EDITOR’S NOTE: The global health agenda is only starting to pay attention to neglected tropical diseases. Overseas Development Institute researcher Romina Rodriguez Pose tells the story of a group of community volunteers leading the fight against NTDs by distributing the drugs themselves in Sierra Leone.
For the world’s poorest, difficult living conditions are often compounded by the prevalence of a threat to their health that for many years barely appeared on the global health agenda — a group of ailments known as neglected tropical diseases (NTDs). Ninety percent of the NTD burden can be explained by five diseases: Onchocerciasis, also known as river blindness (causing terrible itching and lesions on the eye), Schistosomiasis or bilharzia (causing extensive organ damage), Lymphatic Filariasis, also known as elephantiasis (causing damage to the lymphatic system and painful enlargement of body parts), Soil Transmitted Helminths (causing diarrhoea, abdominal pain, chronic intestinal blood loss and anaemia) and Trachoma (the world’s leading cause of preventable blindness).
I first came across NTDs while conducting research for the health dimension of the Development Progress project. I’ve been working on development — and particularly on health — for some time now, so it was quite a surprise to me that I had never heard of them before (I remember thinking: “well, indeed they are neglected!”). As part of the project, I had the opportunity to travel to Sierra Leone to conduct field research and see first-hand how NTDs are being addressed.
Sierra Leone was chosen because of the progress it has made in recent years in tackling NTDs. For instance, in 2005, elephantiasis was found endemic in all 14 health districts in Sierra Leone; by 2011, only one district remained endemic. In the case of river blindness, therapeutic coverage has consistently been over 70 percent since 2006, with the programme’s geographical coverage consistently reaching 100 percent since 2007, translating into an overall reduction in prevalence of 60.3 percent between 2007 and 2009.
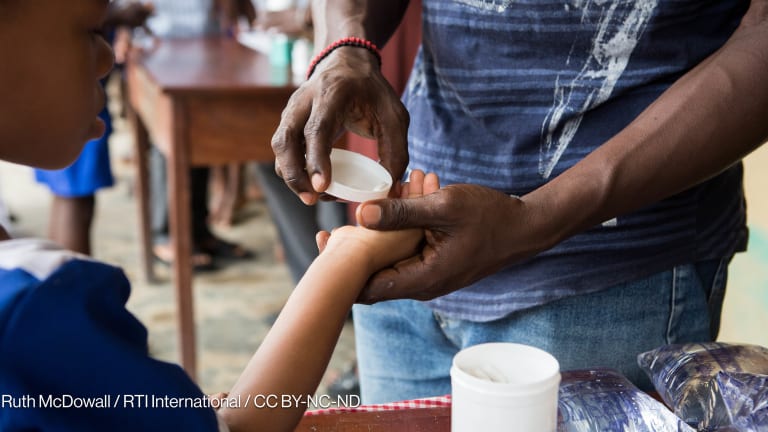
By far the most striking aspect of the field research was meeting those on the frontline of the fight against NTDs. Known as Community Drug Distributors (CDDs), they are the most humble people you could meet, with scarce resources and no monetary incentives to do their job. Selected by their own communities, once a year they have the responsibility of distributing drugs to fight NTDs, with each CDD covering their catchment area over a period of three months.
Why has this experience of meeting the CDDs had such an impact on me? After all, community involvement is a well-known strategy to implement programmes in a resource-constrained setting. Well, in the case of NTDs, we are talking about a vastly different scale to normal — the strategy implemented through the CDDs is known as ”mass drug administration“(MDA). For an MDA campaign to be successful it must reach every corner of the country where NTDs are endemic (in Sierra Leone, this is the entire country) and at least 70 percent to 80 percent of the people living in those areas. This is because most of these diseases, whilst transmitted by vectors, only develop in a human host. It is therefore necessary to reduce their prevalence in the community to a sufficient level that allows for the gradual interruption of disease transmission. Without meeting this target, all efforts will be in vain.
While on the ground in Sierra Leone, travelling through the countryside by 4x4 under a burning hot sun, I couldn’t help but feel admiration for the CDDs, who undertake similar and often even more remote journeys but on foot. During focus group discussions, they told us how they sometimes walk for four hours to reach the farthest and most remote settlements; once there, they still need to convince community members to take these vital drugs. Sometimes they must cross rivers, or walk in the rain (and I mean serious rain!) to cover their assigned catchment area, and all without what we in wealthier countries might consider the necessary outdoor wear.
Perhaps not surprisingly, when you talk with the CDDs, you hear a lot of complaints — that the job is very hard, that they need incentives and support beyond just their free CDD t-shirts and that they are sometimes not received kindly by those they are there to treat, particularly in the early days of a campaign. As I listened to all their troubles, I kept coming back to the question: “Why are you still doing this?”
The reason is a sense of community — the manner in which the NTD control programme is implemented empowers CDDs with an important role to play within their communities, despite the lack of financial reward. The CDDs are clear and straight forward when answering this point: they are doing this to help their communities, because they themselves have seen how the distribution of medicines has reduced the harm caused by NTDs amongst their peers. One told us: “I was sick with worms in the past and then I took the drugs and they relieved me, so I want to pass on the message and contribute.”
Their commitment is paying off. A key development actor told us how in the past he would go to certain towns and the majority of the people had lost their sight due to river blindness. Returning to those places after years had passed and after the work of the CDDs had begun, he could see the change in plain sight: far fewer people were blind.
Throughout our fieldwork, people gave testimony to the work of the CDDs, such as one woman who said: “I was reluctant to take the medicine. We were suspicious but the CDDs explained to us why it was important. After taking the medicine, my itching stopped and I could see much better.” Thanks to their early efforts in reaching out to their peers, initial reluctance to take the drugs has faded and nowadays people start asking for the drugs even before the distribution campaigns start.
CDDs are one, but a seemingly essential, part of this story of progress. The fight against NTDs is a collective effort, comprising many actors, from the World Health Organisation setting international guidelines and the support of a range of international partners, to Ministries of Health developing these guidelines into strategies for local implementation, non-state actors such as NGOs providing technical assistance and pharmaceutical companies donating the drugs themselves to fight the diseases on the ground. However, all these efforts would be doomed to fail without those at the sharp end of the fight, walking throughout their communities to distribute the drugs and convince their peers of the positive impact they can have in their lives.
Edited for style and republished with permission from the Overseas Development Institute. Read the original article.