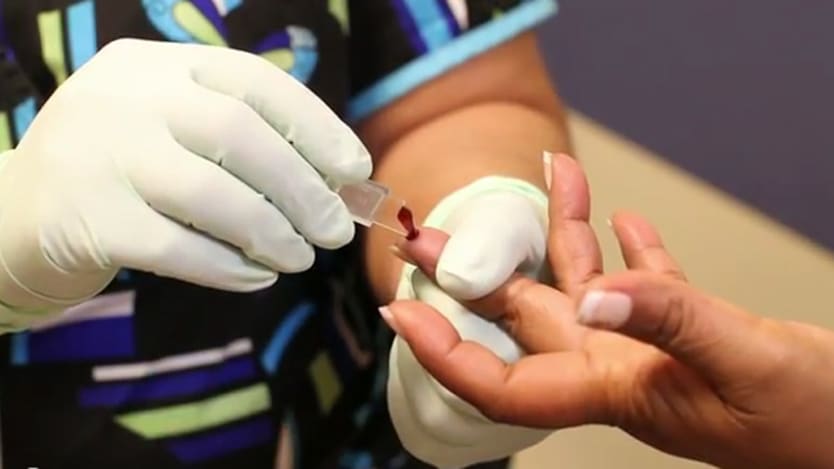
Progress in the fight against HIV/AIDS has allowed people living with HIV who have access to antiretroviral treatment, or ART, to live longer, healthier lives. Yet as the disease evolves into a chronic one, patients are more likely to suffer other health issues.
Noncommunicable diseases, chiefly cardiovascular diseases, cancers, respiratory diseases, and diabetes, are now responsible for 80 percent of “premature” deaths — occurring between the ages of 30-69 — in low- and middle-income countries. Due to the inflammatory effects of HIV, the side effects of ART, and the consequences of aging, people living with HIV appear to be at a higher risk of developing NCDs, especially considering that some HIV medicines can increase blood glucose levels and lead to diabetes.
This means the fight against HIV/AIDS must now take into account the increasing prevalence of NCDs — as well as tuberculosis and anemia — to keep patients as healthy as possible. Yet in countries where health systems are lagging, getting screened and treated for NCDs remains out of reach for many patients.
However, what could be seen as a challenge may also represent an opportunity to leverage the infrastructure and systems — for example, supply chains, training of health care practitioners, availability of diagnostics medicines, and more — that have successfully been set up in developing countries over the past decades to prevent, screen, and treat HIV, and to deliver high-impact interventions for other diseases at the primary health care level.
“Although there are unanswered questions about the best way to integrate HIV and NCD services, the major barrier to integration is the lack of access for NCD diagnosis and treatment.”
— Miriam Rabkin, director for health systems strategies, ICAP Columbia“The investment and hard work on the part of donors, ministries of health, health workers, and communities has helped to create a highly functional system with which to deliver chronic HIV care, and this has the potential to support chronic disease services more generally,” said Miriam Rabkin, director for health systems strategies at ICAP Columbia and associate professor of medicine and epidemiology at Columbia University's Mailman School of Public Health, in an interview with Devex.
Finding new models of care and benchmarking what works
In 2011,the Joint United Nations Programme on HIV/AIDS recognized the need to integrate the responses to HIV and NCDs. In 2015, the World Health Organization called for universal access to HIV treatment, aligning with its 2016 framework on integrated, people-centered health services, and its Global Health Sector Strategy on HIV 2016-2021.
All of these frameworks come in support of Sustainable Development Goal 3 on achieving universal health coverage, and encourage better coordination of different health systems and services that a patient living with HIV might be accessing in the course of their treatment — for instance primary care, maternal, newborn and child care, emergency care and, of course, HIV care.
How to put these guidelines into practice has been less clear. In 2017, a team of researchers conducted a study comparing existing services integrating HIV and NCDs in Kenya, Nigeria, Uganda, Zambia, Tanzania, Cambodia, Malawi, and Lesotho. In some cases, NCD care had been incorporated into HIV care centers. In others, HIV care had been streamlined into primary health care services. A third scenario involved creating brand new services incorporating both HIV and NCD care. All of them encountered both varying degrees of challenges and successes regarding supply chain management, staff training, services coordination, and monitoring and evaluation, according to the local context.
In Malawi, nonprofit health care organization Partners in Health has been running programs out of 10 rural health centers in the district of Neno, including highly successful HIV/AIDS services. Yet the health centers were facing a surge of patients suffering from undiagnosed or untreated NCDs.
“We were really feeling this need to rapidly increase access to NCD care,” recalled Emily Wroe, Partners In Health’s chief medical officer in Malawi. “We knew we weren’t going to be able to make a new vertical program to get out to the health centers. We couldn't hire a whole new team. So [we asked ourselves], what exists already that we can take advantage of?”
See more stories:
► AIDS 2018 told the story of a global health crisis
► The funding dilemma for noncommunicable diseases in Africa
In 2015, PIH began offering chronic care services addressing NCDs in its health centers, making use of well-functioning systems put in place for HIV/AIDS, such as data systems for patient follow-up, and supply chains. Local staff members have received additional training, and have been supplemented by hospital-based staff, who travel to the health centers a few days a week. All patients attending local health centers are now tested and screened for a variety of conditions, including HIV, tuberculosis and diabetes. According to Wroe, these measures have brought retention rates of chronic NCD patients in Neno from less than half to over 90 percent.
“The benefit, in our setting, of integrated chronic care like this, is really at the primary care level. It's pushing services where a patient only needs to walk for 40 minutes to get their drugs instead of four hours,” Wroe explained, adding that the specifics of this program were entirely dependent on the local context and needs.
In a separate study conducted in Swaziland, Rabkin and her team at ICAP measured the impact of screening HIV patients for cardiovascular risk factors, namely hypertension, diabetes, hyperlipidemia, and tobacco smoking, during routine HIV visits. The study showed that screening increased visit length, but also identified large numbers of HIV patients with cardiovascular risk factors. Both patients and clinicians favored the added services, and Rabkin noted that the challenges, management of staff and space, may be outweighed by the benefits of diagnosing patients early.
“The more people you diagnose and treat early, the fewer people who are going to have complications and need to go to subspecialty or inpatient care,” said Rabkin.
This model may work well in Swaziland, which has the highest HIV prevalence in the world — 27.2 percent of adults aged between 15-49 as of 2016 — and where using HIV as an entry point for delivering a broader range of health services has the potential of reaching a great number of people. However, it may not be as efficient in countries with lower rates of HIV such as Ethiopia, which has a 1.1 percent prevalence rate, and emphasizes that each model needs to be tailored to the local context.
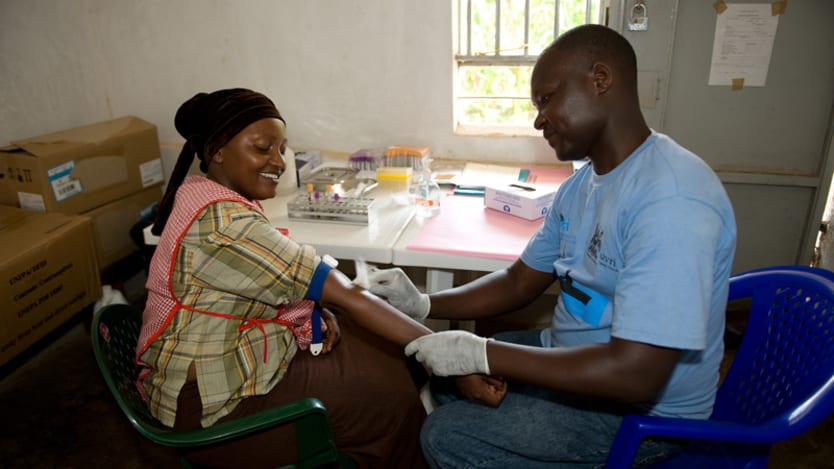
Embracing innovation by addressing a need, not creating it
There are myriad reasons to remain optimistic, however. HemoCue, a Swedish company, manufactures diagnostic solutions that address anemia and diabetes, shortens testing time, allows for accurate point-of-care testing, and decreases the cost of diagnosis. This is because test results are delivered on site, rather than by a laboratory adding convenience for the patient and improved workflow for the health teams.
Technological innovations like these can improve access to diagnosis and treatment while increasing the government’s capacity to conduct surveys and collect accurate, timely data, as well as allowing for cost-efficient patient care.
“The way testing is done must be adapted to local context,” said Dean Garrett, biomarker and laboratory adviser for the Demographic and Health Services program at ICF International, a global consulting and technology services company. “There needs to be a new way of interaction between diagnostic companies in the developed world and the developing world. We can't just make a test and expect it will be used in the same way it’s used in developed countries.”
HemoCue’s products are said to be robust enough for use in harsh environments and remote areas, which also make them suited for use in the world’s least-developed countries, allowing the same high-level of quality as is being used in developed countries.
The company sees its role beyond that of a manufacturer. It has launched Embrace Health, an initiative run in partnership with local authorities in southern Africa, as well as local and international NGOs, to treat anemia. By doing so, HemoCue hopes to amplify the work being done at the intersection of NCDs and HIV care to have an impact across the board in the field of primary care services.
With partnerships such as these, technology, and know how, adequate prevention, screening, and care can be delivered and incorporated in what is already being done at the primary health care level.
“By taking many of the priority health care areas into consideration such as the malaria program, maternal and child care programs and HIV care, all these intersect at the primary health care level” said Evan Herbst, regional sales director for HemoCue in South Africa. “And that’s where we can have an impact on many more people, because that's where the real work often happens.”
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5








