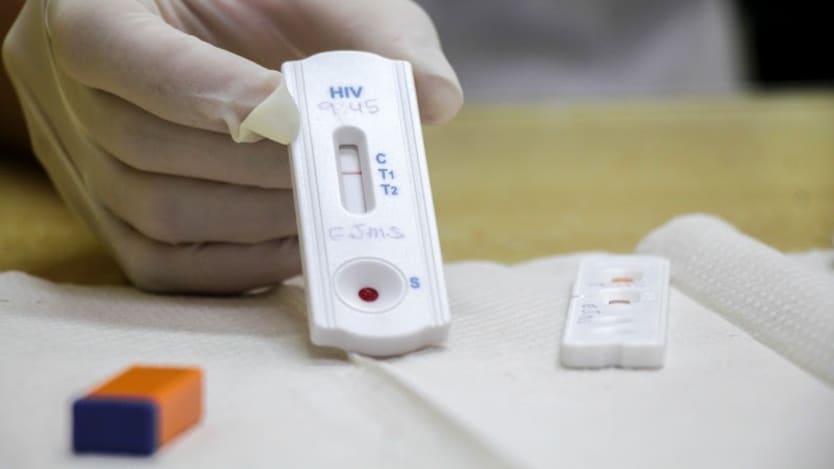
In the Philippines, there’s been a more than 70% delay or reduction in the number of visits to HIV clinics since the arrival of COVID-19, according to a survey conducted by Gilead Sciences and partners. Restrictions on mobility as a result of the pandemic were blamed. As a result, 64% of individuals at-risk reported a decrease in testing and more than half reported having either decreased or stopped taking their preventive medications.
“Proper routine testing, as well as preventive care, are important for affected populations to manage their health to avoid higher risk of health complications,” explained Dr. Katerina Leyritana, medical director of Sustained Health Initiatives of the Philippines, a local partner in the survey. Limited clinic visits could mean significant setbacks in care in a country that already has the highest new HIV infection rate in the western Pacific region, she added.
In the survey — which looked at the extent of disruptions for HIV care across 10 countries in the Asia-Pacific region — 80% of Filipino respondents also cited concern about the long-term ability to access anti-HIV medications.
“It is crucial to find new ways to provide support and access to adequate HIV care when they experience such constraints,” Leyritana said.
Speaking to Devex, Leyritana explained what longer-term impacts there might be as a result of halted or delayed essential HIV care and diagnosis and how telehealth might plug the gap.
This conversation has been edited for length and clarity.
SHIP recently supported Gilead Sciences in conducting a survey evaluating the impact of the COVID-19 pandemic on the access and delivery of care in HIV in the Asia-Pacific region. What were the main findings?
Despite the small number of survey respondents, it gave us some insights on how COVID affected HIV, specifically in the Philippines and the Asia-Pacific region. Specific to our country, in the Philippines, we saw decreased access to HIV care with regards to personal visits of patients, and people wanting preventive medications, to physicians. There's also decreased access to laboratory tests because these are done personally at the clinic. We are in an extended quarantine in the Philippines and we saw that there was a more than 70% decrease in the number of visits. The findings also made us aware that the respondents are concerned about continued access to medications.
What is your reaction to these findings?
Impact of COVID-19 on access and delivery of HIV care in Asia Pacific
This survey was conducted online — by Kantar Health, funded by Gilead Sciences — throughout October and November 2020 in Hong Kong, India, Japan, Malaysia, Philippines, Singapore, South Korea, Taiwan, Thailand, and Vietnam. A total of 1,265 respondents, including people living with HIV, individuals at-risk, and HIV care prescribers, were interviewed. 153 were from the Philippines.
The purpose of the survey was to assess the current status as well as gaps and barriers to access to HIV care during COVID-19. The findings provide insights on the impact of COVID-19 to the disruptions of HIV care and inform ways in which health systems, as well as the HIV community, can adapt strategies to maintain the provision of HIV care services and mitigate future disruptions.
With regard to the growing concern about antiretroviral therapy supply, it was really surprising that the Philippines ranked No. 1, but then again, we have had some experience with inconsistent supply in our country so I guess it is somehow to be expected as well.
But I was happy to see that that telehealth was a favorable factor in the survey. Despite us having a limited number of personal patient visits, we saw that access to telehealth was actually appreciated by the respondents. During the survey, we were already making use of the remote refill process in 150 clinics providing HIV in the Philippines so this was to be expected because telehealth was being used by some providers in some areas at least.
What do these findings mean to the Philippines and Asia countries in general?
I think it means that we have to increase investments in innovation [and] in HIV service delivery, which will actually help achieve the objectives of the differentiated service delivery. COVID has forced us to think outside the box and despite it presenting as a problem, it actually provides us an opportunity to make things better.
What longer-term impacts could halt or delayed essential care and diagnosis have on people living with HIV?
What's important is that the supply-chain of medications should be protected. The lockdown of countries engaged in ART production can actually grind things to a staggering halt. HIV testing at the community level can also be severely affected and it was a great means of reach in the Philippines. During our initial strict lockdowns, this was severely affected by about 50% and this could happen again with every major COVID-19 surge. With this in mind, I think we need to have HIV self-testing done, whether it's assisted or not assisted, but provide a means of support and counseling and linkage to care, even by virtual means.
How do you think the current gaps and barriers to care should be addressed and what actions can be taken to sustain critical health care services for HIV at this time?
Telehealth is great, but internet-based video conferencing is not available for everyone. Our internet connection in the Philippines is one of the slowest and we have geographically isolated and disadvantaged areas that do not support strong signals. Investment in this technology is important. However, in places where land or sea travel is not consistent maybe we can think of other things like drones or similar machines as a means of delivery of medication.
SHIP has been doing telemedicine and remote delivery for patients and telehealth for education years before COVID came into the picture so little adjustment needed to be done. We are looking for the next new thing to take on to make HIV service delivery adapt to the changing times. We are currently doing community-based PrEP at our main clinic and we are going to do same-day ART, index testing, and ART clubs [community ART distribution] when we open our new clinics this year.
What call to action do you have for the global health community around ensuring HIV care during a pandemic?
We were able to overcome the pandemic of HIV. Now let's use the lessons learned [over] all these years to conquer COVID as well. Our mission to care for people living with HIV does not end with closed borders and limited movement … We must strive to carry out our call to end unnecessary deaths from HIV through prevention, treatment, care, and support despite limitations. This is a call to action to think outside the box.








