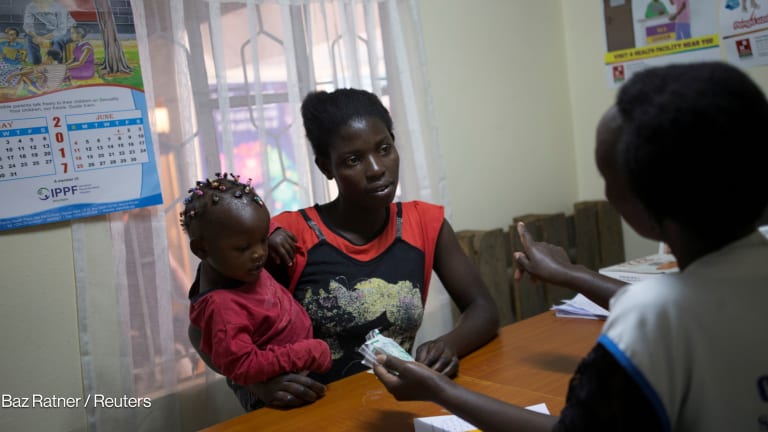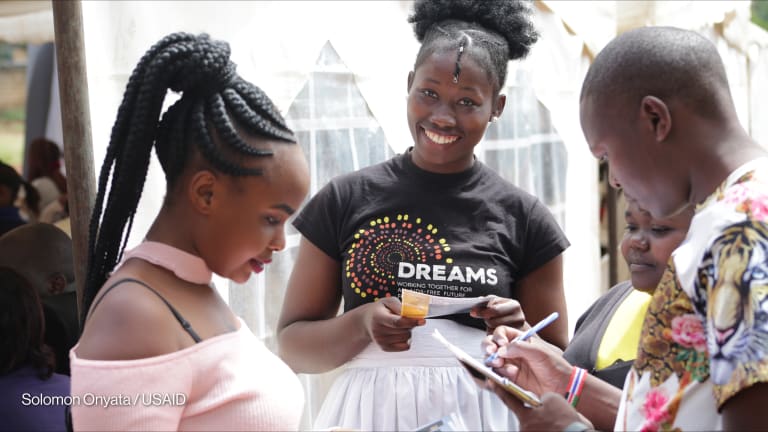Opinion: The 'global gag rule' hits PEPFAR implementers, study shows

This year marked the second anniversary of U.S. President Donald Trump’s reinstatement and expansion of the “global gag rule” — which bars U.S. global health funding to any organization that provides abortions, counsels or refers for abortion services, or advocates for access to safe abortion. A new report from amFAR shows how the policy, which has known detrimental impacts on the reproductive health of women and girls, is now also undermining U.S. investments in global HIV prevention, namely the U.S. President’s Emergency Plan for AIDS Relief.
Launched under the Bush administration, PEPFAR has been a bipartisan success story in the global fight against HIV. It is the largest commitment by any nation to address a single disease in history — and has transformed the lives of millions of people in countries most impacted by HIV/AIDS. In the wake of President Trump’s State of the Union address pledging to end HIV in the United States, evidence is now emerging that global HIV programming is being damaged by the global gag rule’s restrictions.
Minority groups excluded from global progress on SRHR, UNFPA report says
Despite global gains in securing sexual and reproductive rights over the past 50 years, many people are still left behind, according to UNFPA's "State of World Population 2019" report.
In the recently published study led by amfAR and Johns Hopkins University, nearly 300 PEPFAR implementing partners from 45 countries responded to a confidential electronic survey. The results were clear: The expanded gag rule has impeded the ability of PEPFAR implementing partners to provide full sexual and reproductive health services, disrupting the provision of contraception and HIV services.
While the effects of the policy were geographically broad, with impacts reported in 31 of 45 countries, many service disruptions were reported in sub-Saharan Africa, where HIV rates are among the highest in the world. Indeed, PEPFAR implementing partners in Kenya, Mozambique, South Africa, and eSwatini, where HIV prevalence in adult women ranges from 6.2% (Kenya) to 35.1% (eSwatini), reported the largest number of service disruptions from the gag rule.
Such a high disease burden among women is compounded by a high unmet need for family planning, which in turn contributes to unintended pregnancies and births among women living with HIV. Contraception is a known mechanism for preventing unintended pregnancy and HIV infections, with one study estimating that contraceptive coverage averts 173,000 new infant HIV infections in sub-Saharan Africa annually.
Even seemingly small reductions in contraceptive coverage in these high HIV prevalence contexts could have sobering implications for increased rates of new infant HIV infections. In our study sample alone, nine organizations reported reducing or stopping providing contraception, counseling, or referrals due to the gag rule.
In addition to contraception, PEPFAR partners reported reducing numerous other core health services including cervical cancer screening, condom provision, and HIV testing. Moreover, a lack of clarity on the policy’s provisions from U.S. funding organizations has led to over-implementation of the policy. Only 53% of survey respondents reported receiving any training on the policy from their U.S. funder.
Members of key populations, such as men who have sex with men, or MSM, people who use drugs, sex workers, and transgender populations experience the highest HIV rates in the world and frequently face discrimination, barriers to health services, and criminalization. Youth are also at disproportionate risk for HIV, especially in sub-Saharan Africa, where over 60% of the population is under the age of 25.
Survey and interview results showed that service disruptions caused by the gag rule are hitting youth and key populations particularly hard. For example, youth rely heavily on integrated delivery of family planning and HIV services since they often cannot afford to make multiple trips to separate health facilities. Since one of the outcomes of the gag rule is to deintegrate services, it is these populations that suffer the most.
Survey results further showed that PEPFAR implementing partners that serve MSM or pregnant women/girls were significantly more likely to report a reduction in operations as a result of the policy. This may be because the same types of organizations that serve key populations such as MSM are also more likely to provide comprehensive sexual and reproductive health information – including information on safe abortion services.
These disruptions have the potential to widen preexisting disparities in health access and to damage HIV service delivery to populations that need these services the most.
These results extend existing evidence showing the harmful effects of the gag rule on sexual and reproductive health outcomes to U.S.-funded HIV/AIDS programs. U.S. global health policy should be responsive to emerging evidence in the field in order to increase the effectiveness of U.S. investments.
One such policy initiative has been the recent introduction of the Global HER Act, which urges Congress to permanently end the global gag rule. This would ensure that U.S foreign assistance such as PEPFAR remains in the hands of the most effective partners in combatting HIV. Sound policy should be based upon effectiveness — not politics and ideology.
Update, April 17, 2019: This story has been updated to reflect that this year marks the second anniversary of the reinstatement of the global gag rule.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5