Opinion: To enable UHC, close COVID-19 testing and gender gaps
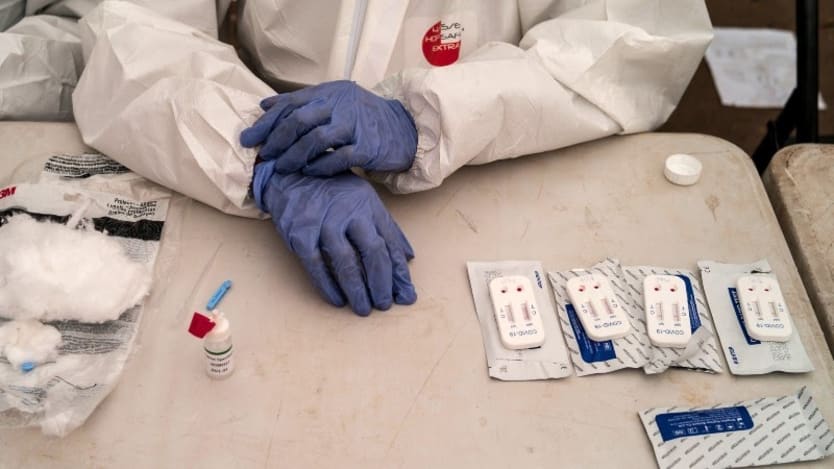
COVID-19 has surfaced longstanding fault lines in the way health care is provided, accessed, and managed.
One of these is inadequate access to testing, which historically has been an afterthought in global health and political agendas, among decision-makers, and even within health care systems. Women’s limited access to testing, in particular, threatens to undermine the global goal of universal health coverage because only accurate diagnosis enables accurate treatment — and the central concept of UHC is that everyone has access to the health care they need.
Enabling women as self-carers, caregivers, health professionals, and political decision-makers will help close the gap in testing, and enable the achievement of UHC for everyone.
—Inadequate testing remains the Achilles heel of the COVID-19 response. There are not enough tests overall, and not enough laboratory capacity to process those we do have, especially in low- and middle-income countries. Simple, affordable, high-quality “rapid” tests — that do not require laboratory processing — are important for the whole world, but would be a game-changer for LMICs.
Even before COVID-19, the greatest gap in disease management had become diagnosis in high- and low-income countries alike.
One study from the U.S. Centers for Disease Control reports “true” COVID-19 seroprevalence in some U.S. states to be between 11 and 24 times the reported rate. For some other diseases, up to 63% of all cases are never diagnosed. Why does this matter? Not only is an accurate diagnosis a prerequisite for appropriate patient management and accurate treatment, it helps reduce unnecessary use of antibiotics, and provides key data to inform health care policy. It also allows surveillance of an epidemic’s trajectory, and the roll-out of a vaccine when one exists. UHC will not be achieved without closing the testing gap.
This article is part of Focus on: Gender Data
This focus area, powered by UN Women, highlights how data is being used to inform policy and advocacy to advance gender equality. Gender data is crucial to make every woman and girl count.
Gender inequalities magnify testing inequalities, while gaps in access to testing threaten the health and lives of women and adolescent girls. For women, accessing testing can be especially hard, because health systems do not enable testing services in places and in ways women can access them.
Right now, only 52 countries out of 194 are reporting sex-disaggregated data on COVID-19 infections and mortality. Moreover, of countries reporting full and partial data, 14 countries report 70% or more infections in men and 5 countries report over 80% of infections in men. In conflict-affected and fragile states such as Afghanistan, Central African Republic, Chad, Pakistan, Somalia, and Yemen, less than 30% of reported COVID-19 cases were women, compared with a global average of around 50%.
These figures suggest that more infections in men are being recorded because men have more access to testing, which, in turn, suggests women may not receive the treatment they need and women’s deaths from COVID-19 are being under-reported.
The social and economic barriers impeding women’s access, in all settings, are complex. The poorest women may face obstacles such as needing a male relative’s permission to leave home, not being able to afford transport to a clinic, or may be afraid of a confirmed diagnosis because they cannot afford treatment anyway. Without the data, however, the story ends there.
Women are the ones in the engine room of our global, local, and community health systems.
—The foot soldiers in the COVID-19 crisis and the people who drive health systems are women: they make up 80% of nurses globally, 90% of social care workers, and 70% of the global health workforce overall, suggesting fewer women than men at the physician level. Yet women occupy only 25% of decision-making roles in global health.
This means that women are disproportionately directly at risk during and after a health crisis — and indeed, data from UN Women shows that in some countries, COVID-19 infections among female health workers are twice that of their male counterparts.
Yet while the rate of infection for women in some countries is higher than for men, more men are dying from COVID-19 than women, partly because of behavioral risks such as tobacco use, and partly from biological causes we have yet to understand.
Without gender-responsive data, “we leave critical clues on the table,” U.N. researchers have pointed out. If women have higher infection rates but greater survival, women’s immune responses could provide insights into treatment and vaccine development. But in research and development — and historically — women are underrepresented.
We need to understand this better. We need better data, and we need sex-disaggregated data, which is scarce. For many other major diseases, sex-disaggregated data on testing gaps mostly does not exist or is not reported internationally. Public and global health policies have typically not emphasized the gendered impacts of disease outbreaks. Only by fully understanding how COVID-19, or any health condition, is impacted by gender medically, socially, and economically, will we be on our way to building an effective, comprehensive response — for COVID-19, and for health overall.
As countries implement their commitments to UHC, it is critical that we close the testing and gender data gaps, by investing in equitable access to testing. Although women, as health systems users, have less access to services, women can drive change in health systems, politics, and their communities.
The Foundation for Innovative New Diagnostics and Women in Global Health are partnering on a study on testing, women's empowerment, and UHC, to break down the barriers preventing women from accessing testing and countries from achieving universal health coverage targets. The first high-level consultation event took place on Tuesday, July 14, with a report due to be published in late 2020.
Recognizing the complex relationship between health issues, including disease outbreaks, and gender is a cornerstone of creating effective, equitable policies and interventions. Equal gender representation in health and political decision-making roles is another. This is not just a moral imperative — it is about efficacy and pragmatism.
This enormous, but low-profile, task risks getting side-lined while the world’s attention is on seemingly more pressing issues. But the facts should be persuasive: women are the ones in the engine room of our global, local, and community health systems.
For everyone to be healthy and cared for, we need to ensure women are healthy and cared for. And we need to ensure women, as experts in health systems, have equal access to decision making in health. Enabling women as self-carers, caregivers, health professionals, and political decision-makers will help close the gap in testing, and enable the achievement of UHC for everyone.
Devex, with support from our partner UN Women, is exploring how data is being used to inform policy and advocacy to advance gender equality. Gender data is crucial to make every woman and girl count. Visit the Focus on: Gender Data page for more. Disclaimer: The views in this article do not necessarily represent the views of UN Women.

Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5









