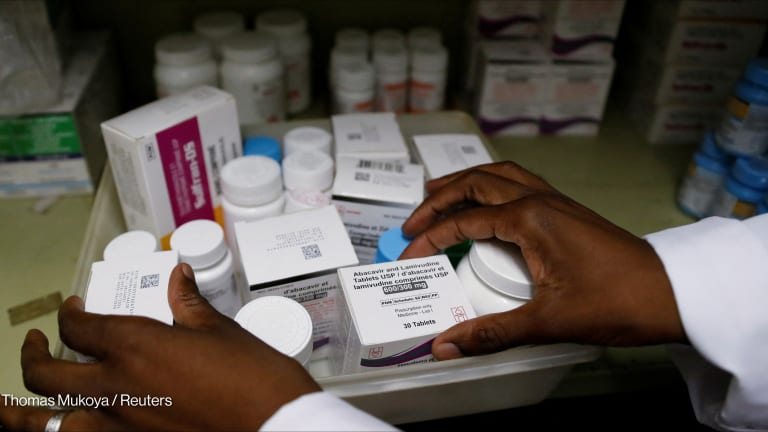
Kenya's blood bank unprepared for PEPFAR cuts, health insiders say

NAIROBI — This week, the U.S. government severed funds for the Kenya National Blood Transfusion Service.
While Kenya’s Ministry of Health reassured the public that services will continue uninterrupted, health actors told Devex that the government is not adequately prepared to fill the gaps. The Kenyan government reportedly asked for a six-month extension of funds from the U.S. President's Emergency Plan for AIDS Relief after learning of the cuts, but the extension was denied.
According to a PEPFAR spokesperson, this is a “long-planned” transition with the U.S. government working closely to prepare the Kenyan government for the hand-off. PEPFAR’s support for blood transfusion services in several other African countries has also been cut in recent years. The U.S. government has “largely transitioned this activity to host governments,” the spokesperson said.
Until now, PEPFAR provided the “bulk of funding to support Kenya’s blood collection and testing for HIV, HBV, HCV and Syphilis,” according to the Kenyan government. In fiscal year 2018, it provided about $1.4 million for blood safety activities in Kenya, according to a PEPFAR spokesperson. Moving forward, PEPFAR said technical assistance is no longer needed and the Kenyan government has picked up a greater share of the costs. It estimates the government will now need to absorb an additional $400,000 in commodities, personnel, and other blood safety-related costs per year.
Even with the U.S. government’s help, there have been massive deficits in the service. Kenya needs about 1 million units of blood annually, but last year collected only 164,275 units or 16% of the need.
What's behind PEPFAR's funding cut threats?
PEPFAR priority countries that are failing to hit targets are facing unprecedented cuts to their budgets this year.
There is concern in the health sector that the cuts will make the situation worse. Unsafe blood transfusions can lead to the spread of HIV, hepatitis B and C, and syphilis.
“There will be a lot of confusion and people running helter-skelter,” said Dr. Rowena Njeri, medical superintendent of a sub-county in Murang'a County, in central Kenya. “It’s only going to get worse. We are predicting an increase in mortality over maybe the next year until the government gets their heads together.”
According to Njeri, there are already blood shortages in some areas of the country, such as Kisumu in western Kenya.
“There are patients that are willing to donate blood. But you find that the facility and the blood transfusion units in the area don't have blood bags or the necessary equipment. It's not that there is a shortage of blood donors. There's just really no system to support the donation anymore,” she said.
Beyond the quantity of blood available to patients, there is also concern about the quality. Amref Health Africa, for example, was a recipient of PEPFAR funding for laboratory strengthening and providing technical capacity to public hospitals.
Amref is now working with counties to help them take over these responsibilities. “But we know that they might not have the capacity to do this,” said Antony Masika, blood safety officer at Amref Health Africa in Kenya.
Its regional centers were also dependent on PEPFAR for human resource funding, so it is expected that staff will lose jobs, which will impact the centers’ ability to operate at an “optimal” level, Masika said.
Government priorities
Since 2004, PEPFAR has provided programming focused on blood availability and safety in 14 sub-Saharan African countries with high HIV prevalence rates. The funds were used to help create national blood policies, improve donor screening, and increase donor recruitment, among other efforts.
For BIA subscribers: PEPFAR funding: Taking stock of the latest changes
To help understand PEPFAR's evolving business model, Devex digs into the available data to uncover key issues and trends shaping PEPFAR activities in Nigeria and Zambia.
Between 2004 and 2016, PEPFAR provided about $468 million in funding and technical assistance for these efforts. During that time, there was a 60% increase in blood supply and a steady decline in HIV prevalence rates in recipient countries, though HIV prevalence among blood donors remained higher than the World Health Organization recommendations.
PEPFAR has already successfully transitioned out of some of these countries. In 2016, the governments of Ethiopia, Swaziland, and Tanzania managed to completely absorb the cost of collecting and testing blood, according to an analysis from the Centers for Disease Control and Prevention.
But Kenya only received a quarter of its funding for blood transfusion services from its Ministry of Health in 2016. Health actors said a successful transition depends on prioritization.
“The government doesn't seem to place a priority on blood, but maybe that’s because it was heavily supported by PEPFAR,” said Julius Tome, project manager of Amref Health Africa in Kenya’s Sustainable Laboratory Quality Systems Project. “Now that [funding from PEPFAR] is going to be zero, they must do something. Blood is a necessity.”
Key to sustainability is ensuring that a sufficient percentage of the budget is automatically allocated to the Kenya National Blood Transfusion Service, Masika said.
A bill focused on blood donations that is up for parliamentary approval would “provide a robust legislative and regulatory framework that will aim to strengthen the current blood transfusion governance structures,” health cabinet secretary Sicily Kariuki said recently.
According to the PEPFAR spokesperson, the government should be able to take on this responsibility, “thanks to a decade and a half of U.S. government technical assistance.”
The government of Kenya “possesses the necessary technical capacity to autonomously and effectively manage this program,” the spokesperson said.
The private sector could also help to fill in gaps, some health actors said. Sisu Global Health, a medical device company, has a product called Hemafuse, which it launched in Kenya last year. It is used for autotransfusion — when a patient receives their own blood. While there are different types of autotransfusion, the Hemafuse method specifically targets emergency situations, such as ruptures or abdominal injuries.
It is not a replacement for donor blood, and cannot be used in all circumstances, but can be used to supplement the donor supply, explained Gillian Henker, co-founder and chief technology officer of Sisu Global Health.
Damu-Sasa, a cloud-based blood services information management system, is also working with Amref Health Africa on a system that supports “blood appeals, donations, screening, tracking, storage, distribution, transfusion and reporting.”
It was inspired by the Westgate Mall terrorist attacks in Nairobi in 2013, when there were “desperate unstructured appeals for blood and a slow response,” according to Amref.
The program was piloted at Kenyatta National Hospital, the nation’s largest public referral hospital, and is still running there.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5