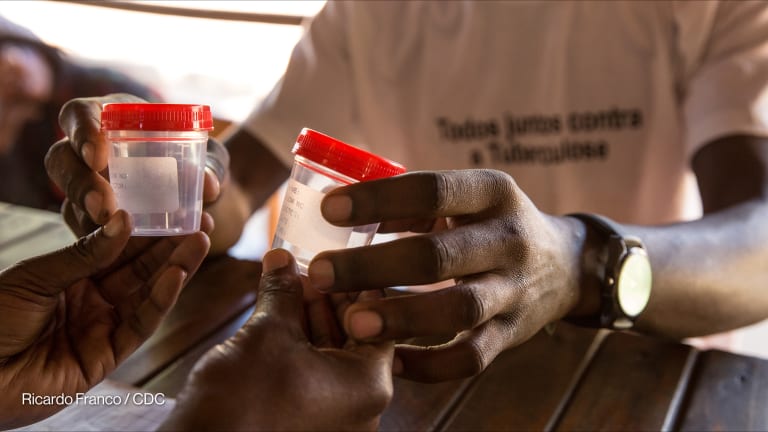
NEW YORK — The novel coronavirus outbreak is further derailing progress toward ending tuberculosis, experts say. At the same time, COVID-19 is providing an example of what is possible when an infectious disease is met with a high-profile, global response.
“I hope that the COVID lesson is that ... investing in health is an important piece of the work.”
— Lucica Ditiu, executive director, Stop TB PartnershipThe U.N. Sustainable Development Goals aim to end TB, long considered the world’s most infectious disease, by 2030. Governments have also committed to treating 1.5 million people with multidrug-resistant TB — or MDR TB — by the end of 2022. But continued progress over the last several years has now been lost in the first two quarters of 2020, said Lucica Ditiu, executive director of the Stop TB Partnership, in a Devex digital event Monday.
More on TB:
► Will new TB treatments reach those who need them most?
► Opinion: The impact of the technology revolution on tuberculosis
“We are far behind in terms of treatment. The current environment is creating additional challenges for us,” Ditiu said. “As much as we are passionate and engaged in the fight to end TB, the reality is now that if someone would have told us almost no flights in the world would be happening for weeks … anyone would have said that this is fantasia, it could never happen,” Ditiu said.
In 2018, an estimated 10 million people became sick with TB — with a relatively stable rate for the last several years — and 1.5 million people died because of the disease, according to the World Health Organization. The rise of MDR TB has posed another threat in the battle against the infectious disease. Globally, 3.4% of new TB cases and 18% of previously treated cases had MDR TB in 2018.
On Tuesday — World Tuberculosis Day — WHO released new guidelines to help countries accelerate efforts to provide preventive treatment to people infected with TB.
“COVID-19 is highlighting just how vulnerable people with lung diseases and weakened immune systems can be,“ said Tedros Adhanom Ghebreyesus, WHO director-general, in a media release. “The world committed to end TB by 2030; improving prevention is key to making this happen. Millions of people need to be able to take TB preventive treatment to stop the onset of disease, avert suffering and save lives.”
About one-quarter of people across the world are infected with the TB bacteria but are neither sick nor contagious. They are, however, at greater risk of developing the disease. Preventive treatment could help them stay healthy and also cut down on the risk of greater community transmission.
The new guidelines recommend increasing TB preventive treatment among at-risk populations, such as people living in crowded settings or with HIV, and integrating preventive treatment services during screenings of people who reside with TB patients.
The guidelines also recommend new, shorter options for preventive treatment, which could include a monthlong regimen of commonly used TB drugs such as rifapentine and isoniazid. Three- and four-month preventive treatment plans are also available, in addition to the widely used six-month regimen of daily isoniazid doses.
People living with TB are especially vulnerable to the new coronavirus, which had infected at least 380,000 people at publication time. The first reported deaths in South America are of people who had both TB and COVID-19, Ditiu said.
TB symptoms can be very similar to those for COVID-19 — a dry cough, fever, fatigue, and trouble breathing are all common — which can lead to people with TB not receiving testing for COVID-19, according to Ditiu.
COVID-19 — a timeline of the coronavirus outbreak
Follow the latest developments on the new coronavirus that causes COVID-19.
“I think we should be able to look at it and realize this has a major impact on what the prognostic of people with TB and MDR TB will be,” Ditiu said. “I am also worried, based on what we hear, that basically it is very difficult for people to reach the services that are right for getting diagnosed.”
Susan Maloney, chief of the global TB branch at the U.S. Centers for Disease Control and Prevention, noted that “innovative and people-centered approaches” to the two diseases could emerge from shared platforms between people working on both illnesses.
“TB has built a lot of capacity in countries that can be used to support the COVID response and to continue the response to TB,” Maloney said, speaking during the Monday morning digital event.
A clear difference between the diseases, though, is the pace and intensity of the global response. While there are nearly 30 vaccine candidates for COVID-19 and almost 100 types of diagnostic tests, there are just two tests for TB. The most common TB vaccine is roughly 100 years old and is not always effective.
“Money is not the issue. … It is a very good pipeline for diagnostics. We are getting some traction, but nothing close to this. I hope that the COVID lesson is that the decision-makers and people with money will finally understand investing in health is an important piece of the work,” Ditiu said.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5