Africa CDC offers a slightly different take on AstraZeneca rollout
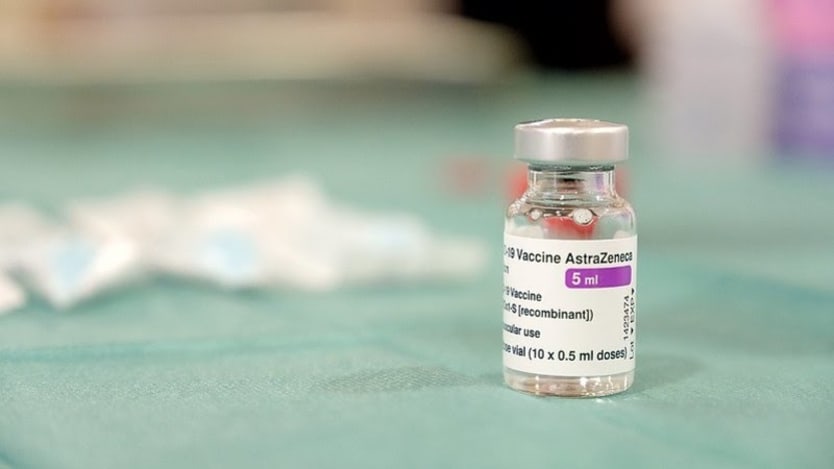
African countries where a certain variant of COVID-19 is dominant should not roll out the vaccine developed by AstraZeneca and the University of Oxford, according to Africa Centres for Disease Control and Prevention Director John Nkengasong, saying countries should still deploy the vaccine if the variant is not dominant.
“We will not be walking away from AstraZeneca at all,” Nkengasong said during a press conference Thursday. “For countries that have not identified this variant, there is absolutely no reason it should not be used there.”
This advice comes days after South Africa announced a temporary hold on the full rollout of the vaccine, in light of research finding it offered minimal protection against mild and moderate cases of the new variant B.1.351, also known as 501Y.V2. The variant, which was first identified in South Africa, is now dominant there, making up to 90% of new cases.
Africa CDC’s recommendations on the AstraZeneca vaccine differ slightly from those made by the World Health Organization on Wednesday, which called for countries to continue with plans to roll out the company’s vaccine but did not specify what countries should do if the new variant is found to be dominant domestically.
“While a vaccine that protects against all forms of COVID-19 illness is our biggest hope, preventing severe cases and hospitalization, which overwhelm hospitals and health systems, is crucial.”
— Matshidiso Moeti, Africa regional director, WHOPeter Piot, director at the London School of Hygiene & Tropical Medicine, said that WHO needs to make general recommendations, but “it’s not a one-size-fits-all at the moment.”
There are currently seven African nations that have detected the variant: Botswana, Comoros, Ghana, Kenya, Mozambique, South Africa, and Zambia. It’s also suspected to be circulating in Tanzania after two travelers from the country arrived in the United Kingdom carrying the variant, according to WHO Africa Regional Director Matshidiso Moeti.
Countries have varied in their response to the news out of South Africa. Eswatini said it will not use the AstraZeneca vaccine, whereas Kenya said it will.
Nkengasong urged countries to collect sufficient amounts of evidence to show that the new variant is dominant over the original form of the COVID-19 virus circulating globally.
“Having reported one or two cases in a country doesn’t mean the variant has dominated. We will only be cautious in areas that have an extensive takeover of the pandemic by this variant,” he said.
Nkengasong said South Africa is the only country that has thus far proved with adequate evidence that the dominant variant domestically is 501Y.V2. He said proving this should include studies tracking the variant over time.
But not all African countries have the in-house capacity to test samples of the virus to identify the variant through genomic sequencing. These countries are instead shipping samples to countries on the continent that do have capacity.
And even without a body of evidence proving dominance, health workers across the southern African region are reporting that the new variant, which is more contagious than the original, is spreading quickly and leaving health systems overwhelmed. In Mozambique, for example, case numbers are almost seven times higher than at the peak of the first wave of infections, according to Médecins Sans Frontières.
News of the vaccine’s minimal efficacy came only days after the COVAX Facility, the global initiative for equitable access to COVID-19 vaccines, gave countries notice about how many doses they can expect to receive in the coming months.
Nearly 90 million doses are forecast for the African continent, and the majority are from AstraZeneca. Delivery of the vaccine is expected to start before March. Countries were told that delivery is contingent on the vaccine receiving emergency use listing from WHO, which could happen this month.
Throughout the pandemic, the global health community has had high hopes for the AstraZeneca vaccine as a suitable option for lower-income countries because of the ease with which it can be distributed. It only needs standard rather than ultracold refrigeration, and it is affordable.
COVAX releases country-by-country vaccine distribution figures
Countries involved in the facility received estimates for the number of Pfizer-BioNTech and AstraZeneca-Oxford vaccine doses they should expect in the coming months.
The research out of South Africa found the AstraZeneca vaccine’s efficacy was only 22% against mild to moderate cases involving the new variant, which is well below the minimum efficacy threshold of 50% recommended for emergency use of vaccine candidates, Nkengasong said. Before the new variant became dominant in South Africa, the vaccine was showing efficacy for mild and moderate cases that was around 75%.
Protection against severe disease, hospitalization, and death could not be assessed in these trials because the participants were young and largely at low risk for developing severe cases. That’s an important factor to be explored with further research, according to health experts.
“While a vaccine that protects against all forms of COVID-19 illness is our biggest hope, preventing severe cases and hospitalization, which overwhelm hospitals and health systems, is crucial,” WHO’s Moeti said.
Instead of a full rollout of 1.5 million doses purchased for health care workers in the country, South Africa is using the AstraZeneca vaccine experimentally, inoculating only 100,000 people and monitoring them. It will now provide the Johnson & Johnson vaccine to its health workers.
Moeti said that “there is not very much difference” between the recommendations from WHO and Africa CDC, adding that countries should temper their expectations when using the AstraZeneca vaccine.
“We are not expecting now to reach rapidly herd immunity in countries where this new variant is circulating at a significant level. But if a country realizes it can benefit from preventing severe disease while understanding that the virus will continue to circulate … I think that’s perfectly acceptable,” she said.

Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5




