Opinion: It's time for a new US cancer initiative in Africa

The World Health Organization estimates that cancer will claim the lives of 8.3 million people in sub-Saharan Africa over the next 10 years, surpassing HIV, which will claim 6.6 million lives during the same period. Without action, the overwhelming majority of Africans with cancer will not receive any treatment. But cancer’s devastating impact will linger for decades, as families cope with financial devastation and a generation of cancer orphans.
The state of cancer care in Africa is, in many ways, similar to HIV 20 years ago. Patients are diagnosed late in the course of disease, there is limited access to treatment — which is scarce and unaffordable — and, as a result, outcomes are poor, with high mortality for cancers that are survivable in other parts of the world. There is perhaps no better example of these disparities than pediatric cancers, with survival at more than 80% in high-income countries and less than 10% in East and West Africa.
The United States’ global health strategy has not kept pace with the changing epidemiology of cancer in Africa. U.S. bilateral development assistance for health in sub-Saharan Africa in 2017 totaled $4.3 billion, but just $1.2 million — or 0.03% — was for noncommunicable diseases.
As the country seeks to build global health leadership under the new presidential administration, a new U.S. cancer initiative in Africa provides an opportunity to lead boldly in an area of considerable need, to accelerate existing initiatives, and to build on the historical strengths of our HIV work.
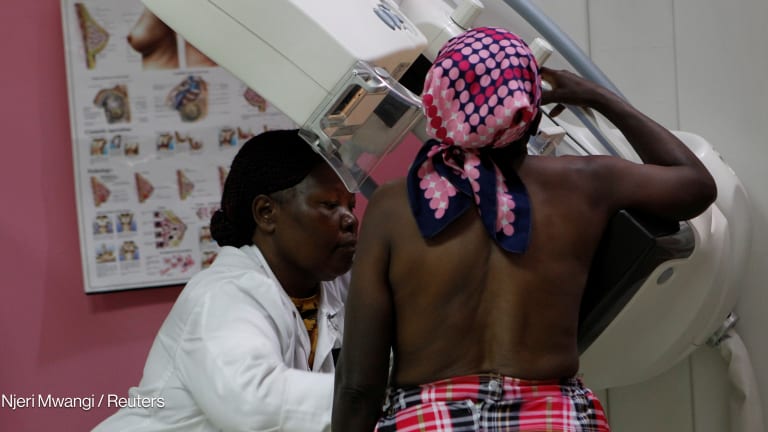
The case for action is strong. One-third of cancer deaths in Africa are due to cervical, breast, and prostate cancer, which can be prevented or treated when detected early. Many cancers can be effectively treated with surgery, off-patent chemotherapies, and radiotherapy, and survival can be boosted significantly by early diagnosis and treatment.
In sub-Saharan Africa, an estimated 29% of cancers have an infectious cause. Cervical cancer, the leading cause of cancer deaths in the region, can be prevented with HPV vaccination, which costs as little as $4.50 per dose.
The time for action is now. African governments are increasing their investments in cancer. Most have established national cancer programs, and there are now more than 30 cancer centers in the region.
The African Cancer Coalition has brought together more than 100 cancer experts from 13 countries to adapt dozens of U.S. cancer treatment guidelines for use in sub-Saharan Africa, creating practical clinical standards that are harmonized across the region.
And recently announced pricing agreements with international suppliers are bringing high-quality cancer treatments into the African market, at prices that are less than half of what they were previously. Significant investments can intersect with these efforts to rapidly accelerate the scale-up of cancer care.
Improving cancer care in Africa will require tackling challenges similar to those presented by HIV — in particular, needs related to training a new clinical workforce, strengthening laboratory systems, and addressing high treatment costs to make care more affordable. These are things the U.S. knows how to do well, because we’ve done them before.
As the country seeks to build global health leadership ... a new U.S. cancer initiative in Africa provides an opportunity to lead boldly in an area of considerable need.
—The U.S. leads in cancer care. Over the last 100 years, we have built world-renowned cancer centers, trained the leading cancer experts, developed groundbreaking treatments, and built vast and effective cancer research networks. We can harness this expertise and ingenuity to create the foundation for a new U.S. cancer initiative in Africa that is structured around six priorities:
1. Strengthening systems for cancer prevention and early detection through expanded access to HPV vaccination and scale-up of technologies for cancer screening and diagnosis.
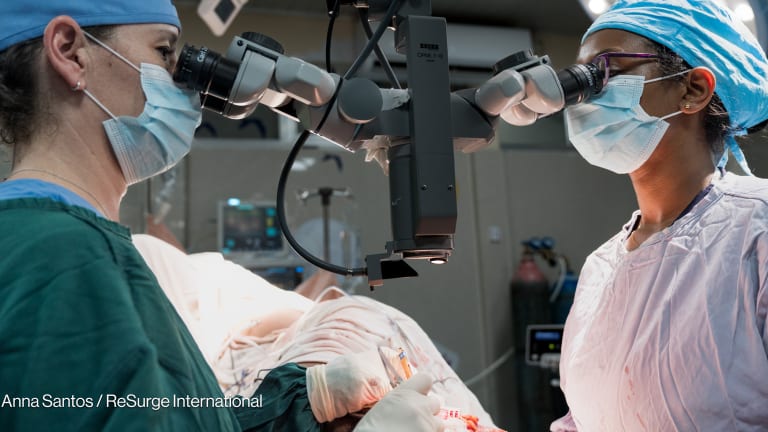
2. Investing in cancer treatment, including surgery, radiotherapy, and chemotherapies to give every patient a chance to survive.
3. Training a new generation of cancer health workers.
4. Implementing supportive care that enables patients to complete cancer treatment without delays or interruptions and that reduces suffering due to cancer.
5. Expanding investments in research to improve the quality, affordability, and availability of treatment.
6. Protecting patients from catastrophic financial impacts by reducing the cost of treatment and creating sustainable financing programs for cancer care.
The development of the initiative should begin with consultations with the leaders of African health ministries and cancer centers to ensure that the priorities and activities reflect their needs, and it should be designed to promote collaboration within the region and to build capacity within African institutions and organizations to lead the implementation of the initiative’s investments.
Cancer will be the defining challenge for African health systems over the coming decade, and it is time to update the U.S. global health strategy to include bold, ambitious efforts to address it through a new U.S. cancer initiative in Africa.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5