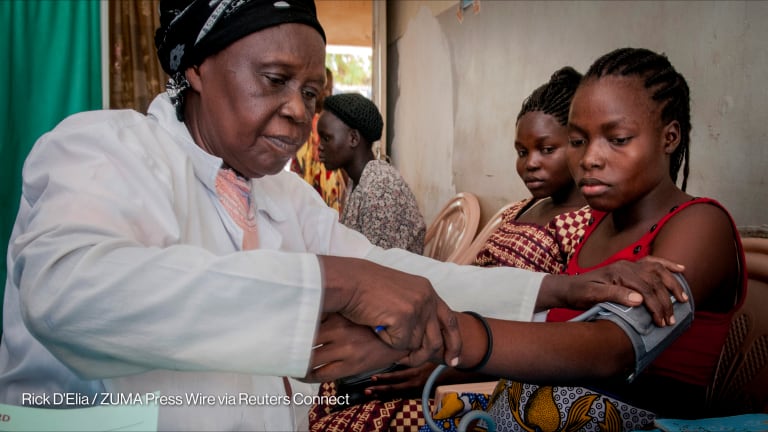Opinion: Planning for the next pandemic must start now. Here's how

The spread of COVID-19 over the last year is unprecedented, but it’s not the first time nations around the world have been — or will be — threatened by a public health crisis. In Asia and Africa, there are regular outbreaks of infectious diseases such as Ebola and malaria, for example.
To successfully combat these diseases and the next public health emergency, we must start planning now. The foundation of that planning requires a mindset shift: We have to move away from trying to fix the problem at hand and toward preventing the problem by building community and health system resilience. And we have to stop viewing people living in areas of need as merely beneficiaries.
Sign up for Devex CheckUp
The must-read newsletter for exclusive global health news and insider insights.
This mindset shift starts by finding ways to utilize a country’s existing infrastructure and its population to deliver information and services.
No one knows more about a country or culture than those who live there, work there, and breathe the air on a daily basis. Working side by side with trusted members of the community — including religious, community, and political leaders, as well as community-based organizations and educators — has a real and lasting impact on improving health.
But after spending more than six decades in many of the countries where we work, we can confidently say that developing this trust and these relationships takes time. And this is exactly why preparing for the next pandemic starts now. Here are three steps that are necessary to help establish and strengthen the delivery of health care services to communities in need:
Employ members of the local population. Rather than just partnering with leaders and the government, bring local community members onto your staff. They provide valuable insight into how their neighbors feel about global health situations, as well as how existing health infrastructure can best be utilized.
When a public health emergency occurs, local staff members will be able to stay on the ground and adapt existing programs and services, rather than simply abandoning their work and evacuating — something that outside organizations are often forced to do during times of great need.
We must take time to engage, build partnerships, and build trust with the people — and the communities.
—Adopt a culturally competent approach. Managing community-focused development requires time and energy to fully understand the people, customs, and existing resources that could facilitate or hinder enduring, effective, and equitable interventions.
Consider recent pushback in African nations from people who have refused a COVID-19 vaccine. Health care workers and leaders in these countries are battling misinformation and distrust, and much of this stems from viewing the population they’re trying to help as recipients rather than resources. This is a perfect illustration of why taking a culturally competent approach is so important, and why this is required for establishing or strengthening a health care system that delivers essential services.
For example, a COVID-19 outbreak that isn’t as severe in one area as it is in others may lead some to think the disease simply isn’t real. Gaining local perspective allows organizations to respond in a way that not only resonates but also leads to behavioral change, such as getting vaccinated.
Improve access to care. Because our staff is largely local, we learn of the unique concerns communities have when accessing care — especially regarding the COVID-19 vaccine. How can we expect people to get it if they lack transportation to a vaccination site that is typically in a larger city or town, or if they lack the broadband service or literacy to register for a vaccine?
The countries that don't want the COVID-19 vaccine
Some African countries have not made plans to inoculate their populations, but public health experts are calling on them to follow scientific evidence and give their citizens a choice regarding vaccination.
As health care providers and managers, we must listen to, reflect on, and understand those concerns — especially among those who have historically distrusted the medical care or health system and political leaders more broadly. And by relying on the expertise of those living in these areas, we can learn ways to modify the health care infrastructure to meet people where they are as much as we can.
Adopting a bottom-up, grassroots approach — as many organizations like ours have done — requires partnering with local leaders to build trust and deliver enduring change. Doing so provides a better understanding of existing systems and structures, how these systems and structures work together, and how the community interacts with them. Knowing who the trusted leaders are is a hugely important consideration when planning a response to the next health emergency.
As part of that plan, it helps to view community engagement from a programmatic perspective, remembering that for programs like these to be truly impactful, they must have longevity. Programs strongly rooted in the local culture can and will lead to behavioral change, of course, but that behavioral change will take time — and it will only happen with the buy-in and participation of the local community.
But to do that, we must take time to engage, build partnerships, and build trust with the people — and the communities. Only then can we start creating a healthier, and more resilient, global population.

Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5