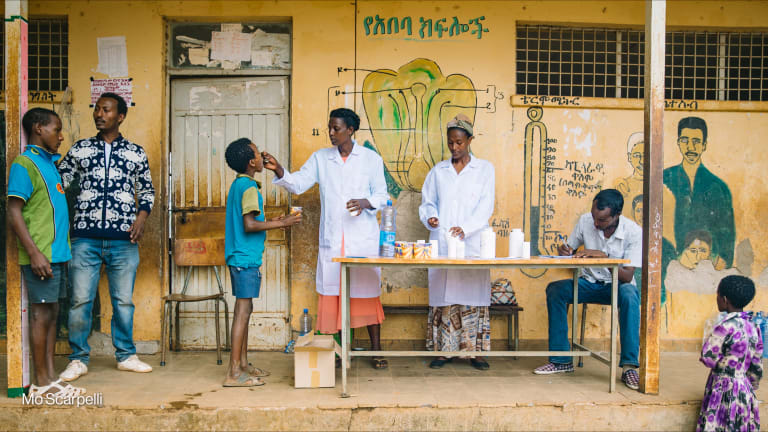
Working in partnership with a group of philanthropists and the U.K. Department for International Development has “allowed for a new way of doing business” in the fight to eliminate neglected tropical diseases, according to USAID’s head of NTDs.
The term NTDs refers to a group of illnesses that affect the poorest communities in the world, killing approximately 150,000 people every year, and disabling 1.6 billion. But given the relatively low death toll compared to other global killer diseases, they tend to be overlooked by donors.
The real impact of these diseases are felt long term through stunting, malnutrition, disability, and pain and suffering, which can perpetuate cycles of poverty as children miss school and adults are unable to work.
Printing articles to share with others is a breach of our terms and conditions and copyright policy. Please use the sharing options on the left side of the article. Devex Pro members may share up to 10 articles per month using the Pro share tool ( ).
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5