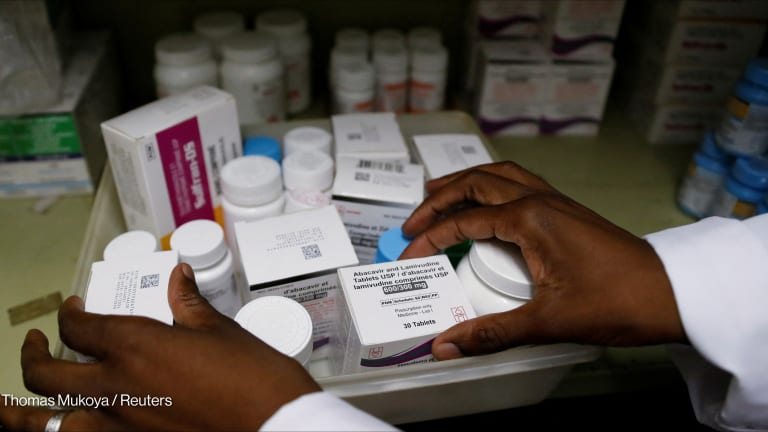
Mozambique is at the outset of recalibrating its HIV response, following a global shift in approach by one of the primary donors to the country’s AIDS response — the U.S. President’s Emergency Plan for AIDS Relief.
Across the 40 countries and regions it supports, PEPFAR’s new strategy calls for a massive scale up in services in areas where the most new HIV infections are happening. Along with the Global Fund to Fight AIDS, Tuberculosis and Malaria, PEPFAR underwrites the bulk of Mozambique’s HIV activities, which means the new strategy will have a significant influence on the country’s efforts to fight the virus.
Based on an extensive analysis of public health data, the PEPFAR team in Mozambique prioritized 77 of the country’s 148 districts they expect to generate the most new HIV patients. The goal, officials said, is to dramatically curb transmissions in those districts in a bid to bring the country’s larger epidemic — one of the worst in the world — under control. The strategy offers the best opportunity, within current international funding constraints, to finally get ahead of Mozambique’s epidemic, according to officials.