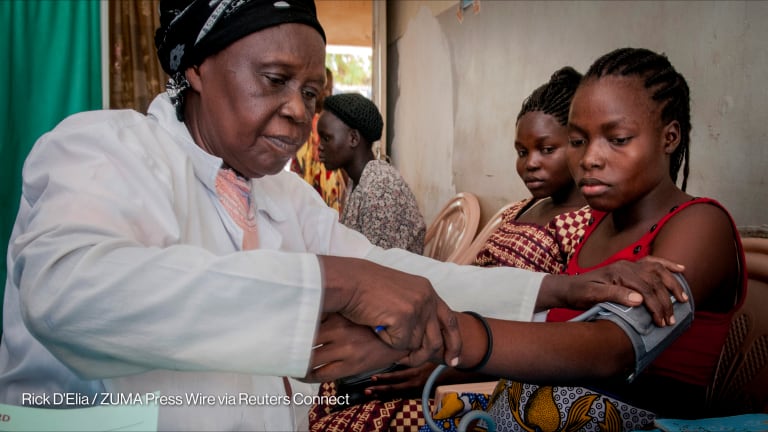Strong health systems: The offense to defend against future epidemics?

After recently doing very important and admirable work in Guinea, Dr. Craig Spencer returned to New York City and within days showed symptoms of Ebola. Yet Spencer had access to an equipped local health facility, and access to transportation to safely take him there. At the hospital, he had access to trained health care providers with personal protective equipment and access to quality supportive care. He was fortunate to access care in a well-developed health system.
Thousands in West Africa have unfortunately not been so lucky. The Ebola epidemic is a constant reminder that the capacity to prevent, detect, and rapidly respond to infectious disease threats is essential. It was because of the weakness of the health systems in West Africa that Spencer put himself in harm's way to help fill a gap in trained health care workers.
Strong health systems are not only crucial to bring the current epidemic under control, their economic and social impact are a critical step to ending extreme poverty and building resilient societies.
The Global Investment Framework, an argument for increased global investments in women and children’s health, shows that an investment of less than 0.2 percent of a country’s gross domestic product on health systems and infrastructure would show a return on investment by 2017 that would only continue to grow each year.
The upfront cost is to build out health systems and expand access to care. For example, a woman in need of emergency obstetric care needs a healthy facility nearby, means to travel there, access to a skilled birth attendant, and the ability to afford all of this. Once these structures are in place, governments can spend the majority of their resources on operating expenses like commodities, ongoing workforce training, and prevention of illness.
More than 20 years after investing in these health systems, they are still reaping benefits. A child that was saved because he had access to a health worker to diagnose and treat his pneumonia is now 25 and in the workforce. The social and economic combined benefits of lives saved, morbidity averted, and an enhanced workforce can have an impressive return on investment. According to the Investment Framework, for every U.S. dollar invested in health, the return is between $9 and $20.
Let’s not let economics mask the positive impact strong health systems bring to families and societies. Investments in health are widely recognized as building individual ability to learn and work. Children whose mothers pass away are on average less likely to make it to age two than their peers, and even if they do they are disadvantaged socially and economically for the rest of their lives. Healthy individuals can care for their children: they make it to work and are able to contribute to their families’ income and therefore that of their society. Strong health systems lay the groundwork for countries to have healthy citizens, who in turn help their countries rise out of poverty.
The fact that Spencer showed symptoms of Ebola in one of the world’s most populous cities is not what is most important in the current crisis. Instead, it should teach us the incredible value of strong health systems. The same structures that keep populations healthy during stable periods — like trained health care workers, health facilities, and surveillance systems — are the ones that allow countries to adeptly manage and respond in a time of crisis.
When a health system is not robust or strong enough to handle a crisis like Ebola, we risk an epidemic at vast scale. According to the Institutes of Medicine, only 20 percent of the world’s nations are currently prepared and able to effectively respond to a pandemic. Defeating this Ebola epidemic is going to take a huge coordinated effort among governments, health care workers, civil society, and others to gain control and get the health systems in place to deal with its impact.
Looking ahead, shouldn’t we try to build strong health systems, so they are resilient and ready to respond to future threats to our global health?
Want to learn more? Check out the Healthy Means campaign site and tweet us using #HealthyMeans.
Healthy Means is an online conversation hosted by Devex in partnership with Concern Worldwide, Gavi, GlaxoSmithKline, International Federation of Pharmaceutical Manufacturers & Associations, International Federation of Red Cross and Red Crescent Societies, Johnson & Johnson and the United Nations Population Fund to showcase new ideas and ways we can work together to expand health care and live better lives.
Read more #HealthyMeans articles:
● Ebola: Why we must play the long game
● Healthy means hospitals, too
● The next frontier of inclusion for the 'working poor' — and how insurers can profit
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5