'World Malaria Report' calls for increased focus on pregnant women and children
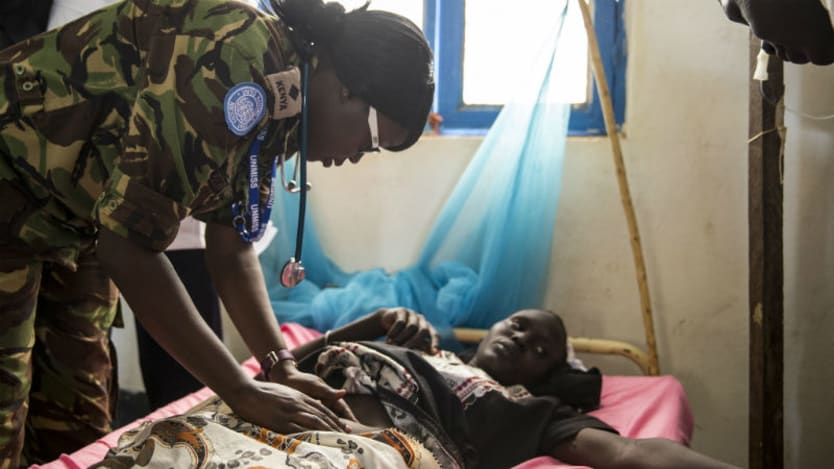
SAN FRANCISCO — Pregnant women and children are disproportionately affected by malaria, which can result in loss of life for the mother and the baby, the World Health Organization explains in its annual report on malaria data and trends.
“Putting back the focus on our highest risk groups — pregnant women and children — is not just an essential road to progress in the future but an ethical imperative to put the best of our resources to protect the most vulnerable ones,” Dr. Pedro Alonso, director of the WHO Global Malaria Programme, said in a call with reporters ahead of the release of the report.
“We also need to get better at identifying the people that global efforts are missing and how to reach them.”
— Dr. Abdourahmane Diallo, CEO, RBM Partnership to End MalariaThe “World Malaria Report 2019” highlights the consequences of the disease for maternal, infant, and child health: Last year, children under 5 accounted for 67% of all malaria deaths worldwide, making them the most vulnerable group affected by the disease. And 11 million pregnant women in sub-Saharan Africa were infected with malaria, increasing their own risk of illness, anemia, and death, and interfering with the growth of their unborn children, according to the report.
Taking a targeted approach
The WHO report provides a comprehensive overview of the status of efforts to eliminate the disease and calls on countries and development partners to prioritize support for pregnant women and children.
Improving access to existing tools — such as bed nets, rapid diagnostic tests, and treatments like antimalarials — and supporting a steady pipeline of research and development for new tools will reduce rates of malaria for all groups, including pregnant mothers and young children.
But WHO, which launched a new country-led response called “High burden to high impact” together with the RBM Partnership to End Malaria last year, is calling for a move from a one-size-fits-all strategy to a targeted approach to protect vulnerable groups.
“It is critical that we accelerate the rate of progress in the next few years to reach ambitious targets toward reaching zero malaria and protect the most vulnerable,” Dr. Abdourahmane Diallo, CEO of the RBM Partnership and former health minister of Guinea, said in an email to Devex. “We cannot leave anyone behind.”
For example, the global malaria community needs to scale up intermittent preventive treatment in pregnancy, which means giving antimalarial medicine to pregnant women at routine visits regardless of whether they are infected with malaria, he said.
In his foreword to the report, WHO Director-General Dr. Tedros Adhanom Ghebreyesus commended Sierra Leone for pioneering the delivery of intermittent preventive treatment in infants, a WHO-recommended approach, through its immunization platform.
And on Wednesday, the same day the “World Malaria Report 2019” was released, UNITAID announced a call for proposals to accelerate the scale-up of intermittent preventive treatment in infants in other malaria-endemic countries.
While Tedros called for more funding, explaining that total funding for malaria control and elimination in 2018 fell more than $2 billion short of WHO’s $5 billion target, he also emphasized the need for more effective use of existing tools and resources for malaria prevention and treatment.
“We need affordable, people-centered health services. We need reliable and accurate surveillance and response systems. We need strategies that are tailored to local malaria-transmission settings,” he wrote in the report.
Reaching the most vulnerable
Martin Edlund, CEO of Malaria No More, a nonprofit focused on ending malaria deaths, calls malaria “a disease of inequity,” and sees this report as further confirmation of that fact.
“Every year, global investments and actions save nearly 600,000 lives and prevent almost 100 million malaria cases,” Edlund said in a statement responding to the report.
“[But] too many people — especially pregnant women and young children in sub-Saharan Africa — are still suffering needlessly from this preventable and treatable disease,” Edlund said.
The report cites global progress on malaria, but that progress has been uneven, and experts say it is not happening fast enough for the most vulnerable.
Since 2004, nearly 2 billion mosquito nets, one of the most effective ways to protect against deadly mosquito bites, have been delivered to malaria-affected countries, Diallo told Devex.
The percentage of pregnant women and children in sub-Saharan Africa sleeping under insecticide-treated nets increased from 26% in 2010 to 61% in 2018, according to the report.
But that leaves nearly 40% of women not sleeping under nets, and nets alone will not solve the problem of malaria cases and deaths, Diallo said.
“Expanding access to quality health services to reach the most vulnerable populations with life-saving interventions is essential,” he continued. “We also need to get better at identifying the people that global efforts are missing and how to reach them.”
In areas where people are exposed to frequent malaria infections, they develop partial immunity to the disease during childhood, but children under 5 have not yet acquired that immunity.
Integrated community case management, which provides treatment of malaria, pneumonia, diarrhea, and in some cases malnutrition, has been identified as an effective strategy for reduction of under-5 deaths, said Dr. James Tibenderana, technical director at Malaria Consortium, in an email to Devex.
But most of these programs have not reached the scale they need to in sub-Saharan Africa “due to challenges such as ensuring reliable supplies of the necessary drugs and diagnostic tests, and appropriate support and oversight of the community health workers providing this care,” he said.
In the Sahel, WHO has called for seasonal malaria chemoprevention, full treatment courses of antimalarial medicine provided to children under 5 in areas of high transmission.
The intervention has been scaled up in 12 countries in the region, but more than 13 million children living in areas that could have benefited from this intervention were not covered in 2017, despite commitments from governments and efforts by implementation partners, Malaria Consortium’s Tibenderana explained.
While seasonal malaria chemoprevention has proven evidence of impact, the global malaria community needs to improve the quality of implementation by strengthening stock management, reinforcing training and supervision of health workers, and developing strategies for reaching populations that have not been treated in the past, he said.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5








