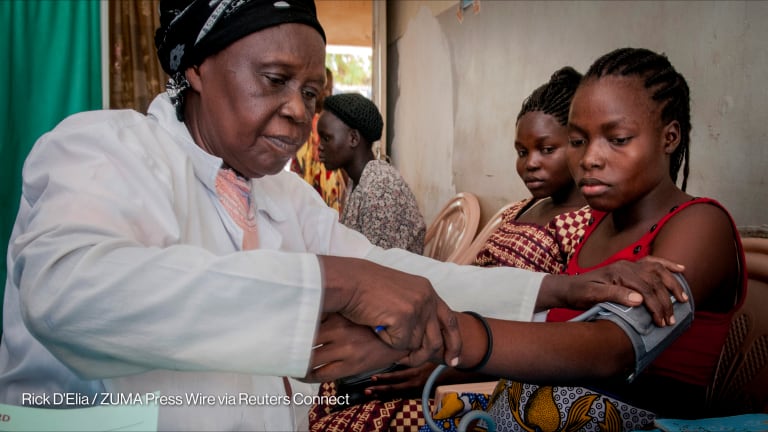Opinion: When incremental change is not enough — dismantling institutionalized racism in health care systems

Although illness does not discriminate, health care systems do by design.
Systemic racism is a global health crisis when people living in resource-poor areas lack access to basic health care after billions of dollars have been invested in international health assistance and when, even in the most resource-accessible nations, race may be the biggest barrier to a long and healthy life.
Health care systems often struggle with putting their intentions into action because goals such as “dismantling systemic racism” and “decolonizing global health” can feel like ambiguous endeavors. While the cry for social justice was always there, now more than ever it seems like health care institutions are listening but failing to respond aggressively in pursuit of a global effort to topple white supremacy.
Opinion: We must translate anti-racism statements into action
This op-ed examines the action and structural changes needed at senior leadership level, drawing on experiences of racism from working at the headquarters of two white-dominated development organizations.
Global problems need global solutions focused on processes instead of on people. Equity, diversity, and inclusion solutions solely for fixing people will never tap into the root cause because it is an issue of institutionalized processes. It is deeper than an individual’s personal intent; the lens of institutionalized racism targets the institutionalized processes in which we all operate as the cause of inequitable outcomes.
We can measure the structural determinants of health globally by the 36-year gap in life expectancy between countries. Health care systems claiming to provide quality care, but in fact prolonging the cycle of inequitable health outcomes, have sold a false narrative to themselves and the communities and made their systems unsustainable.
This is because health care institutions that claim a process-improvement approach to solving these problems perpetuate the “golden thread” of white privilege that created the outcomes we are experiencing today.
Process improvement implies that the core elements of a process are salvageable and, with subtle shifts in the way things are done, you can improve the results. When Black, Indigenous, and people-of-color communities are disproportionately affected by COVID-19 globally, a focus on process design, instead of process improvement, is the only way to dismantle systemic racism — because incremental change is not enough.
Take a process-minded approach
A process is a measurable structure for action with a repeatable and documented order of work activities. Health care delivery is a complex system of micro and macro processes — some designed with intention and others not. Either way, data follows processes, so to impact results, we must take a process-minded approach to understanding the silent systems that divide us.
Engaging in a transparent conversation with patients opens opportunities to create new paradigms for quality, equitable care.
—For example, your job is to manage the production of the highest-quality coffee at the new local cafe. From your perspective, the best cup of coffee has cream and sugar, so you craft the process around this taste. However, you receive mixed reviews, which demand a wider investigation.
As the decision-maker, you have two options: to optimize the process you already have or to start again from scratch with a wider lens on what better benefits your customer.
Optimizing the existing process, in this instance, would be to ask for the recommendations of a group of the best baristas known for their cream-and-sugar coffee, who might suggest you offer a nondairy alternative. You implement these incremental changes but still do not meet all of your customers’ needs — some of whom have to go without.
Alternatively, ask for the recommendations of a group of customers — some like their coffee black and others prefer tea. You engage the customer group in designing a new menu to provide the right product for the right customer every time. It was difficult work to reimagine the traditionally produced cup of coffee but worth the effort, because even with incremental improvements, you would never have met the needs of the broader group of customers.
Designing for equity challenges the assumption that all patients want the same thing. Engaging in a transparent conversation with patients opens opportunities to create new paradigms for quality, equitable care.
Mosaic of leadership should match that of communities
Process-minded health care leaders are critical to this design work by mobilizing their workforce and collaborating with patients in a results-driven way. For solidarity in design, the mosaic of leadership should match that of the communities served.
Within health care, many of the processes driving inequities were designed by and for those that are benefiting the most. Process design requires capturing the voice of the customer, defining what matters most to them, and constructing processes to best meet those needs.
If you are wondering how systemic racism is prevalent in health care globally, look back at who was at the table influencing decisions regarding processes during infancy, implementation, and cycles of improvement. It is unlikely that diversity of thought was considered or patients directly consulted. Then snowball those voices over time, and that brings us to our current reality, because we struggle to decolonize global health by calling out inequitable processes at their core.
Is COVID-19 magnifying colonial attitudes in global health?
As countries around the world struggle to contain the coronavirus, inequalities brought about by existing imbalanced power structures are resurfacing, resulting in growing calls to decolonize global health.
If we do not start getting comfortable with the uncomfortable, future global health leaders will continue to inherit processes that do not value all lives equally and will be tasked with managing discriminatory outcomes, regardless of their personal intent for equity. Academic and training institutes need to better champion these equitable processes within their curricula to nurture a new generation of leaders capable of designing from the patient perspective.
The University of Global Health Equity, a global health sciences university in Rwanda, is just one institution prioritizing these skills. These are not seen as add-ons but as critical elements of a health professional’s path to building, maintaining, and repairing systems that address social injustices such as systemic racism for a more sustainable, equity-driven future.
Engage in a transparent conversation
Process improvement in its most pedestrian application can be translated into practice by simply asking, “How are we currently doing?” Process design challenges us by asking: “Is incremental change enough? And if not, what should we be doing?”
The only way to answer those questions is to engage in a transparent conversation with the patients we serve. We mustn’t be color-neutral in the pursuit of quality care or avoid the importance of race during these critical conversations.
Design work is appropriately messy because it requires participation from the patient and a willingness from health care leaders to intimately listen and build trust. For truly patient-centric care, the patient should be invited to and engaged as part of the design team. Through building relationships, we can challenge the transactional paradigm of health care delivery when patients can directly fact-check assumptions.
The good news? We are not beyond reversal. Since we constructed this paradigm, we are empowered to do better designing for quality by not whitewashing the voice of the potential patient. By doing this, we can design a system that does not discriminate, and we can remove race as a barrier to a long and healthy life.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5