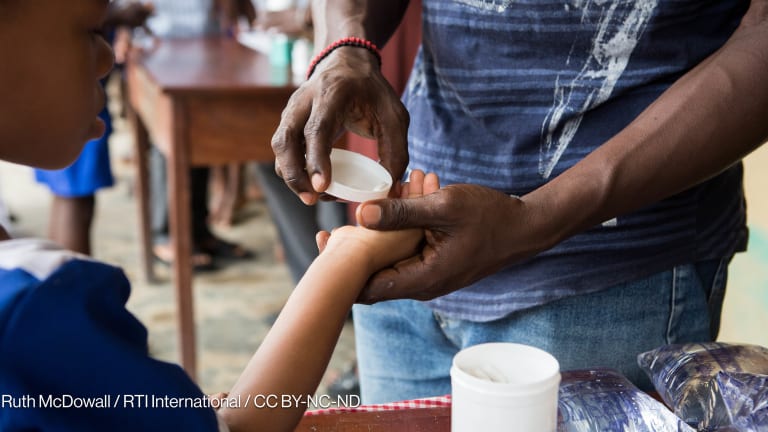
Universal health coverage is coming to the world’s developing countries.
As recently as a year ago, it was still uncertain whether UHC would gain enough support for inclusion in the post-2015 sustainable development framework. Today, as health groups recognize UHC Day, the argument on UHC “has been won, and won remarkably quickly,” as The Lancet editors put it. UHC’s place in post-2015 appears secure and the range of constituencies supporting UHC has grown considerably.
Bringing UHC to the global agenda has been an international collaboration. It’s created a large coalition behind the concept of health for all — bringing needed health services to everyone and reducing the financial burden of paying for care.
Printing articles to share with others is a breach of our terms and conditions and copyright policy. Please use the sharing options on the left side of the article. Devex Pro members may share up to 10 articles per month using the Pro share tool ( ).