Opinion: Vaccine trials start and end with the community
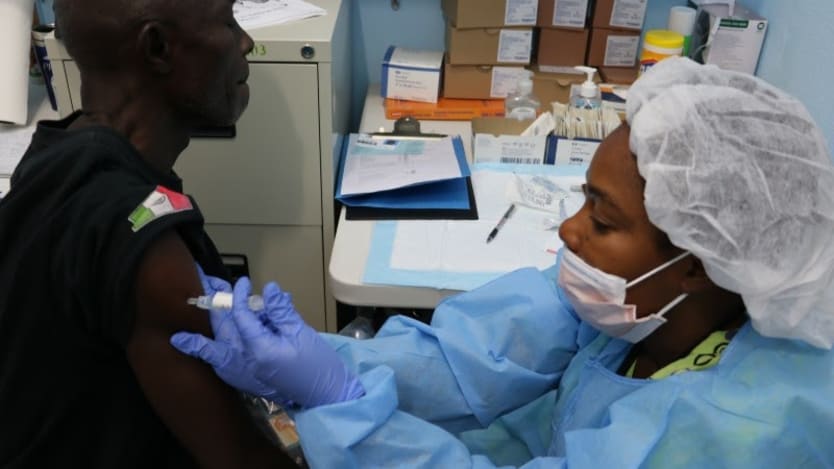
It starts and ends with the communities. Communities will drive the success or failure of the COVID-19 vaccine trials and immunization uptake. Scientists, policymakers, and public health experts must start involving communities now as discussions and plans progress toward finding a vaccine — not after the scientific breakthrough but before.
African Union aims to scale up COVID-19 vaccine clinical trials
A new consortium aims to help increase the number of COVID-19 vaccine clinical trials conducted in Africa, to ensure that any successful vaccines that come to market will work for African populations.
In recent decades, there has been a rise in anti-vaccine sentiments across the world. These sentiments have slowed acceptance of immunization services. In Uganda in 1997, for example, low coverage, below 75%, during National Immunization Days in eight districts was attributed to poor mobilization and community engagement, and also fuelled by rumors that the oral poliovirus vaccine was contaminated with HIV.
In 2019, aside from active conflict, Congo’s Ebola vaccine hesitancy was fueled by community distrust driven by the same social and cultural factors documented during the West Africa Ebola outbreak. As we saw, myths around vaccines and conventional health care ran deep in these communities, even though these were the communities with the most critical need for the Ebola vaccine.
The COVID-19 vaccine has not been spared these rumors. The proposal by some French researchers in early April to test the vaccine in Africa was met with warranted backlash across the world.
This has since heightened preconceptions against the COVID-19 vaccine trials, overshadowing the success of ethical and well-regulated vaccine trials which have been conducted in Africa. This is further fueled by rampant misinformation around COVID-19 disease itself. Past experience has shown us that communities must be first and at the center — end to end.
Just last week, as part of Africa’s Joint Continental Strategy for COVID-19 response, the Africa Union launched the Consortium for COVID-19 Vaccine Clinical Trial, which aims to rapidly secure more than 10 late-stage vaccine clinical trials and dismantle barriers related to vaccine trials.
This initiative has been welcomed by governments, donors, and research institutes across Africa. However, a strong argument can be made that the achievement of its six approaches will also depend on collaboration and cooperation with communities. Establishing partnerships, identifying trial sites, increasing public awareness, adherence to regulated trials, and scaling up vaccine distribution, will depend on communities’ acceptance of the COVID-19 vaccine trials.
Engaging communities
As the first COVID-19 vaccine clinical trial is rolled out at the University of Witwatersrand in Johannesburg, South Africa, what must be done now to include communities? How should we engage communities?
Researchers must engage with communities as they design and execute vaccine trials. Indeed, it is unethical for research teams to appear in villages without any prior consultation with the community with approved research protocols to “merely collect data.”
There is an overabundance of tools such as Community-based Participatory Research and use of the Participatory Learning and Action model — both provide useful tips for community engagement. Basic principles of empowerment demand that we involve communities as we conceive, design, and implement trials. This investment in community understanding of the research process as well as expected results and benefit leads to ownership.
Communities are by nature a complex web. Researchers must be mindful of this fact and interactions must carefully navigate these intricacies. This includes and is not limited to identifying community leaders to tailoring consultations, education materials, and other engagement tools to specific communities.
For example, there are significant differences between communities in rural areas and urban informal settlements, gated communities, farmers, nomads, and in some cases, notable intracommunity variations. In order to enhance public trust, communication should be multidirectional and strategies must be tailored specifically for the target population.
Most communities have solid structures and very influential “gate keepers.” As highlighted during the HIV vaccine trials in Tanzania, gate keepers are key in overcoming barriers to participation.
COVID-19 vaccine trials must leverage existing community structures such as community health workers, women and youth groups, religious, and traditional organizations which are can be hugely influential.
Accurate and timely information and reassurances about vaccine trials must be provided to these influential members of the community, throughout the trial duration. Understandably, research ethics require that each participant consent to participate independently. However, in many communities, critical decisions are taken by the family and/or community. Community ownership must precede individual consent.
Additionally, community concerns around the vaccine trial must be addressed as much as possible. Researchers must engage with communities and respond to genuine concerns, such as explaining what a trial means, and why are certain age groups targeted and not others — or discussing the anticipated side effects and how the information will be collected.
COVID-19 vaccine trials have just started. As we prepare communities it is the duty of government, the public health and scientific community, as well as policymakers and donors to consider low risk approaches with high yields.
Top of this is to create effective mechanisms for early community engagement as partners in the research process, not merely recipients of the results.
Key stakeholders should establish functional community advisory boards to enable reflective and systematic discussions between researchers and communities aiming to educate, improve practice, and drive positive impact in public health.
Communities must be first in science for its products to have acceptance and demand.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5










