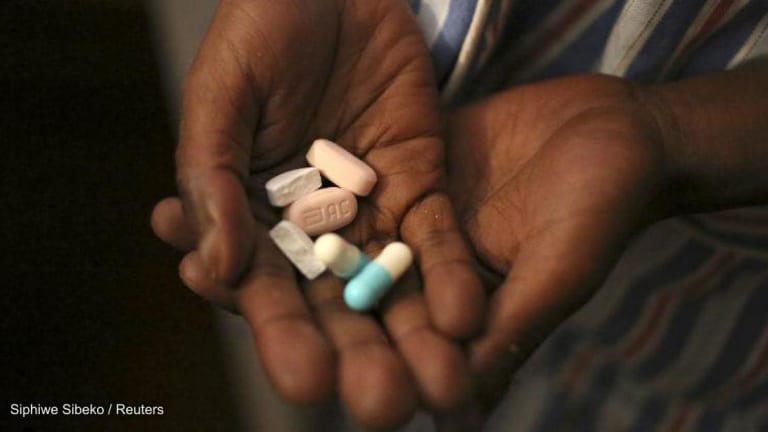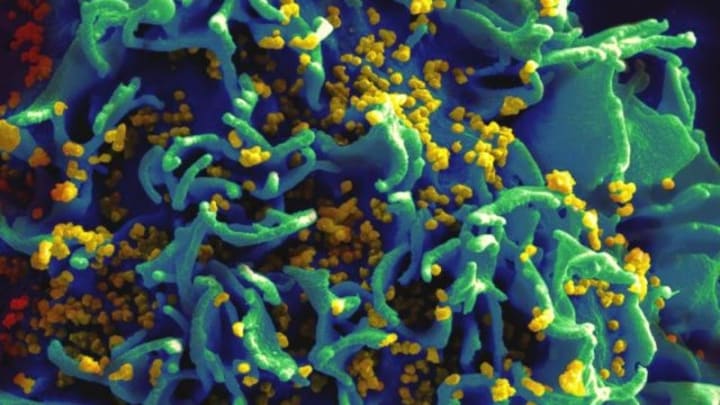
HIV/AIDS may have fallen off the priority list for many countries and international bodies with the arrival of COVID-19, but advocacy for adequately funded responses must continue, according to Dr. Adeeba Kamarulzaman, president of the International AIDS Society.
“There's no such thing as ‘HIV is more important than COVID’ or even ‘one disease is more important than the other,’” the Malaysia-based doctor said. “However, as we've learned over the past four decades, if we don't adequately fund prevention programs and we don't adequately fund treatment programs, then the outcome could be worse — and, in the long run, could even be more costly.”
As the deadline for the Joint United Nations Programme on HIV/AIDS’ “90-90-90” goals approaches — 90% of people living with HIV knowing their HIV status, 90% of those diagnosed receiving sustained antiretroviral therapy, and 90% on ART having viral suppression by 2020 — many countries in Asia are already lagging behind. As of 2019, 25% of people living with HIV in Asia and the Pacific did not know their status, while 20% of those diagnosed were still not on treatment.
Kamarulzaman said the region needs to do better but admitted that it will be difficult without sustained funding for programs and with COVID-19 disrupting treatment.
“We have so many tools — particularly prevention tools, but also treatment tools. And we need to keep pushing governments and relevant international bodies to ensure that these tools get to the people who most need them,” Kamarulzaman said.
Speaking to Devex, she provided insight into what an HIV testing and preventive strategy looks like in Asia, the need for a holistic approach, and what it will take to end the epidemic in the region.
This conversation has been edited for length and clarity.
What are the challenges in Asia in regard to tackling HIV/AIDS?
One of the issues with HIV/AIDS in the Asia and the Pacific is that it's not a homogeneous region. It's very diverse in terms of key populations. A large proportion of infections in Asia-Pacific are among the key populations at risk in certain countries. It could be people who use drugs; in other countries, it could be [men who have sex with men, or MSM] and transgender [people]. And so that adds to another layer of complexity in terms of prevention efforts.
One of the things we do know in Asia and the Pacific is that many who present for treatment do so at a later stage of illness, with CD4 [cell] counts averaging in the low 200 to 300. And that indicates that either they're not being tested early or they're presenting late because of fear of stigma and discrimination.
What will it take to end AIDS in Asia?
Health literacy in this part of the world in general is a lot lower, and health literacy specifically around HIV [and] around advanced treatment needs a lot more work, so that's No. 1. And No. 2, because those at risk already are discriminated against, that adds a layer of complexity — that intersectional stigma of living with HIV and the stigma of either being an MSM, transgender, a sex worker, or a person who uses drugs.
So what can be done to address those two? No. 1 is more peer-led education.
No. 2 is engaging the community and peers in delivering services. There are wonderful examples from Thailand [and] Vietnam, where peer-led HIV testing efforts have increased engagement in care. Peer-led preexposure prophylaxis delivery services have also been shown in Thailand to increase PrEP uptake and linkages for MSM, for transgender [people]. So I think community engagement and community participation and community services are crucial.
No. 3 is utilizing technology, and I think the COVID-19 pandemic has forced us to fast-forward the use of technology, whether it's HIV testing or whether it's engaging people in PrEP and giving the education to a much wider audience through social media. To me, that's one of the key answers in countries like mine, which are extremely conservative.
We've been talking for years about having sexual education and HIV education in schools, and we just get stonewalled. With Malaysia and in fact the whole world becoming more and more conservative, I don't see that changing overnight. I think we just need to get more creative, and digital technology is the answer to that.
No. 4 — and probably what's going to be one of the most impactful but also one of the most difficult — is, of course, policy and legislative changes. … Many countries in my region still have laws and policies that not only criminalize sexual behavior, but also sex work and drug use. All of these drive people underground and therefore limit their access to information, to prevention, treatment, and care, and [they] feed ongoing stigma and discrimination.
What do you think a holistic HIV prevention strategy looks like?
In the past few years, we've heard about so [many] advances with HIV treatment and that people on effective treatment can live a healthy, normal, productive life, with a good quality of life and a normal life expectancy. There is also the availability of preventive treatments for individuals at risk.
While we have all these wonderful technologies and advances in treatment and prevention, if people are not coming forward to receive them or people are not coming forward for fear of being arrested, for fear of being turned away by a hostile health care system, then those things are not going to be effective.
Do you think enough is being done to reach all people with HIV testing and prevention strategies?
I think different countries have achieved the targets differently, and I have to say it's never enough. There's always going to be a new generation that needs to be educated in HIV/AIDS. Unless it's completely eliminated, that risk is always going to be there, and therefore there has to be ongoing education and ongoing access to prevention services, treatment services, and testing services.
Are there lessons that can be learned from certain countries on this?
HIV self-testing — I think Thailand has scaled this up — where people can order the HIV test kits online, is one important example because we really need to increase the percentage of that first “90” all over the region. And I can't say enough about the importance of community engagement.
However, I think it also comes hand in hand with adequately funding these community organizations to deliver essential health services. Often, these communities and peer group organizations are not adequately funded and live from month to month, year to year, in terms of the funding and cannot effectively scale up or effectively provide the kinds of care that they potentially could.
Is there any one entity you think should be playing a bigger role in expanding HIV testing to the marginalized and key affected populations?
I think one of the hallmarks of the HIV response since the 1980s is the collaborative nature that makes it successful. Government agencies can't do it alone, but neither can community organizations and civil society. We all play our part, and it has to be collaborative and adequately funded and with adequate training.