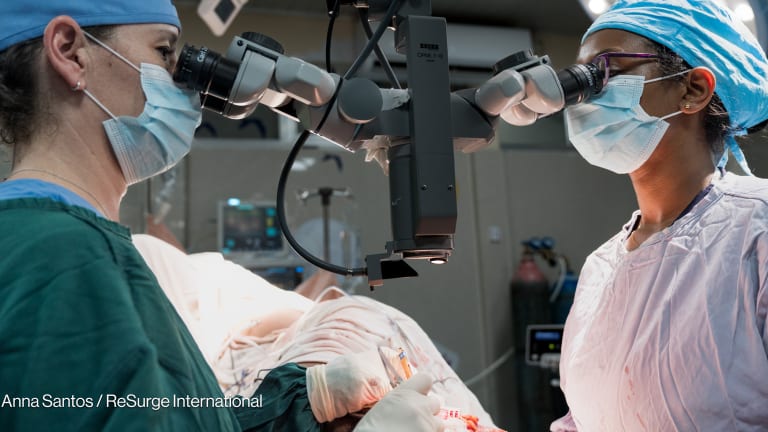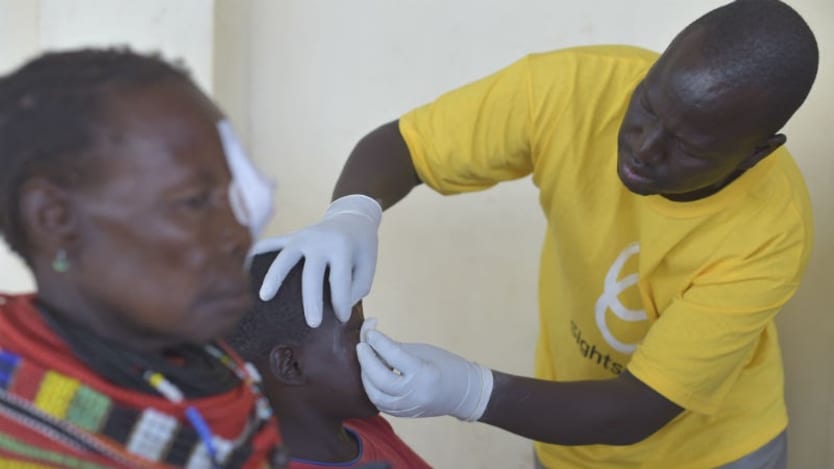
BARCELONA — Trachoma, a painful bacterial infection that turns eyelashes inward, is the world’s leading infectious cause of blindness. Transmitted through personal contact and certain species of flies, it affects over 30% of people living in arid and semiarid areas of Kenya.
“Eye care is not considered as immediate. People want to deal with epidemics [instead].”
— Samson Lokele, eye focal person for Turkana county, SightsaversWhile antibiotics can treat trachoma in the early stages, in the latter stages — before the scarring and in-turned eyelashes cause permanent damage — surgery is the only solution. Yet this isn’t always an option for people living miles from eye health services.
More on vision:
► 5 misconceptions preventing progress in eye health
► Results in rural India offer window into what works to fight blindness
“Many people struggle to get the surgery they need, either due to lack of knowledge that the help is out there or because the path to the hospital is long and treacherous,” said Samson Lokele, a Sightsavers eye surgeon who travels to mountainous and remote areas within Kenya, Uganda, and South Sudan to find people in need of such care.
The surgery is quick, straightforward, and possible to do anywhere, Lokele said, adding that he’s done the procedure under trees and in the backs of cars. “We do surgery wherever the patients are, wherever we find them — even in their homes,” he said.
The first eye surgeon in Kenya’s Turkana county — which has a population of 1 million — Lokele has performed eye surgery on more than 3,500 trachoma patients since 2010 and says the process involves preparation and education.
Speaking to Devex, Lokele described how a typical day begins with outreach to people with potential eye problems. This involves visiting communities where food and water are scarce and living conditions can be unhygienic, allowing flies — which carry the disease — to multiply.
When a patient with trachoma is identified, mobilization happens fast, and “on a surgery day, the patient is cleaned, dressed, and then taken in for surgery, which takes around 15 minutes,” Lokele said. This is followed by a period of postoperative care, including medicine for pain relief and for trachoma.
As well as explaining the conditions he faces, Lokele discussed what more could be done to ensure those living in rural areas aren’t abandoned when it comes to tackling treatable eye conditions.
This conversation has been edited for length and clarity.
Why is trachoma so prevalent in these rural communities?
We did a trachoma survey in 2010 where we found that the prevalence of trachoma in Turkana county was 42.3% in children. This became a public health problem, so we had to employ the World Health Organization’s SAFE strategy [for surgery for trichiasis, antibiotics, facial cleanliness, and environmental improvement]. We started giving people antibiotics and doing surgeries and outreach. We had a backlog of around 11,000 people, and last year we finally cleared our backlog. In 2017, trachoma dropped down to 9.9% [according to figures from Sightsavers and the Ministry of Health].
We have also put strategies in place to ensure that people are found. We have opened eye clinics in various parts of Turkana and trained around 64 people to ensure when they find these cases they can operate on them. We are also doing surveillance where any case found is reported to us immediately for action.
In some of the more rural areas, what do people do if they have trachoma and need surgery?
It's not easy to do surgeries on these patients because you need equipment and a good setup with infrastructure. These people stay far from hospitals, which is one of the biggest problems, and the human resources are very difficult to get. Then there's the cost. People are not able to meet costs, and therefore they like it for free.
And you can get a patient with an eye problem who refuses treatment, and it becomes an issue. With proper communication skills, health education can improve the issue. Health becomes important to them if we [educate] them.
In urbanized areas, whenever people feel an illness, they go to hospital. Here, they focus on the animal. If the animal is OK, they are also OK, and therefore they don't go to hospital.

What are the biggest challenges of doing surgery in isolated and rural communities?
There are many challenges to helping people in isolated and rural communities.
Resources: Mapping out where the people are who need help, organizing outreach, and getting treatment or surgery to them takes time and resources that aren’t always readily available.
Travel and terrain: Getting to isolated communities can be dangerous. I’ve lost count of the amount of times my car has been stuck in mud or sand. We once got stuck when crossing a river and had to send a team member to walk more than 100 kilometers to get help. Sometimes you have to go as far as you can, then get the communities to come to you.
Nomadic tribes: These tribes move around a lot, which makes them hard to treat. Sometimes when we come back to help them, they have already moved on, so we need to track their movements.
Cost: People will pay to keep their animals healthy, but not pay to heal their own ailments. But after many years of education, advocacy, and social communication, this attitude is slowly changing.
Conflict: As doctors, we are unarmed so cannot go places where there is conflict. Many rural communities fight or steal resources, so we organize peace caravans to help change this. Peace caravans allow us to work closely with community leaders, peace nongovernmental organizations, ministries of health, and students, who travel to the villages and tell them the disadvantages of fighting. They help return stolen livestock and teach them how to farm and irrigate. They also explain that until there is peace, no doctors can come to treat them.
What more do you think is needed by others in the global health community to tackle these challenges and improve access to eye health services like trachoma surgery?
The first thing is purely infrastructure — taking health to them. We put up facilities and equip the nearby places they can reach, or we do an outreach program that can reach them or give them health education. Also, we encourage them to use toilets instead of defecating in the open, and we try to control flies because they spread the disease.
I think we need to discuss this with governments and advocate for support in terms of resources and funds. Eye care is not considered as immediate. People want to deal with epidemics [instead].
Devex, with financial support from our partner Essilor, is exploring challenges, solutions, and innovations in eye care and vision. Visit the Focus on: Vision page for more.