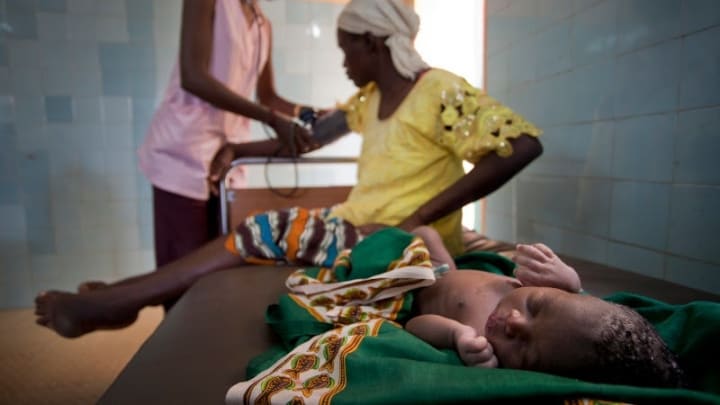
GLASGOW, Scotland — Disruptions to maternal health services over the last few months could endanger the lives of expectant mothers long after the COVID-19 pandemic.
Maternal health services take a hit amid global lockdown
With lockdown measures beginning to ease, activists across the global south are finally beginning to gauge the impact of restrictions on maternal health, even as they move quickly to prevent any long-term damage.
While there is still a lack of official data, anecdotal evidence suggests that the global health crisis is already having a devastating effect on pregnant women. Concerted efforts are needed now to ensure pregnancies are safe and wanted and to save lives, according to several sexual and reproductive health experts.
Anneka Knutsson, chief of sexual and reproductive health at the United Nations Population Fund, warned of a “women’s health crisis” that could evolve as a result of the pandemic. In April, the U.N. agency estimated that lockdown-related disruptions over 6 months could prevent 47 million women in low- and middle-income countries from accessing modern contraceptives, leading to 7 million additional unintended pregnancies.
Young girls, who face greater risks of complications during pregnancy and childbirth, are particularly at risk, Knutsson said. And an increase in child marriage, which is common in contexts where livelihoods are impacted, is likely to result in more young girls becoming pregnant.
Katja Iversen, president and CEO of Women Deliver, said there is evidence that a rise in unwanted pregnancies causes a spike in maternal deaths and unsafe abortions. She urged governments and agencies to safeguard maternal health funding and programming.
“We've seen it in previous pandemics — that resources were diverted away from maternal and, not least, reproductive health,” she told Devex. “Not only resources in terms of money, but also resources in terms of staff.”
Women’s rights and maternal health organizations are working to ensure funding for and access to critical services are maintained during the pandemic and incorporated into recovery plans. There are also opportunities to build on lessons that could strengthen maternal health care and the broader health system going forward.
Adapting and resuming programs
Even short-term disruptions to services and programming can have a significant impact when work resumes.
The Ebola crisis is evidence that service recovery can take a long time, Iversen noted. During that crisis, maternal and reproductive health staff members — many of them women — were among those who lost their lives after being transferred to front-line response work. Communities mourned these losses while struggling to get services up and running again within a depleted health system.
The importance placed on maternal health before the pandemic and whether there will be a second wave of COVID-19 infections are among the factors that will determine how quickly and effectively countries rebuild their services, Knutsson said. But with progress on maternal health indicators plateauing even pre-coronavirus, she stressed that minimizing service disruption is a priority.
“The more we can maintain services, the more we can actually support midwives to have the enabling environment they need to continue their services. And the more we can adapt services, the quicker the build-back will be,” Knutsson said.
UNFPA is striving to ensure that countries maintain critical services by providing personal protective equipment to health workers and disseminating information through various local networks so women and girls know when and how to seek care.
Organizations will have to be agile in using available data to adapt and repurpose programs to better fit the needs of women, Knutsson said. UNFPA has developed a number of technical briefs with advice on how to adapt services, such as training health workers to deliver contraceptive counseling over the phone.
In El Salvador, UNFPA is working with the Ministry of Health to implement a teleservice system for maternal and child care, while social media is being used in the Philippines to evaluate the impact of COVID-19 on unintended teenage pregnancies and preventable maternal deaths. Training is also being rolled out to facilitate task-sharing and to allow midwives to handle delivery complications in the absence of a doctor.
“If we're able ... to really support countries to be able to maintain the services ... to maintain maternal health care for women and girls at scale,” Knutsson said, “then we hope that we will see fewer or a lower increase in maternal mortality.” But, she added, “I do think that we will see an increase.”
Protecting policy and funding
Using a gender lens in COVID-19 response and recovery efforts is critical for reducing the long-term impacts on maternal health, according to Women Deliver’s Iversen. This is an opportunity to overcome some long-lasting barriers and build “better gender-equal services and gender equality,” she said.
Women Deliver has been working with high-level U.N. policy leaders to shape guidelines and frameworks that uphold maternal, sexual, and reproductive health and rights. The United Nations COVID-19 Response and Recovery Fund has a strong gender lens and gender marker, Iversen said, and it mentions safeguarding these types of services. However, more disaggregated data is needed to know whether a gender lens is truly being applied in national and subnational response efforts, she noted.
“The more we can maintain services, the more we can actually support midwives … to continue their services. And the more we can adapt services, the quicker the build-back will be.”
— Anneka Knutsson, chief of sexual and reproductive health, United Nations Population FundWomen Deliver’s teams are also mobilizing hundreds of civil society groups across health and other sectors to urge governments to adopt a gender lens in their recovery plans. Advocacy efforts elsewhere are focused on keeping funds earmarked for maternal health.
The economic situation facing many countries and the prospect of reductions in domestic and overseas development assistance is a concern, Knutsson said. A lack of funding has already forced UNFPA to suspend its reproductive health services in 140 health facilities in Yemen.
“If that happens in many more countries and there is not enough funding to support countries to maintain services, then the [post-pandemic] build-back again will be longer,” she said.
Opportunities to rebuild services
Lessons and innovations from the pandemic could improve maternal health care going forward. Telemedicine and apps have the potential to change how information is disseminated and how services, particularly those related to self-care, are delivered, Knutsson suggested.
In some countries, contraception can now be accessed through pharmacies with the support of an app, allowing people to ask for advice instead of having to visit a health practitioner. Of course, some situations will still require in-person visits, Knutsson noted.
There are also many takeaways from this pandemic that could inspire countries in rebuilding their health systems, she said.
The impact of the pandemic on maternal and newborn health will turn out less severe in some countries, which will allow systems to recover quicker, she said. It will be important to recognize the characteristics of these countries and to understand what work they had done previously to strengthen their health systems, as well as what actions they took during the pandemic.
Lessons around what makes women fear seeking health care, as well as the role of the wider family in decision-making, should also be built upon, Knutsson added.
One positive takeaway is that the crisis has highlighted the pivotal role of women — not just in times of crisis, but in everyday life, Iversen said. In rebuilding health systems, there should be a focus on universal health care that is women-centered, she suggested, adding that such systems would actually improve service delivery for society as a whole.





