Malaria No More was founded by two prominent business leaders, Ray Chambers and Peter Chernin, who saw combating malaria as a unique opportunity to save lives and improve livelihoods on a global scale. As Chernin put it, ending malaria represents “the best humanitarian investment in the world today.”
It’s easy to see why. Malaria is a devastating disease and one of the top killers of children under the age of 5 and pregnant women worldwide. It’s also a huge drain on economies, accounting for approximately $12 billion in lost economic productivity in Africa each year, due to the burden it places on health systems and the toll of work absenteeism and missed school days.
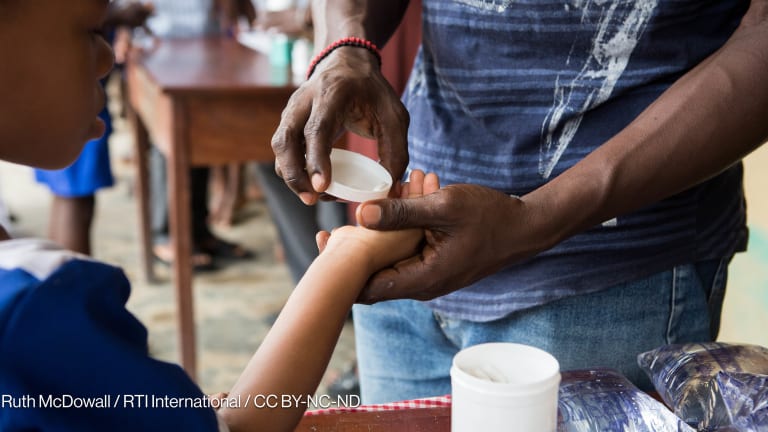
By contrast, the existing tools are simple and scalable — a mosquito net can protect a mother and child for three years for around $5; a 50 cent rapid diagnostic test and $1 treatment can save a child’s life — and as this series highlights, revolutionary new technologies are just around the corner.
When Malaria No More was founded in 2006, global spending on malaria was only a few hundred million dollars a year, and approximately a million people were dying from mosquito bites annually.
Through a massive global effort — including $3 billion in annual funding, led by the U.S. and U.K. governments, Global Fund to Fight AIDS, Tuberculosis and Malaria, World Bank, private sector and philanthropists — the rate of malaria deaths in Africa has been cut in half in under a decade. According to the World Health Organization, an estimated 3.3 million lives have been saved since the year 2000 from malaria alone.
Planning for a rainy day
The danger with malaria — the thing that keeps us malaria fighters up at night — is that if you lose focus, even for a single rainy season, the disease can come roaring back with devastating consequences.
There have been 75 documented instances of malaria resurgence from the 1930s to the year 2000, and nearly all of them were associated with the weakening of malaria control efforts. If we stopped investing in malaria control today, it would cause a massive humanitarian crisis, claiming millions of lives, and undo the hard-fought gains we’ve made in the past decade.
As the burden of malaria continues to be reduced, we need to shift from catalytic “scale up” funding models to sustainable, long-term approaches that will enable us to end the disease. That means diversifying the sources of funding so that the continued commitment of international donors is buoyed by growing domestic and regional investments, as well as innovative financing approaches. It also means using better data to find efficiencies that will stretch and strengthen the impact of malaria spending at the country level.
See more from this series:
● Solve for M: 5 key challenges to ending malaria
● Challenge 1: Find the parasite
● Challenge 2: Complete cure
● Challenge 3: Block transmission
● Challenge 4: Data and mobile
Put your money where your malaria is
We often say that malaria is both a cause and a consequence of poverty. But the reverse is also true: Malaria control is equally a cause and consequence of economic growth. It’s not just geography that caused malaria to be eliminated first in the United States in 1951 and most of Europe by 1975 — it was equally the result of economic growth, development and increased spending on health and infrastructure.
The current slate of countries moving toward malaria elimination — mostly in Asia and South America — are already covering the bulk of the expense themselves: Almost 80 percent of interventions are self-financed, according to a recent analysis by the University of California, San Francisco’s Global Health Group and Cambridge Economic Policy Associates.
In Africa, however, most countries still fall short of the self-declared “Abuja target” of dedicating 15 percent of domestic budgets to improving health. As “Africa Rising” moves from rhetoric to reality and economies on the continent continue to grow, Africa has the wherewithal to finance an increasing share of its malaria elimination ambitions. And it has powerful financial incentive to ensure the work continues — a recent study by Accenture estimated the present-day economic value (i.e., profit) of continued investment in malaria control in Africa at more than $322 billion between now and 2035, due to the tremendous health and productivity gains that would result.
Endemic countries also have the opportunity to stretch their budgets by working smarter. To the extent that countries can draw on good timely data to inform program decisions, they can save money by targeting the appropriate mix of interventions by region and setting. Zambia and Zimbabwe, for instance, have saved millions of dollars by using malaria risk mapping to optimize their net and insecticide spraying programs.
Particularly as countries reduce their malaria burden, one-size-fits-all, national-scale approaches may no longer apply. Namibia, a country moving toward elimination, has used malaria and mobility data to develop a more sophisticated, spatially targeted malaria program.

The future of funding
Regional financing mechanisms are emerging for countries, companies and philanthropists to invest in malaria control and elimination in their own backyards. Asia-Pacific has set the ambitious goals of eliminating drug-resistant malaria by 2020 and all malaria by 2030. To help finance the efforts, the Asian Development Bank and the Asia Pacific Leaders Malaria Alliance this year set up a regional trust fund to solve this pressing regional challenge.
Mechanisms for nontraditional donors to play a part in eliminating the disease are growing as well. In Indonesia, a small group of high net worth individuals have pledged to co-invest alongside the government and Global Fund in health priorities, while in the Philippines and Ghana companies with large local operations — the Pilipinas Shell Foundation and AngloGold Ashanti — have managed Global Fund malaria grants working hand-in-hand with government agencies.
Innovative financing efforts, including concepts such as development impact bonds, also have the potential to contribute. Creators of The Mozambique Malaria Performance bond aim to establish a sustainable new funding source that can also improve the efficiency of malaria programs through a pay-for-performance model.
It’s an attractive concept: Private investors front the costs of malaria control interventions to be repaid by a group of government and private-sector partners who reap the rewards of successful malaria control, including healthy citizens, employees and consumers. But we have yet to see investors step up to participate in such an instrument vehicle. If these models take root, malaria could evolve from being “the best humanitarian investment” to an actual investment opportunity — one that pays a dividend to those who contribute.
Achieving the historic goal of malaria eradication requires endurance. To sustain and extend the gains of the past decade, the global community must commit to providing predictable, sustainable, long-term support.
Our success in fighting malaria over the past decade has been built upon a solid foundation of funding, and the continued support of the U.S., U.K. and Australian governments; as well as institutions such as the Global Fund and the World Bank, will be essential to finishing the job. But we also need endemic countries and regions to commit to shouldering an increasing share of the costs as we move toward malaria elimination.
In the end, it will not be one sector or government that will finally eradicate malaria. It will be a global success — one we should all be proud to have contributed to.
This article is part of a series entitled Solve for M: 5 Key Challenges to Ending Malaria, hosted by Devex in partnership with Malaria No More and the Bill & Melinda Gates Foundation.
Join the Devex community and access more in-depth analysis, breaking news and business advice — and a host of other services — on international development, humanitarian aid and global health.