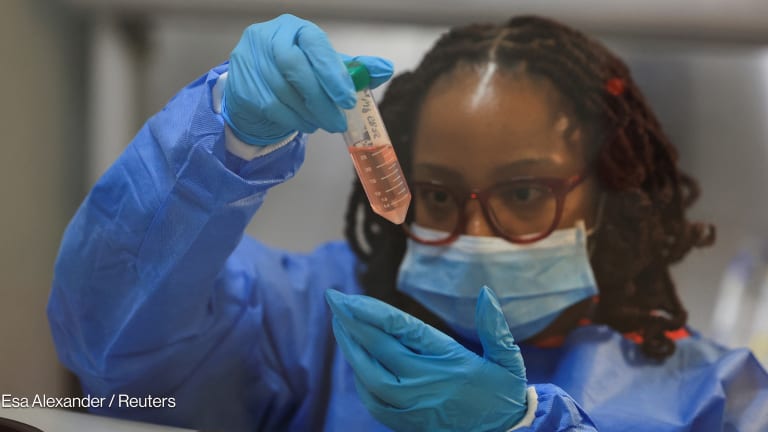
In March, Mercy Corps warned that countries that had the highest levels of violent conflict will most likely be the last to achieve widespread COVID-19 vaccination.
In a statement, the organization’s CEO, Tjada D’Oyen McKenna, said that “by the time vaccination efforts reach communities in fragile contexts, unequal distribution may itself deepen or sow new divisions.”
Sign up for Devex CheckUp
The must-read weekly newsletter for exclusive global health news and insider insights.
“Vaccine refusal may be high and compliance with public health guidelines may be low, further prolonging the spread of the virus and fueling protracted waves of conflict and economic disruption,” she said.
As vaccine rollouts begin in Africa, health experts in countries experiencing conflict fear that people living in such conflict zones are at a double disadvantage due to the conflict and limited continental access to vaccines.
Though some countries have mechanisms in place to roll out vaccines in their conflict zones, health experts have warned that the continent needs to secure enough doses before these rollouts can begin.
Vaccines outlawed
More than half of the 20 countries that experienced the highest levels of conflict in 2020 were African countries and according to Mercy Corps, these countries will most likely reach widespread vaccination in 2023 or later.
Ahmed Khalif, Somalia country director at Action Against Hunger, said in Somalia people living in regions controlled by Al-Shabaab will most likely not get access to vaccines as they have to choose between taking a chance with vaccine-preventable diseases or risk getting killed by the Al-Shabaab militant groups — who have outlawed vaccines.
“Al-Shabaab groups have given a pronouncement that they will not take the COVID-19 vaccine and that has been their position even before COVID-19, with routine immunization like measles, polio, [and] that has not changed,” he said.
“In our planning for these security-compromised areas, we engaged the military just like we did with the polio [vaccination program].”
— Dr. Faisal Shuaib, executive director, National Primary Health Care Development AgencyIn areas under the control of the government, vaccine hesitancy and resistance are being driven by misinformation which officials are striving to address. But in parts of the country that are controlled by the Al-Shabaab militant group, there is little or no hope that the COVID-19 vaccines will reach people there, considering the group has outrightly banned vaccination exercises, he said.
Action Against Hunger has been helping the Somalian health ministry with the COVID-19 vaccine rollout, with the militant group’s position on vaccination clear, the organization has limited their interventions and COVID-19 vaccine support to parts of the country where they have full or partial access.
“It [rolling out vaccines] presents more security challenges than it will help them prevent the disease. Lives are affected at both levels — whether you get killed by them [Al-Shabaab] or by the disease,” Khalif said.
While Al-Shabaab has lost control over the port cities of Kismayo and Barawe, it controls the southern city of Jilib, which was made as its de facto capital, in addition to controlling parts of central and southern Somalia. It also has a resurgent presence in the north, where it is battling fighters affiliated with the self-proclaimed Islamic State.
Using the military to deliver vaccines
Nigeria also has a militant crisis in its northern region that delayed and almost derailed its national polio control program but has laid the foundation for the country’s COVID-19 vaccination plans for its crisis zones.
Tracing Nigeria’s long fight against wild poliovirus, Oyewale Tomori, a Nigerian professor of virology and chairman of Nigeria's Ministerial Expert Advisory committee on COVID-19, told Devex that crisis in the northern region was a major contributor to the country being the last African country to eradicate the disease, due to lack of access to targeted vaccine recipients in conflict areas and widespread distrust exacerbated by the crisis.
While admitting conflicts contributed to the delay in ending polio, the country’s agency in charge of Nigeria’s COVID-19 vaccination efforts — the National Primary Health Care Development Agency — told Devex the systems it put in place to overcome the challenges posed by conflict zones to polio vaccination efforts are still in place; ready to be deployed to expand COVID-19 vaccine access to dwellers of crisis zones in Nigeria.
NPHCDA Executive Director Dr. Faisal Shuaib said that valuable lessons were learned and are being carried forward.
“We learned our lessons from the polio eradication program, and in our planning for these security-compromised areas, we engaged the military just like we did with the polio,” he said. “In those areas where, due to insecurity, civilian health workers could not go, we actually had military officers drop oral polio vaccines in the mouths of children.”
Securing more doses
Humanitarians plan for COVID-19 vaccinations in conflict zones
International and regional NGOs operating in conflict zones are beginning to prepare for the first batches of COVID-19 vaccines expected this year. Access is a chief concern but far from the only one, experts say.
Dr. Matshidiso Moeti, World Health Organization regional director for Africa, said the global health body and the United Nations are urging countries with ongoing conflicts, displaced persons, or humanitarian crises to commit some proportion of the vaccines that they’ve acquired for people in difficult areas.
But Dr. John Nkengasong, director of the Africa Centres for Disease Control and Prevention, said before the continent starts making plans to vaccinate in such areas, vaccine doses need to be secured.
“Most vaccinations are happening in major cities which makes sense — that’s where the pandemic, which is the enemy, is,” he said. Adding that vaccinating large chunks of the population in major cities “will create herd immunity very early on.”
“That will give us time to do a mop-up operation in those conflict areas, and just vaccinate them. You need to have vaccines before you start planning on vaccinating in conflict areas,” he said.