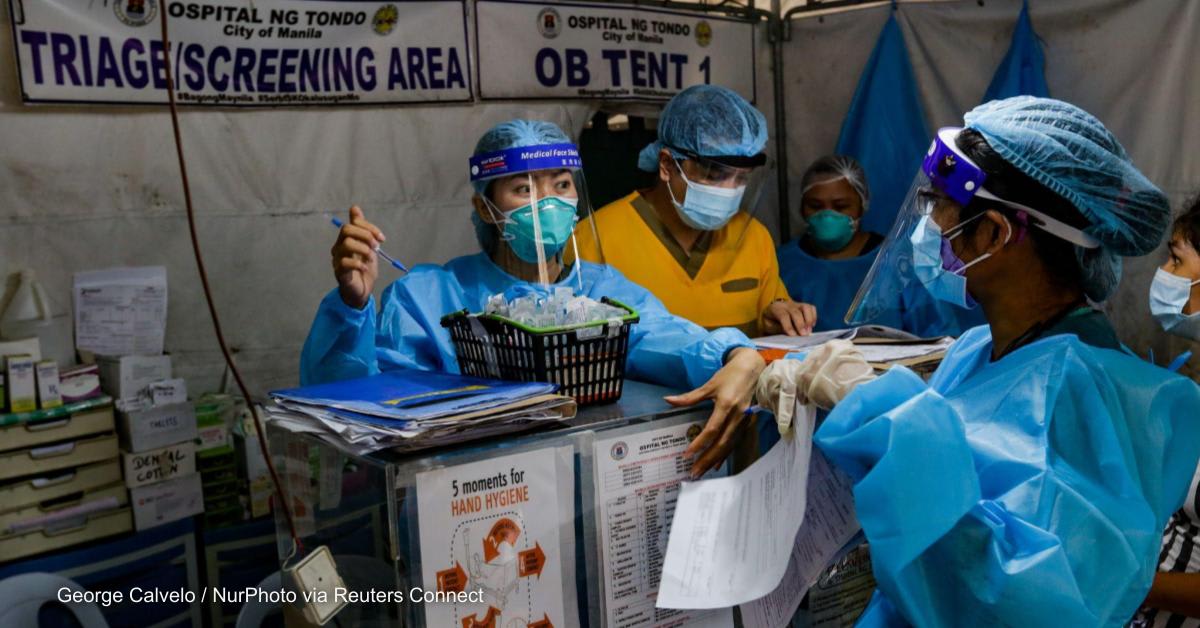
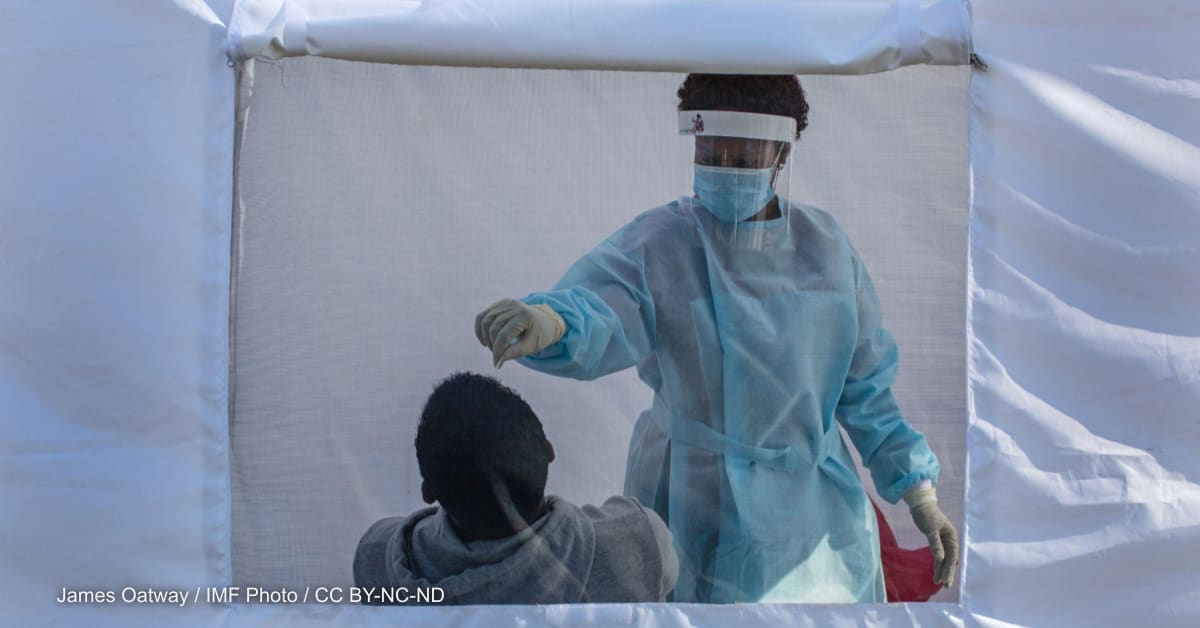
COVID-19 has unmasked shortcomings across the globe by elevating issues that previously lived in silos or underneath the surface. As the pandemic continues to expose vulnerabilities on national and global scales, people everywhere are asking, “Why weren’t we prepared for this?”
In the aftermath of the 2014-2016 Ebola outbreak in West Africa, multiple international expert panels recommended pandemic preparedness reforms that included developing standards and capacities to measure a country’s preparedness level. Guidance was robust and supported by evidence, yet COVID-19 has challenged or undermined these recommendations worldwide since the start of this year.
So instead of asking why the world was not prepared for COVID-19, the global community should be asking, “What does ‘pandemic preparedness’ really mean?”
How has preparedness been measured?
The United Nations says “preparedness” means that the right mechanisms are in place for national authorities, multilaterals, and relief organizations to be aware of risks and deploy staff members and resources quickly once a crisis strikes.
Opinion: As the world battles coronavirus, never let a crisis go to waste
Did we let the HIV, Ebola, SARS, MERS-CoV, Zika, and cholera crises go to waste? In the face of COVID-19, experts weigh in on what an immediate response should look like.
To assess preparedness, the World Health Organization and partners unveiled the “joint external evaluation” process in February 2016 to help countries understand their health security strengths and weaknesses to protect each nation, and the world, from infectious diseases. JEEs are voluntary, objective assessments that review and score 19 areas of epidemic preparedness and response capacity every five years.
The goal of the JEEs, as standardized and internationally accepted evaluations, is to make recommendations for countries to take necessary action to address any gaps. At the end of 2018, 110 countries had completed or planned to complete a JEE.
Established in 2019, the Global Health Security — or GHS — Index, managed by the Nuclear Threat Initiative, the Johns Hopkins Center for Health Security, and The Economist Intelligence Unit, also takes a comprehensive look at preparedness and capacity gaps at national and international levels.
While similar to JEEs, the GHS Index is involuntary, includes more background indicators, reviews government transparency, and looks across six categories to assess a country’s capability to prevent and mitigate pandemics. Currently, the GHS Index has benchmarked health security capabilities across 195 countries.
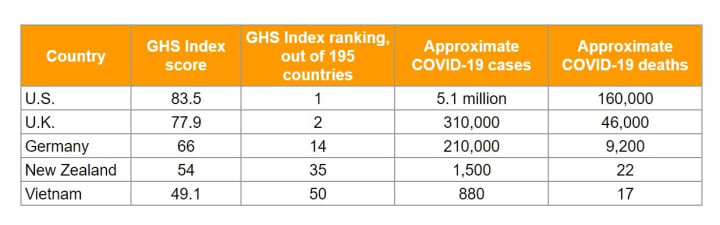
While other sources for measuring preparedness exist, the JEEs and GHS Index are common tools for predicating preparedness capabilities. Yet some of the highest JEE and GHS Index countries — including the U.S. — are leading in coronavirus cases, while countries with lower preparedness scores — like New Zealand — are excelling at managing COVID-19.
What is missing from measuring preparedness?
Current preparedness measures capture capabilities in terms of processes and mechanisms in place at country levels. What they fail to capture is the level of influence that leadership, community support, and trust can have on response measures. Once COVID-19 became a global threat, these factors became impossible to ignore and quickly began shaping how well a country managed COVID-19.
Global leaders have been put to the test nearly as much as health systems during this pandemic. Countries with leaders who have remained transparent and consistent while also using science-based messaging have been able to control domestic COVID-19 cases. More importantly, they were able to engage their populations to adopt new behaviors, such as social distancing and mask-wearing.
Muddled messaging around COVID-19 complicates response in Tanzania
Tanzanian President John Magufuli has repeatedly minimized the risks of COVID-19. This has created a complicated environment for organizations focused on health communications to speak with communities about the ongoing pandemic.
Public confidence in leaders of the early standout countries — including New Zealand, Vietnam, and Germany — has made a tremendous difference in case counts as well as death rates. These leaders responded early, listened to public health officials, and communicated often, which made their populations more willing to adhere to guidelines meant to stop the spread of the coronavirus. These countries now serve as international case studies on how to respond to a health crisis, but not one had a top preparedness score.
In contrast, the U.S. and the U.K. — the countries with the highest preparedness scores — are among the nations with the most COVID-19 cases and deaths. Government leaders have provided inconsistent messages on testing, treatments, and even the severity of the pandemic. National leaders have also not endorsed, accurately messaged, or exemplified public health recommendations. Health systems are continuously undermined by public distrust and uncertainty that swirls across each country.
Despite high marks on preparedness capacities, national response efforts in these two countries are quickly becoming case studies of what not to do.
Reimagining preparedness indicators
COVID-19 response and containment have proven that strong health systems are not enough and that preparedness measures need to go beyond what was previously thought predictive. The global community should come together to rethink how to define and measure preparedness so that it promotes putting people first and building trust across governments and communities. This is the first step to creating a system in which leaders and communities alike can hold each other accountable.
COVID-19 is a stark reminder that the world is only as strong as its weakest link. Coming together with a shared sense of responsibility and commitment to one another is our best chance of building back better.