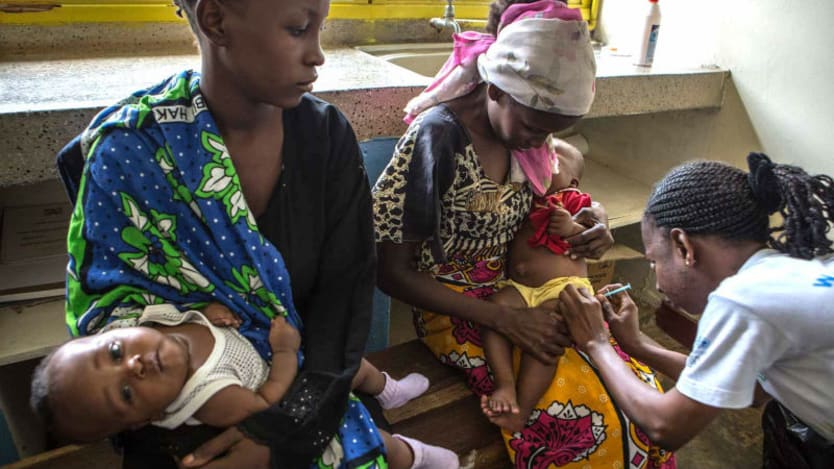
UNITED NATIONS — Pneumonia is the biggest killer of children worldwide, but when it comes to fighting the deadly disease, the problem is not a lack of tools or knowledge, but access, experts say.
A combination of factors — including the respiratory infection’s ambiguous symptoms and a low rate of vaccination — contributes to the relatively slow decline of pneumonia, sometimes thought of as a silent killer that does not garner enough media or development sector attention.
See more related topics:
► Opinion: 3 ways to end preventable child deaths from pneumonia
► Bill Gates makes the business case for breakthroughs in global health
“It’s not for lack of tools, but for putting it together and reaching the beneficiary,” Stefan Swartling Peterson, the United Nations Children’s Fund’s chief of health, told Devex in a recent interview at UNICEF headquarters. “The difference between what we know, and what actually reaches the people who need it.”
UNICEF, the Bill & Melinda Gates Foundation, and other research and technology organizations are now teaming up to jump-start global attention to lagging progress on the infection, which caused 16 percent of all deaths among children under five in 2016 alone.
“Unfortunately, this is surprising to most people that pneumonia is the number one killer of children in the world, and it is surprising because in developed countries pneumonia is way down the list of causes of death in young babies,” said Keith Klugman, the director of pneumonia at the Bill & Melinda Gates Foundation. “It used to be that the biggest risk to mortality for these kids was from poor quality of water.”
While at risk young children are still extremely vulnerable to malaria and diarrhea, the spread of mosquito nets and oral rehydration solutions have helped these related child deaths drop dramatically since 2000. Infant mortality linked to pneumonia fell 47 percent between 2000 and 2015, dropping from 1.7 million to 920,000 deaths.
“By virtue of the fact there has not been a global community and no funding stream routing for pneumonia means it has gotten lost in many ways.”
— Stefan Swartling Peterson, chief of health at UNICEFProgress on pneumonia in children — increasingly presenting in countries in conflict and middle-income countries — is still too slow, pneumonia experts such as Klugman and Peterson say. While the under-five mortality rate has more than halved worldwide since 1990, pneumonia could place the Sustainable Development Goals target of ending preventable deaths of children under five by 2030 out of clear view.
In late 2017, UNICEF hosted the Gates Foundation and other organizations at the agency’s headquarters in New York to discuss pioneering solutions to end child pneumonia deaths. It was a chance to convene different organizations working on parallel tracks, and also to present new innovations, such as a device that can capture and store oxygen without electricity.
“We’ve been through a period that has targeted various diseases through various initiatives, and unfortunately pneumonia has not been one of those. We have targeted HIV, tuberculosis and malaria predominantly through various vertical funding initiatives,” Peterson said.
Not so for pneumonia.
“By virtue of the fact there has not been a global community and no funding stream routing for pneumonia means it has gotten lost in many ways,” he continued.
Isolating the problem
Correctly diagnosing pneumonia can sometimes be the first challenge.
When kids fall sick with pneumonia, they don’t always present flashing symptoms of the respiratory infection. Pre-existing conditions such as malnutrition, influenza or other issues that compromise their immune systems can cause small sacs in their lungs to fill with pus and fluid. Breathing becomes rapid and painful.
These respiratory symptoms can often mask themselves as malaria, Quique Bassat, a pediatrician and research professor at the Barcelona Institute for Global Health, found in a 2011 study in Mozambique.
“The clinical symptoms are not easy to distinguish and overlap with different diseases,” said Bassat, explaining that many of the “supposed malaria” cases he treated in children were actually pneumonia.
In the case of Mozambique, where the under-five mortality rate is 79 deaths per 1,000 live births, only 50 percent of kids with suspected pneumonia will be taken to a health provider, according to U.N. figures.
If a child with suspected pneumonia is taken to a health provider, a precise diagnosis of pneumonia would require imaging of the lung and an X-ray. This technology is rare in most health clinics in Mozambique, like many other developing countries, Bassat says.
Awareness is another issue. A small study in Mozambique in 2011 found that caretakers often thought it was possible to treat respiratory distress in their children at home.
Peterson, though, suggests looking beyond families as a source of blame to placing the responsibility on the global health community.
“I would like not to blame caretaker and parents as ourselves in the health system, because we are actually failing to deploy very effective tools in terms of immunization and the appropriate diagnostics and the oxygen for those who need it,” he said. “We need not just product, we need system innovation, and social innovation.”
Presenting workable solutions
Oxygen — along with antibiotics — is key to pneumonia treatment. If every child with pneumonia who reached a health facility received oxygen support it could make a huge difference in reducing infant mortality.
This doesn’t always happen, though, explains Jim Black, an infectious disease specialist. He’s the co-designer of a new device, FREO2. The system produces oxygen without electricity and is supported by the FREO2 Foundation, which presented its work at the UNICEF event.
“In a small health facility where they don't have any oxygen at all, a lot of children die and it’s really sad,” said Black, co-founder of the Australia-based foundation. “Health workers might say, ‘Here is a referral letter, we can’t treat your child here, please take your child to the district hospital,’ and parents say, ‘Thanks,’ and then realize they don’t have the money to get there. It’s complex.”
FREO2, which draws water from local river streams and uses it to produce oxygen, offers one solution for hospitals and health centers that do not have stable electricity flows, Black says. The device is now undertaking an ethics approval process, with the goal of finding partners to produce units that will be affordable for low-resource settings. This could also be beneficial to countries in conflict, which may lack stable electricity supplies but have the highest rates of pneumonia in children.
The Gates Foundation, meanwhile, is also pushing another protection measure already available, but not fully utilized: A largely effective pneumonia vaccine. It’s on the market, but only one-third of young children globally have been vaccinated, Klugman says.
“There are challenges in pneumonia diagnostics, which in some countries leads to a perception that the vaccine is not needed,” he said.
Support from Gavi, the Vaccine Alliance, has lowered the cost of the vaccine — hundreds of dollars when developed by a U.S. manufacturer in 2000 — to a more reasonable $10 for three doses.
But middle-income countries are not eligible for Gavi aid. The Gates Foundation is concentrating on encouraging local manufacturers to begin production of pneumonia vaccines in these countries.
“The problem is the middle-income countries, so there are countries really struggling and quite a lot of kids in those places, such as Indonesia,” he said. “They’re rich enough to not be eligible for the cheap vaccine, but poor enough there are a lot of kids still dying from pneumonia … India is in the same boat.”
Study of key age groups has also showed that toddlers are the biggest spreaders of pneumonia. If one or two doses of the vaccine are given to toddlers, this could likely maintain protection for entire populations, Klugman says, while also reducing the cost of the vaccine, which normally requires three doses.
“It’s a big deal,” he said. “That's a key thing for us, lowering the number of doses required as a strategy.”
“We might see increasing momentum to lift the number of doses in developing countries and then more of those countries could vaccinate their kids.”
Read more Devex coverage on global health.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5








