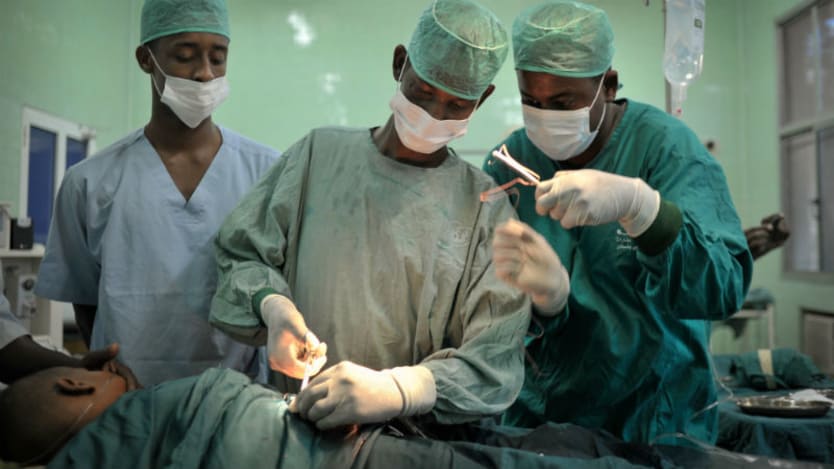
In recent years, Maroua, the capital city of the Far North Region of Cameroon has been in the news because of its role as the epicenter of the Cameroonian fight against the terrorist extremist group Boko Haram.
The mostly rural inhabitants of Maroua and its neighboring villages have been terrorized by Boko Haram for many years, with frequent bombings and kidnappings. The victims are often in desperate need of health care services. While the government and various NGOs have provided much-needed assistance to injured patients, many still die from treatable conditions because they do not have access to surgical care.
In February 2019, Charles Mbunwe, a 33-year old father of two, was working in Maroua for an international relief NGO that provides food, water, and agricultural tools to displaced people in northern Cameroon. He was returning from a mission to distribute livelihood products to rural inhabitants near the Cameroon-Chadian border and while riding in the back seat of a pickup truck, the driver lost control and the car hit a nearby tree. All five passengers immediately lost consciousness.
Scaling up basic surgical care in LMICs could prevent 1.4 million deaths.
— NCBIMbunwe was the first to wake and called out to a passing biker to ask for help. The man was able to mobilize a few other locals who came to rescue the victims, pulling the team out of the mangled truck.
Mbunwe and his colleagues were taken to Maroua Regional Hospital, the main tertiary hospital in the region. On arrival, Mbunwe was taken to the emergency department but there was nothing “emergency” about it. It was only many agonizing hours after being admitted that Mbunwe received his first painkillers. Basic amenities were lacking: “I remember being on an uncomfortable bed and my colleagues using stones to raise my head because there were no pillows in the hospital,” he recalled.
The hospital did not have an X-ray machine, so Mbunwe was transported to a private imaging center. However, the quality of the X-ray images was so poor that the doctors were unable to give a proper diagnosis.
Seeing Mbunwe’s critical state and that of his colleagues, his NGO decided to transfer them to Cameroon’s capital, Yaounde, a 30-hour journey by car. Using NGO contacts, it was able to arrange for them to be flown to Yaounde on a small passenger plane.
Achieving UHC in Africa requires support for most vulnerable, experts say
Affordable, quality primary health services for hard-to-reach populations often living below the poverty line is critical to achieving universal health coverage in Africa, yet experts warn the road to UHC for each country will be unique.
In a private hospital in the city, Mbunwe was able to get a good-quality X-ray and learned he had a right posterior hip dislocation. The hip was reduced under general anesthesia but the operation was not successful. He was told he needed a CT scan, but once again he would have to go to a private imaging center. The CT scans revealed that his hip joint had been fractured.
Mbunwe needed a total hip replacement and was finally able to undergo the procedure after six days. “The operation was very expensive and I was lucky that the NGO paid [for it],” he said.
Mbunwe’s story is important because it highlights four critical barriers to surgery that billions living in low- and middle-income countries face: capacity, timeliness, safety, and affordability. Using these criteria, researchers have shown that more than two-thirds of the world lacks access to surgical care, most of them in LMICs such as Cameroon and in rural areas such as Maroua.
Mbunwe was able to overcome all four barriers mostly because he was fortunate enough to be working for an NGO that was able to mobilize a plane for him to be urgently transported to a high-capacity private hospital and covered all related expenses.
Policymakers must act now to address this growing crisis for two reasons. The first is that too many Africans, especially youth, are unjustly dying or being disabled from conditions requiring surgical care. 1.4 million deaths can be prevented each year if populations of LMICs gain access to essential surgical care.
Secondly, improving access to surgical care will lead to increased economic productivity and development. Currently, most African countries rank lowest in the World Bank’s human capital index, indicating high losses in income due to human capital gaps. Most of those dying or being disabled from surgical conditions are young people such as Mbunwe who could be contributing productively to the economy.
A recent study by the World Health Organization shows that noncommunicable diseases and injuries account for more than 47% of the disease burden in the region, costing up to $1.4 billion lost in productivity each year. Improving access to surgical services will not only save lives but improve human capital, thus contributing substantially to economic growth in the region.
Ministries of health can act by prioritizing surgical care in their health care agenda by developing policies such as national surgical, obstetric, and anesthesia plans that systematically improve all aspects of the surgical system, including financial risk protection for patients.
They should also pay more attention to surgical systems by increasing financial investment needed for the implementation of these policies. Without investing in surgical care, universal health coverage in African countries, as well as many of the Sustainable Development Goals, will not be achieved.
We cannot rely on sheer luck for these stories to end well. There is an urgent need that we act to improve surgical services so that our lives are not gambled with.







