Health innovators seek more support as maternal, newborn deaths rise
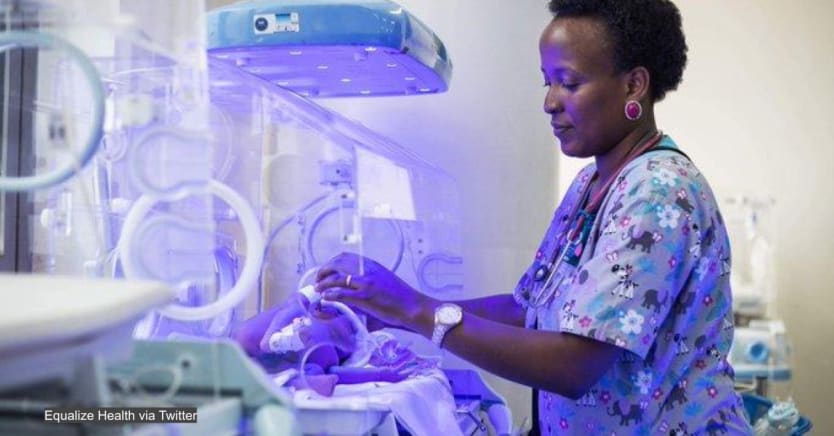
Neonatologist Donna Brezinski had to act quickly to get a second piece of equipment to save a set of jaundiced twins born at the small Massachusetts hospital where she worked.
The neonatal intensive care unit had just one of the blue light phototherapy devices needed to lower the dangerous bilirubin levels in their blood, which can lead to severe neurological problems or even death if left untreated. That experience a decade ago led Brezinski to research jaundice globally. She learned that more than 100,000 babies die of the condition every year, mostly in low-income countries and primarily due to delays in diagnosis and care.
She started working on an idea for a lightweight, collapsible, and portable unit that could run on a car or motorcycle battery and deliver high-intensity phototherapy far from hospitals in urban centers. It became known as the bili-hut, and Brezinski’s work evolved into Little Sparrows Technologies, a neonatal medical device startup.
The concept might never have left Brezinski’s kitchen table were it not for a $250,000 seed grant from Saving Lives at Birth. Launched in 2011 by a range of donors, including the U.S. Agency for International Development, the program supported innovations focused on the high-risk span of time from the onset of labor through 48 hours after birth.
Saving Lives at Birth provided seed funds, validation funds, and transition-to-scale funds, as well as nonfinancial support, including go-to-market strategies for primarily early-stage innovations in maternal and newborn health. Nothing else like it existed.
Though its donors renewed the program in 2015, the last of its eight open calls for innovations was in 2018. A USAID spokesperson said the Saving Lives at Birth partners are exploring how to support maternal and newborn health innovations moving forward.
The Gates Foundation's evolving strategy on MNCH Discovery & Tools
Dr. Rasa Izadnegahdar, director of the MNCH Discovery & Tools team at the Bill & Melinda Gates Foundation, expands on why the program has shifted focus toward addressing the underlying drivers of maternal and newborn mortality.
Little Sparrows Technologies used the seed money to pilot its units in Burundi. But now, the company is focusing on the United States, where the COVID-19 pandemic has created greater demand for decentralized health care solutions, such as portable phototherapy. While Little Sparrows Technologies remains interested in identifying a business model that can work in low-resource settings, it is no longer benefiting from the connections with other innovators that Saving Lives at Birth used to facilitate.
“We were ready to take the next step in expansion,” Brezinski said. “That abruptly ended, and there really hasn’t been any other forum that has consistently connected us. That, to me, has been the biggest loss.”
The timing could not have been more challenging for some of the innovators in the Saving Lives at Birth pipeline — and innovators in the maternal and newborn health space generally.
Since the beginning of the pandemic, there have been higher rates of maternal death and stillbirths, according to a new international data review from The Lancet Global Health. Disruptions to health services, lockdowns, and fear of visiting health facilities have led more women to deliver their babies from home, where there is a greater risk of injury or death, particularly in low- and middle-income countries.
The majority of newborn care facilities were not prepared to handle small and sick newborn care during the pandemic, according to another recent study.
Meanwhile, many philanthropic donors and investors who previously supported a range of global health priorities, including maternal and newborn health, have redirected their resources to COVID-19.
While new efforts are springing up to support maternal and newborn health innovations, entrepreneurs and funders tell Devex more is needed to bridge the gap between early stage research and development and real outcomes for mothers and newborns.
The need for sustained investment in innovation
The partners behind Saving Lives at Birth — USAID, Grand Challenges Canada, the Bill & Melinda Gates Foundation, and donors from Norway, the United Kingdom, and South Korea — funded more than 100 unique innovations. Now, they’re exploring how to get others involved.
“How do we think about fostering efforts to keep bringing in new players, new innovators, scaling partners, and new and different types of funders, including those from the private sector?” asked Meghan Majorowski, a senior adviser for USAID’s Center for Innovation and Impact, during an event highlighting learnings from a two-year evaluation of Saving Lives at Birth by Duke University.
Experts told Devex questions like this are part of a larger discussion among the Grand Challenges community of donors, which pool their funds to support a range of innovators, allowing them to take more risk at the portfolio level, knowing that not every innovation will succeed.
The $77 million that donors invested in Saving Lives at Birth is a fraction of what is needed to bring the most promising ideas through the final stages of development, let alone to scale and drive real impact for maternal and newborn health, said Wendy Taylor, who developed Saving Lives at Birth as USAID’s founding director at the Center for Innovation and Impact.
“Innovation requires ongoing, sustained investment and commitment from donors,” she said. “The key question we should be asking is: How much is enough?”
Taylor, now vice president for technical leadership and innovation at Jhpiego, a Johns Hopkins University affiliate focused on lifesaving services for women and families, called on donors to draw on lessons from the past decade to reimagine Saving Lives at Birth.
For example, she said donors might consider “including advance purchase commitments to provide market assurance that someone was going to purchase the product on the back end.”
Grand Challenges programs finance and often inspire innovations in the sectors they target. When they wind down, there are implications not only for the innovators but also for the implementation partners that support these organizations to understand their target markets, set up testing in the right geographies, or make connections with scaling partners.
“These programs are designed with the best of intentions,” said Maggie Flanagan, program officer at The Lemelson Foundation, a Portland, Oregon-based funder that supports invention, including hardware for unmet needs in maternal and newborn health. “There has to be a catalyst for innovation to solve a given problem. But I think it is valuable when donors are thoughtful about: ‘What role is my funding going to play? I catalyze it, and then what?’”
“How do we think about fostering efforts to keep bringing in new players, new innovators, scaling partners, and new and different types of funders?”
— Meghan Majorowski, senior adviser, USAID’s Center for Innovation and ImpactDiscovery, development, delivery
Without Saving Lives at Birth, innovations such as TempWatch, a newborn hypothermia monitor bracelet, might never have made it past back-of-the-envelope drawings.
Ratul Narain, founder of BEMPU Health, a company based in Bengaluru, India, received a $250,000 seed grant and a $2 million transition-to-scale grant from Saving Lives at Birth, which led to a partnership with UNICEF helping them reach 35,000 babies. It’s just one example of an innovation that the program helped on the path from discovery to development to delivery.
But the expertise for developing innovations is not the same expertise needed to get the technology in the hands of nurses, doctors, and patients, said Krista Donaldson, CEO at Equalize Health, formerly known as D-Rev, a nonprofit medical technology company based in San Francisco that also received support from Saving Lives at Birth.
She recently led her team through a rebrand, with a new name as well as an expanded mission of helping other innovators move away from lab-driven innovation toward innovations that are designed with user and market constraints in mind.
“Looking back at our work, one thing I was really frustrated by was the pace of product development,” Donaldson said. “The whole idea of our evolved model is we just really want to have more product development faster to have more impact faster.”
Now, it is expanding beyond developing innovations for maternal and newborn health — including its Brilliance device for treating newborn jaundice — to supporting other innovators tackling similar challenges. For example, Equalize Health is working with Justus Hofmeyr, a South African obstetrician and gynecologist, on his Safe Birth Tray for postpartum blood loss.
Donaldson said the gap left by the Saving Lives at Birth, combined with the fundraising challenges for maternal and newborn health during COVID-19, made the need for this kind of work all the more urgent.
Moving promising innovations through the pipeline
Some of the donors that supported Saving Lives at Birth are trying new strategies or introducing new initiatives to support innovations in this space.
New VC firm aims to boost financing for women's, children's health tech
Cross-Border Impact Ventures will invest in companies at or near the commercialization stage to bring medical devices, diagnostics, digital health services, and therapeutics to underserved markets.
For example, the Laerdal family — which is best known for inventing CPR training manikins and supported transition-to-scale grants for Saving Lives at Birth awardees — is behind a new $100 million venture capital fund that will back technology companies expanding health care access in a range of areas, including maternal and neonatal health.
The Gates Foundation has merged seven of its teams into a maternal, newborn, child health discovery, and tools portfolio, which focuses on addressing the underlying drivers of maternal and newborn mortality, and works closely with the maternal, newborn, and child health program strategy team.
And Grand Challenges Canada, which continues to support early stage innovators through its Every Woman Every Child Innovation Marketplace, is launching a new venture capital firm to invest in women’s and children’s digital health technology with dual-market applicability, in which a similar innovation can be used in both high- and low-income countries.
In addition, Newborn Essential Solutions and Technologies, or NEST360°, has raised $68 million for what it describes as a holistic approach to neonatal care. It has introduced lifesaving newborn health technologies and educated clinicians and technicians on how to use and maintain these tools — all while supporting innovators on the African continent to build the next generation of technologies.
But none of these initiatives offer a comprehensive platform with a coordinated and catalytic approach to innovation with the same model as Saving Lives at Birth, Taylor said.
She called on the global health community to keep up the momentum the program started, while iterating on the original model and leveraging new funding sources.
“We can’t afford to stop midcourse,” she said. “Many promising innovations are still making their way through the pipeline, and even better, next-generation ideas are yet to be discovered.”
Update, April 8, 2021: This story has been updated to reflect the number of innovations Saving Lives at Birth funded.
This coverage, presented by the Bay Area Global Health Alliance, explores the intersection between technology, innovation, and health. How are tech, innovation, and cross-sector partnerships being leveraged to accelerate equitable access to health care?

Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5