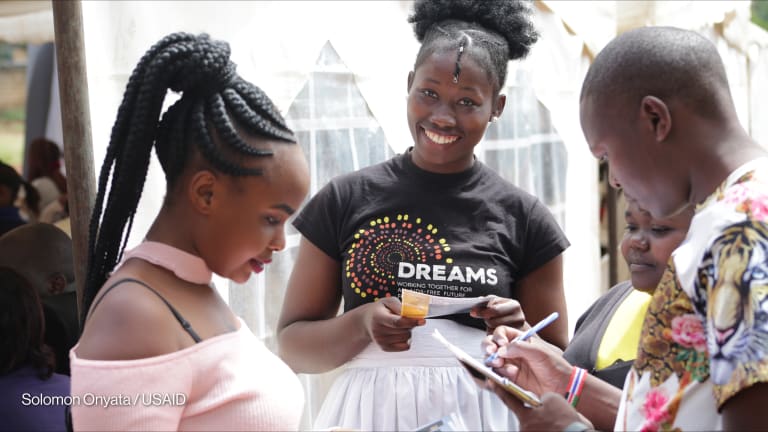
As we approach 2020 — a pivotal year on many levels — we have more options and a clearer picture than ever of what must be done to end the HIV epidemic globally.
But in 2019 we learned some hard lessons about how far we still have to go: a range of prevention trials brought new data on both the potential and the limitations of biomedical strategies in the global HIV response. The data wasn’t necessarily surprising, but it put the obstacles we still face in stark relief.
New data shows that community-wide HIV testing, followed by treatment for people living with HIV, has health benefits for the individual and reduces the incidence of HIV by up to 30%. That is both invaluable and insufficient to end epidemic levels of new infections.
We learned that among general populations of women seeking family planning services in east and southern Africa, HIV incidence is far higher than we thought. Research in South Africa confirmed that young women today often prioritize the need for pregnancy prevention and take a more passive approach to HIV prevention.
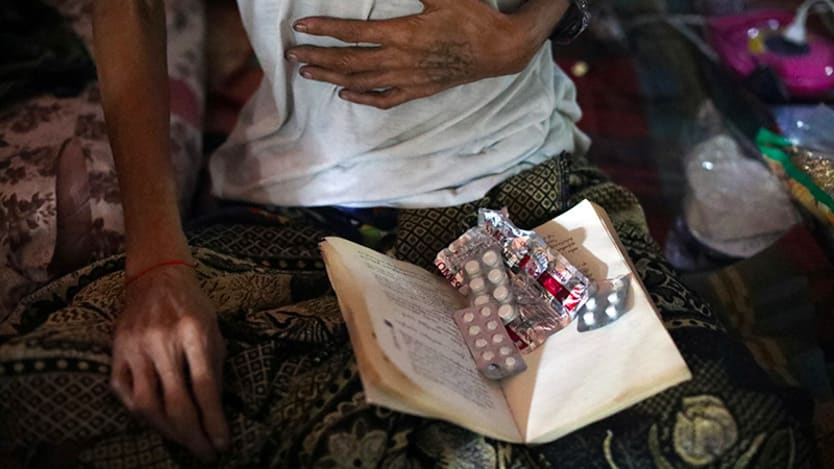
HIV treatment access isn't rising fast enough to reach 2020 targets, UNAIDS report shows
Community engagement is key to boosting the number of people receiving treatment for HIV and slowing progress of new infections, UNAIDS shows in a report ahead of World AIDS Day.
All of this underscores the critical need for family planning and HIV prevention services to work together — delivered in the same place at the same time, and eventually in the same product — to better meet women’s real-world needs.
2020 is the deadline that UNAIDS set for reducing new HIV infections to fewer than 500,000 worldwide. However, in 2018 alone, 1.7 million people became newly infected with HIV.
It is time — in fact, well past time — to redouble efforts and investments in HIV prevention. The need is clear. In sub-Saharan Africa, adolescent girls and young women are 5 to 14 times more likely to be infected with HIV than their male peers.
PEPFAR’s DREAMS partnership that focuses on adolescent girls and young women in specific regions of priority countries is using multilayered biomedical, behavioral, and structural interventions to address the many factors that make girls and young women particularly vulnerable to HIV. But this is just the beginning.
Now what?
In a new report entitled “Now What?," AVAC is calling on the global community — from researchers to funders to advocates — to double-down and advance an agenda for multilayered prevention that supports access to primary HIV prevention — helping uninfected individuals prevent HIV; integrates sexual and reproductive health information and services; and confronts the social and structural barriers that block the way to prevention for those who need it most.
Today, to be young, female, black, and having sex in a high-prevalence sub-Saharan setting is to be at risk of HIV. To be gay or transgender in Africa or the United States — and many other places around the world — is to be at risk of being murdered, harassed, or physically violated. People who use drugs are criminalized, excluded from care, and denied human rights and access to highly effective harm-reduction strategies.
The number of young people in sub-Saharan Africa is increasing dramatically — as it is worldwide. With such large numbers of youth, the absolute numbers of new HIV infections in this age group will be similar to, or even larger than, those earlier in the epidemic. Without prevention that fits into the lives of young people living with and at risk of HIV, there will be no end to epidemic levels of new infections.
The good news is there are energized, committed new leaders in this fight: 2020 is the year of diverse, brave activist leadership in HIV — from the grassroots to Geneva.
For example, over the past decade, AVAC’s advocacy fellows program has supported promising and powerful advocates to design and implement advocacy campaigns that advance HIV prevention research and implementation in their countries and communities.
These fellows, along with the Africa Free of New HIV Infections youth cohort, DREAMS ambassadors, and numerous other leading community voices, have been responsible for advancing policy for the implementation of voluntary medical male circumcision, testing, pre-exposure prophylaxis and treatment, as well as informing gender and key and vulnerable population-sensitive HIV programs and research.
The appointment this year of UNAIDS Executive Director Winnie Byanyima gives us significant hope. In her first week on the job, she spoke about AIDS as a human rights issue and noted the role of “intersecting inequalities, such as gender, age, sexual orientation, race and ethnicity, that are at the root of the higher vulnerability to HIV of women, girls, and key populations.” And one of her first actions as executive director was an important one: meeting with young women affected by HIV.
We urge Ms. Byanyima to continue to stand strong as an activist leader — brave, clear, and unwavering in her commitment to the populations in greatest need of attention. We enthusiastically support a comprehensive and ambitious agenda for addressing unmet goals in HIV prevention. Ending AIDS demands nothing less.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5