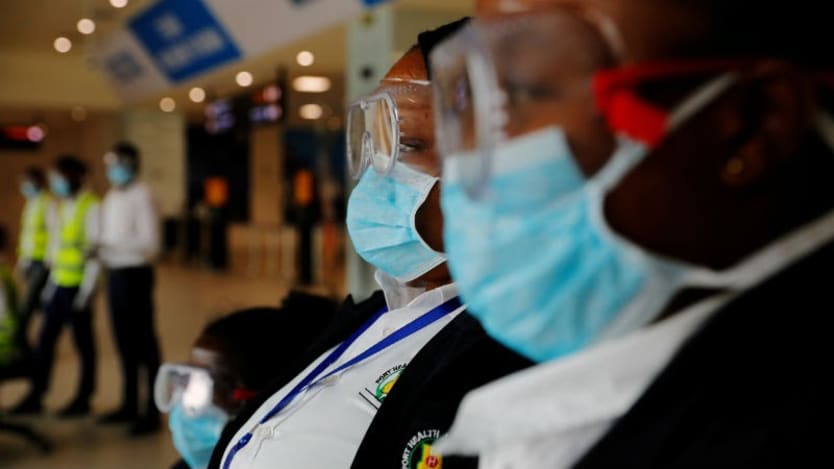
NAIROBI — As the outbreak of the novel coronavirus taxes the health system in China, there is growing anxiety about the potential dire consequences of the virus on countries with weaker health systems. The fears are particularly heightened across the African continent, where NGOs are expecting to play a key role in trying to contain the spread.
“I have a great concern that if this virus makes it to a weaker health system, it will create havoc,” said Dr. Tedros Adhanom Ghebreyesus, director-general of the World Health Organization, during a press conference Tuesday.
“If coronavirus hits a country where people are more mobile — like Kenya, Rwanda, Uganda — it will be very challenging to contain. It will be more of a disaster than Ebola.”
— Margaret Asewe, interim WASH adviser for Horn, East, and Central Africa, Oxfam InternationalThere are currently no confirmed cases of the new coronavirus — officially named COVID-19 — in Africa.
With the help of WHO, at-risk African countries have scrambled to enhance airport screenings for passengers with symptoms and increase capacity to test for the virus — originally only two laboratories on the continent had that capability.
If there is an outbreak in Africa, NGOs expect to help in areas such as patient care, support to governments, community sensitization, hygiene promotion, and contact tracing.
More on Africa and coronavirus
► African countries brace for coronavirus spread
NGOs can apply lessons learned from the response to the Ebola outbreak in the Democratic Republic of the Congo — which has been costly and lengthy — if there is a widespread COVID-19 outbreak, organizations told Devex. This includes the importance of early community engagement.
“It’s taken us so long to contain Ebola in DRC, and that’s just one country. If coronavirus hits a country where people are more mobile — like Kenya, Rwanda, Uganda — it will be very challenging to contain. It will be more of a disaster than Ebola,” said Margaret Asewe, interim water, sanitation and hygiene advisor for Horn, East and Central Africa for Oxfam International.
Because it is a respiratory virus, COVID-19 is more contagious than Ebola, according to health experts.
Overwhelming health systems
Currently, the vast majority of cases of COVID-19 — 44,700 of the 45,100 total at the time of writing — are in China, which has a sophisticated health system capable of delivering high levels of intensive care, said Dr. Michael Ryan, executive director of WHO Health Emergencies Programme, during a press conference on Monday.
In the current outbreak about 90% to 100% of patients need supplemental oxygen, up to one quarter those patients need intensive care, and about 5% to 10% of patients may require some form of mechanical ventilation, he said — a huge demand on a system.
“This disease may appear relatively mild in the context of a sophisticated health system. That may not be the case should this disease reach a system that is not as capable as that of China,” he said.
WHO has categorized African nations into priority groups based on transport connections between those countries and China. Top priority on the continent includes Algeria, Angola, Côte d'Ivoire, DRC, Ethiopia, Ghana, Kenya, Mauritius, Nigeria, South Africa, Tanzania, Uganda, and Zambia.
“That’s what we are really concerned about because most countries have malnourished populations of people who are already suffering from diseases that may make their immune system compromised. If it were to come to those places, and the government couldn't respond very well then communities would be particularly vulnerable,” said Erica Van Deren, senior program manager, humanitarian and emergency affairs at World Vision.
A major concern is if coronavirus were to spread in dense, urban areas.
“The big slums in Nairobi, for example, worry me to the maximum because I don’t know how you could contain it in a situation like that,” Asewe said.
“This disease may appear relatively mild in the context of a sophisticated health system. That may not be the case should this disease reach a system that is not as capable as that of China.”
— Dr. Michael Ryan, executive director, WHO Health Emergencies ProgrammeNGOs gearing up, community engagement
There is a need across the continent to increase and improve isolation facilities, equipping these facilities with things such as personal protective gear and hygiene products, and prepare for community engagement, NGO representatives said.
WHO is hosting meetings with governments and NGOs to provide updates on the situation and outline preparedness measures. NGOs across the continent are passing along information to their field teams to prepare for a potential outbreak. They are also meeting with national ministries of health.
World Vision, for example, has convened a global executive oversight group for COVID-19 and its recommending all of its offices in Africa and Asia take preparedness measures such as assessing internal capacities to respond and looking into how it might procure masks, if needed. In Kenya, Médecins Sans Frontières is part of a national task force to organize preparedness. The Alliance for International Medical Action is working with national governments to identify resource gaps in areas such as patient care, logistics and human resourcing.
Some of the structures already in place for the Ebola response could be scaled up for a COVID-19 outbreak, Asewe said. For example, NGOs in the DRC Ebola response created coalitions to improve information sharing and coordinate their work at a regional and country-level, she said.
One of the major flaws of the Ebola crisis, responders agree, was that communities were not engaged early enough — which led to the spread of misinformation, resistance to treatment, and the violence against health workers.
If there were a COVID-19 outbreak in Africa, it would be crucial to have early engagement with communities to explain how they can avoid the virus and what needs to happen when someone in the community contracts the virus, according to NGOs. It also includes setting up systems for feedback from communities.
“I think as doctors, sometimes you see this medical issue and you just jump in and want to treat it and forget that you need to explain to a patient what the problem is and why you're going to do what you're doing,” said Dr. Trina Helderman, senior health and nutrition adviser at Medair.

With Ebola, organizations learned to engage with a variety of trusted figures including community leaders, community health workers, motorcycle taxi groups, traditional healers, pharmacists, among others, Helderman said.
For example, in DRC, Catholic Relief Services trained local influential faith leaders on Ebola messaging.
“That was one of the main lessons for us — the messenger is as important as the message,” said Oliver Hughes, head of programming for Eastern DRC for CRS.
Community engagement can help combat false information. There have already been rumors of COVID-19 cases spreading across the continent and the spread of information fake remedies, such as boiling water and garlic.
Funding for preparedness, adapting programs
But funds for preparedness are not always easy to get, according to NGOs.
“What we have learned from Ebola preparedness is that getting resources just for preparedness is not very easy,” Asewe said. “People just want to react when there is a case.”
Fortunately, there are some similarities in preparing for a COVID-19 outbreak and other outbreaks, NGOs say. The hygiene messaging is similar to cholera and other communicable diseases. There are also programs that can be adjusted to include a potential COVID-19 outbreak.
For example, after the West Africa Ebola outbreak, CRS began programs in Senegal focused on community-based infectious disease surveillance that includes training community volunteers on the signs and symptoms of eight infectious diseases. These volunteers are given a cellphone and they alert nurses, who verify the case within 48 hours.
“The sooner you can identify these cases and have the nurse come to them versus them traveling a long distance and potentially contaminating other people, the better because you're containing the virus at its source,” said Nickie Sene, head of programming for Senegal and The Gambia for CRS. She said CRS has been in touch with WHO and the regional working group to see if this system could be used to respond to a potential COVID-19 outbreak.
Personal protective gear shortage, creating protocols
Part of preparedness measures for a potential outbreak for NGOs include ensuring access to personal protective gear — like masks and gowns — but there is a global shortage of personal protective equipment because of the COVID-19 outbreak.
“That has become a bit of an issue logistically in that several of the suppliers have either stocked out or are having issues with exporting items. That's something that we're working on currently,” Helderman said.
Medair is working to have a baseline of this equipment in stock, to help the organization if it were to handle any initial cases in African countries that it works in, but this supply would run out quickly if there were an outbreak, she said.
The global shortage could also impact other outbreaks.
Medair had a procurement for protective gowns for its Ebola response, but there was a delay. The supplier told the organization that the delay was because there were issues with the suppliers getting these items because of the COVID-19 outbreak.
WHO said there is a four to six month backlog in obtaining this equipment. Even when there isn’t a shortage, there can be delays in obtaining protective gear. Medair’s fastest supply chain in DRC is usually about two to three months, to get a large supply, Helderman said.
“With long delays, I think you will see a lot of sick health care workers. They wouldn't have any way of protecting themselves if they're still caring for patients. If you have a lot of sick healthcare workers, there could be a collapse of the health care system because you don't have anybody to work,” she said.
It’s also important for countries to start defining their protocols now — in terms of the systems in place to manage cases, Helderman said.
“With Ebola, it took us more than a year to define our protocols. Having countries start early, even before they have a case, it's really important to make sure that when there is a case, people are not caught completely off guard,” she said.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5








