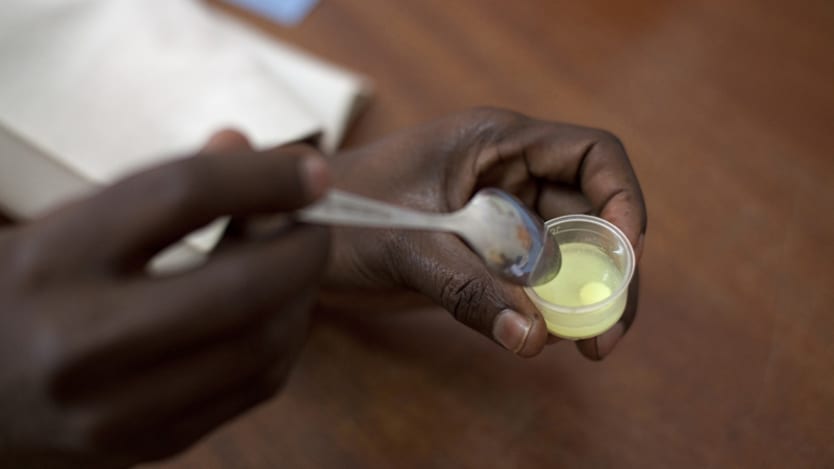
Imagine crushing a tablet, mixing it with water, then getting a child to swallow the bitter substance without spitting it out or throwing it up. This was the only option for children under five — an age group that accounts for 70 percent of deaths from malaria — until 2009, when antimalarial drugs were tailored to meet their needs. Two United States government agencies, the National Institute of Health and U.S. Agency for International Development, funded the development of Coartem Dispersible, a cherry flavored tablet that has saved the lives of an estimated 750,000 children since it was introduced.
But U.S. President Donald Trump’s proposed budget would reduce funding for efforts against malaria by 11 percent, raising concerns about the future of funding from the U.S. government, which is the largest donor for global malaria efforts.
Budget discussions on Capitol Hill last week indicated that malaria funding will remain consistent. But there has been a shift over the past decade from shrinking the malaria map to getting rid of the disease for good, and malaria eradication advocates say current funding levels cannot get us to that goal. The closer malaria gets to zero, the more difficult and expensive the effort to eradicate the disease will become, due to challenges ranging from drug resistant strains to weak health systems, they say.
“But [malaria] — as wily as it, as adaptive as it is, as longstanding as it is — is bigger than any one sector can deal with. This is something that takes all concerned actors in this space, whether they’re from the nonprofit sector, from communities of faith, from the government.”
— James Jones of ExxonMobilNow advocates who want to make sure the ongoing U.S. budget process maintains or even increases funding to fight malaria are pointing to a growing body of evidence about the return on investment in a disease that remains the leading cause of death in many developing countries. But the challenge remains that official development assistance is not growing at the rates that will be required to eradicate malaria by 2040. And while malaria endemic countries are increasing their financial commitments, that won't fill the gap left by a decrease in funding from outside donors.
Getting to zero
It was at a 2007 forum on malaria that Bill and Melinda Gates, the co-chairs of the Bill & Melinda Gates Foundation, sparked an industry wide change in the conversation on malaria, saying that any goal short of eradication is acceptance of the disease. Since then, Bill Gates has been among the global health leaders meeting with Trump to convince him of the value of U.S. foreign aid. Earlier this year, Gates launched the End Malaria Council, one of several efforts that aims to build political will and mobilize resources to accelerate the path to a world without malaria.
“The administration has a real opportunity to challenge the world to join us in a stepped up effort to end malaria,” said Chris Collins, president of Friends of the Global Fight Against AIDS, Tuberculosis, and Malaria. “This would mean increased investments from the U.S. and other donors, engagement in diplomacy to seek increases among donors, encouraging increased domestic investment where possible, leveraging private sector and development bank finance, engaging the private sector and incentivizing their involvement, and incentivizing innovative finance options.”
Gates and Ray Chambers, the United Nations secretary-general’s special envoy for health in Agenda 2030 and for malaria, released a report called “Aspiration to Action,” which lays out a vision for malaria eradication by 2040. They estimated that between $90 and $120 billion would be needed for the effort, which would save 11 million lives, and unlock an estimated $2 trillion in economic benefits from productivity gains and health savings. And they said eradication can only happen if malaria funding doubles between 2015 and 2025.
Experts told Devex this increase in funding will require a combination of traditional aid, domestic investment, private sector funding, and innovative finance, including blended finance and social impact bonds. But donor aid has unique strengths that are essential to effective efforts to end diseases and should rise rather than remain flat, Collins told Devex. He explained that in addition to being results oriented in terms of ending diseases, official development assistance can address the populations most at risk who may be most marginalized in their societies, does not demand a financial return on investment but can incentivize a health results return on investment, and can fill gaps where the private sector and innovative finance will not go.
See more related topics:
► Opinion: Using innovation and technology to tackle malaria
► Lessons from Sri Lanka on malaria elimination
Three promising developments in the malaria eradication effort include a greater focus on surveillance, increasing endemic country commitment and leadership, and tailoring elimination and eradication strategies country by country rather than taking a one-size- fits-all approach, Larry Slutsker, who leads PATH’s malaria and neglected tropical diseases programs, told Devex.
“Everyone who works in malaria would like to see an increase in funding, because the ability to go from point A to point B, high to medium or low, or from point B to Point C, low to very low to zero, is not necessarily a linear relationship,” he said.
But even before the uncertainty that came with the Trump administration, advocates of malaria eradication faced what is a growing political challenge, which is that elimination and eradication is a crowded space, he said.
The role of the U.S.
The President’s Malaria Initiative, which President George W. Bush launched in 2005, has saved 1.7 million infants and toddlers on the African continent, according to a recent study published by PLOS Medicine, a weekly medical journal, that evaluated the long-term effects of the program.
The new study, an independent analysis by economists from the University of North Carolina and Harvard University, was the first to assess the impact of PMI on child mortality in Africa, comparing the 19 countries that get U.S. malaria aid with the 13 that do not, and making adjustments to account for those lives saved by other interventions. The results debunk the myth that foreign aid has no effect because more children survive every year as economies improve, reads this New York Times story that is making the rounds among malaria advocates.
“PMI is a model of effective U.S. investment translating to impact,” Martin Edlund, chief executive officer of Malaria No More, told Devex via email. “It was started by President Bush, but has grown with the support of subsequent administrations and the Congress who respond to PMI’s clear objectives, measurable year-by-year progress, and enormous return on investment. This study is the latest evidence of that. We look forward to continued commitment from President Trump and malaria champions in the Administration and Congress to lead global efforts to save lives, stabilize communities, and end malaria within a generation.”
While Malaria No More is based in Seattle, Washington, half of its team works on advocacy, with much of that work focused on Washington, D.C. This recent study on the effectiveness of PMI demonstrates not only how foreign aid can save lives, but also how it can provide recipient countries with a more favorable impression of the U.S. That is a message that advocates for global antimalarial efforts from Malaria No More said they hope will resonate in an “America First” administration.
But even before the study came out, PMI had strong bipartisan support, in part because the initiative put a priority on documenting what it had done, USAID officials told Devex, reflecting on how Rear Admiral Tim Ziemer, the former coordinator of PMI, would bring graphs and charts demonstrating that progress into meetings.
It was welcome news to malaria advocates that Ziemer would join President Trump’s National Security Council as senior director for global health security and biothreats. But the organization has yet to appoint a new coordinator, pointing to one example of how unfilled positions at USAID and the U.S. Department of State might stand in the way of policy to eliminate malaria. Getting strong leadership quickly and firmly in place will go a long way in securing U.S. government support for malaria, advocates said, pointing to a letter in which 100 global organizations urged the U.S. Senate to swiftly confirm USAID Ambassador Mark Green.
“Like everyone else, the global health community is facing a tight budgetary environment,” said Margaret McDonnell, director of Nothing but Nets at the United Nations Foundation. “We are acutely aware of the fiscal constraints facing members of Congress, and embrace working with them and helping the new administration understand the proven benefits that come with funding malaria programs from economic to moral to diplomatic to protecting members of our military and other Americans who travel abroad. Concurrently, we are actively engaging members of Congress, as well as administration officials, about the value of working through the United Nations and other multilateral partners to leverage U.S. taxpayer money supporting malaria programs as well as other efforts such as protecting peace and alleviating poverty.”
There was not significant discussion of malaria last Wednesday, when the U.S. House of Representatives Committee on Appropriations approved a U.S. foreign affairs budget bill, as the disease is a relatively uncontroversial issue. The financial year 2018 bill would continue robust funding for the Global Fund at $1.35 billion, the same as enacted for financial year 2017, and for PMI at $755 million, the same as enacted for financial year 2017. But $250 million of the $755 million is provided through a one time transfer of unspent emergency Ebola funding, so it may take extra efforts to ensure the full $755 million in the Senate, and to secure this funding next year, Collins of Friends of the Global Fight said.
The Institute for Health Metrics and Evaluation Financing Global Health tool, which breaks down funding by source and health focus, demonstrates how the U.S. tops the charts for malaria. It is the top donor to the number one source of funding for malaria, the U.S. Global Fund to Fight AIDS, Tuberculosis, and Malaria, which has committed more than $10 billion to malaria programs worldwide. Next up is the second largest source of funding for malaria, bilateral aid from the U.S. And when it comes to the third largest channel for malaria funding — NGOs and foundations — the U.S. takes the lead once again.
Specifics of the growing funding commitments on a country-by-country level will be available later this year, due to work happening now from organizations including the Roll Back Malaria Partnership. But while governments of countries affected by malaria have increased their funding since 2000, this increase does not bridge the gap left by a decrease in external funding, which began in 2010 and is expected to decline further, according to a new study in Malaria Journal from researchers at the University of California, San Francisco Global Health Group. Experts told Devex that ending malaria is not a zero sum game, and that they hope to see increased funding from the U.S. government to affected countries and beyond, because a global disease demands a global response.
What lies ahead
Lessons from Ebola can help with malaria fight
Critical lessons from the Ebola outbreak identified by the World Health Organization can be applied to defeat malaria. And there are some warning signs on the horizon that we shouldn't ignore. An exclusive op-ed from Suzanne McCarron, president of the ExxonMobil Foundation.
In Angola, ExxonMobil is partnering with PMI and the government to take on a major challenge: The misdiagnosis of malaria. Together, they are working to improve the capacity of clinicians to diagnose the reason a child has a fever. Interventions such as these save the lives of children who might have another disease that would go untreated, prevents the problem of misdiagnosis worsening the problem of drug resistance, and builds the health infrastructure for diagnostics for other diseases.
“We’re a company whose business is to return an investment to our shareholders, and our business is frankly not to eliminate malaria,” said James Jones of ExxonMobil, which could make a business case for getting involved in malaria elimination once the disease stood in the way of a pipeline project from Chad to Cameroon, and has since became the leading private sector investor in eradicating the disease. “But this disease — as wily as it, as adaptive as it is, as longstanding as it is — is bigger than any one sector can deal with. This is something that takes all concerned actors in this space, whether they’re from the nonprofit sector, from communities of faith, from the government. Anybody who’s investing in, living in, working in, interested in a particular country that’s malaria endemic has a role to play in getting rid of this disease.”
The company has invested $160 million in the fight against malaria, distributed more than 14 million bednets, and reached more than than 125 million people. This is an effort the company sees not as corporate social responsibility but as core to business, in part because of the correspondence between the malaria map and the ExxonMobil operations map, Jones said. Now, the company is investing in the fight against drug resistant malaria partnering with organizations including Medicines for Malaria Ventures and the Worldwide Antimalarial Resistance Network.
“The last chapters of our fight will be the most difficult yet,” wrote Liberian President Ellen Johnson Sirleaf and and Dangote Group President and CEO Aliko Dangote, both members of the End Malaria Council. “Eliminating malaria in Africa will take bold commitments from African leaders in the public and private sectors.”We must double down on our existing malaria control efforts and think creatively about new funding sources, innovative new tools and unique partnerships to drive down cases and deaths and move more countries toward elimination.”
Last week, global health advocates have focused their attention on Washington, D.C., where former ExxonMobil CEO Rex Tillerson leads the U.S. Department of State, to try and convince the administration of the return on investment in global health. For example, “Return on Innovation,” a report released by the Global Health Technologies Coalition, explains how these investments not only drive global health outcomes, but also grow the U.S. economy, protect U.S. health and national security, and protect U.S. global development investments. The report offers key insights into the impact of U.S. investments in malaria: Since 2000, 82 new global health technologies have been approved, resulting in a 60 percent reduction in the number of deaths from malaria; and with $15 billion of investment between 2007 and 2015, the U.S. government has helped to advance 42 of these 82 products, which include 11 new products for malaria. New tools that emerge from the private sector — like a new insecticide-treated mosquito net from the German chemicals company BASF that has just received a recommendation from the World Health Organization — result from investments that were initially made by the public sector, experts told Devex.
As malaria funding advocates turn their attention from the House to the Senate, PMI is moving forward, with USAID officials telling Devex PMI expects to expand its geographic focus to additional countries, particularly in West Africa. Moving forward, PMI will continue to pursue reduction of mortality as its top objective, while also reducing morbidity and helping countries to take steps toward national and subnational elimination, they said. But the USAID officials added that, as the PLOS Medicine study demonstrated, the longer PMI is invested in a country, the better the results are, so in countries such as Nigeria and the Democratic Republic of Congo, which became PMI supported in 2009, the key will be to continue those investments.
When it comes to global health more broadly and malaria in particular, U.S. government initiatives including PMI are essential not only in derisking private sector engagement and investment, but also in strengthening health systems, which can help the global health community accelerate its path to progress on a wide range of diseases, USAID officials told Devex.
On Friday, PATH released a report on innovation for defeating malaria highlights tools, like artemisinin-based combination therapies, rapid diagnostic tests, and insecticide-treated bednets, as well as approaches, such as system and service innovations. It explains how Visualize No Malaria, a partnership between PATH, Zambia’s Ministry of Health, and the software company Tableau to provide software and training to health workers to track and treat malaria, has emerged as a model for ways public-private partnerships might work to tackle malaria in other countries. But Slutsker of PATH told Devex that that these partnerships also depend on sustained political commitment and funding, explaining that Zambia is a regional leader on the effort, with a strategy to eliminate malaria by 2021.
Another country that came up constantly in conversations about trends in funding for malaria was Sri Lanka, which is both a success story in demonstrating what is possible, and a cautionary tale in terms of why close to zero does not cut it.
Last year, WHO declared Sri Lanka malaria free, but it was not the first time the island nation had the opportunity to eliminate malaria. In 1963, the country was down to just 17 cases, but those never translated to full malaria elimination. It became the textbook case for resurgence of the disease.
Even now, donors tend to walk away when elimination is reached, and the 2016 World Malaria Report demonstrates how when the money leaves, malaria can return. While countries may try hard to remain vigilant, they need to have the resources to do so.
Read more international development news online, and subscribe to The Development Newswire to receive the latest from the world’s leading donors and decision-makers — emailed to you free every business day.








