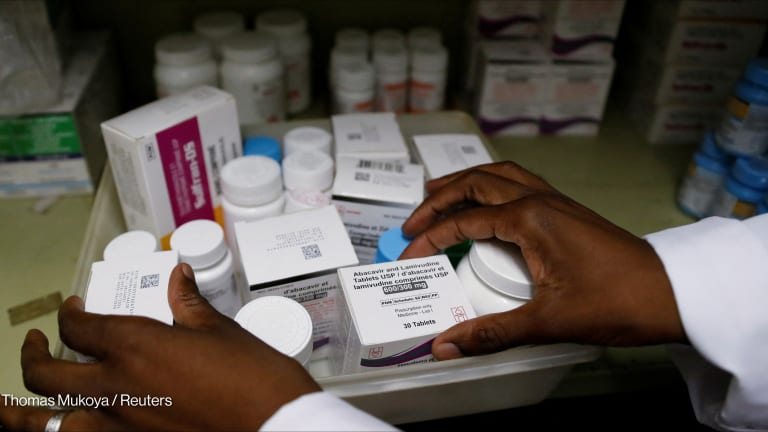
BALTIMORE — The United States government’s flagship global HIV and AIDS program is going local, even as its leaders try to figure out how exactly that will work.
Deborah Birx, the U.S. global AIDS coordinator, has directed U.S. agencies involved in the President’s Emergency Plan for AIDS Relief to reach a benchmark of directing 40 percent of their PEPFAR funding to “indigenous” organizations — those based in the developing countries where the programs are operating — in the next 18 months, and to reach 70 percent indigenous funding in the next 30 months. Birx shared those targets, which have not previously been reported, with attendees at the Christian Connections for International Health conference in Baltimore, Maryland, on Friday.
See more on the future of PEPFAR:
► 15 years later, PEPFAR is still at war with a global epidemic
► Long Story Short #17: 15 years of PEPFAR
► Uncertainty over PEPFAR support prompts concerns from HIV advocates in Nigeria
“If we’re going to have a sustained program, it has to be completely indigenous. We know we have to get to 100 percent — and I don’t mean as [subcontractors]. I mean as [prime contractors],” Birx said.
Currently, over 65 percent of the Centers for Disease Control’s PEPFAR funding, and less than 20 percent of USAID’s PEPFAR funding goes to local organizations, according to PEPFAR spokesperson David Haroz.
Shifting more direct funding to local, indigenous organizations will be a significant challenge for a U.S. global health system that currently leans heavily on large contracts, many of them managed by massive international organizations and contractors. PEPFAR commands more than $6.5 billion in annual funding, which is awarded through government agencies including the U.S. Agency for International Development.
Birx described an effort at CDC, where she previously headed up the global HIV and AIDS division, to shift funding to developing country-based organizations. That shift saw the agency dramatically increase the number of partners it was managing as it moved away from a system of large awards to large organizations.
“When we went to indigenous organizations at CDC, we went from 90 cooperative agreements to 600, which is hard to manage, I just have to say. But to really do it right, we would need 6,000 — if you wanted each of the individual key organizations to have direct funding,” she said.
“If we’re going to have a sustained program, it has to be completely indigenous. We know we have to get to 100 percent — and I don’t mean as [subcontractors]. I mean as [prime contractors].”
— Deborah Birx, U.S. global AIDS coordinatorPEPFAR is not the first to target a major “localization” push. Former USAID Administrator Rajiv Shah’s “USAID Forward” reform agenda sought to direct 30 percent of the agency’s funding to local organizations, while Shah famously declared, “this agency is no longer satisfied with writing big checks to big contractors and calling it development.”
USAID fell well short of that goal and ultimately backed away from the 30 percent target.
In recent months, PEPFAR’s single largest award — a $9.5 billion global health supply chain contract implemented by the American contractor Chemonics International — has drawn intense scrutiny and criticism from lawmakers on Capitol Hill, from USAID Administrator Mark Green, and from Ambassador Birx herself. In May, a USAID official told U.S. lawmakers that USAID has already, “started to aggressively apply lessons learned from this experience to the design of USAID’s next supply chain programs.”
On Friday, some attendees at the conference for faith-based organizations complained that their organizations struggle to access direct funding from PEPFAR, because these awards frequently require that prime contractors coordinate large-scale, centralized programs. Religious groups, on the other hand, tend to support health facilities and clinics that are dispersed across wide areas.
“We, as Christian organizations, have been scattered in all the regions, and we are having to work as subrecipients everywhere across the country, and that has been a very big challenge,” Tonny Tumwesigye, executive director of the Uganda Protestant Medical Bureau, told Birx.
In response, the PEPFAR chief pointed to the consolidation of U.S. HIV and AIDS programs under large awards as one factor in the difficulty decentralized organizations have in accessing direct funding.
“It’s what happened when mega contracts were created that required the people who bid on the contract to cover, not only a whole district, but a whole region,” Birx said.
Birx encouraged the assembly of faith-based representatives to consider how they might form coalitions or networks, which might collectively apply for awards.
“We know the communities of faith may have a hospital here, they may have a hospital over there in like three different districts. We still are working on a solution for that, and I think they’re going to have to find that solution because of our push to only fund indigenous organizations,” she said.
In addition to pushing PEPFAR’s funding agencies to shift money to indigenous partners, Birx said she is overseeing an effort to reassess the initiative’s support for community health workers — and particularly, to ensure PEPFAR’s country partners are paying their community health workers.
“Right now, many of our partners are using volunteer or stipend community health workers. That is not sustainable,” Birx said.
She stressed that the long-term viability of health programs in communities where PEPFAR currently operates will rely on investments in a community health workforce that can be sustained if PEPFAR’s presence in a country or community changes. Birx related a troubling example from South Africa.
“At one time, we were going to leave South Africa. There was a whole plan to decrease our funding in South Africa,” she said, likely referring to an Obama administration plan to “transition” the country from direct PEPFAR support.
“In that time, when it was thought that we were leaving, we had 10,000 community health workers that we were paying for. The first thing the government did was fire all the community health workers,” Birx said, adding that now PEPFAR is rehiring and redeploying them.
“It’s a good example for us that we have to create sustainable programs that the government also recognizes, so that 20 years from now, 30 years from now, those solutions are fully funded and respected,” she said.
At a separate session on Saturday, Yoram Siame, director of advocacy planning and development at the Churches Health Association of Zambia, described his organization’s frustration with USAID’s award-making process.
“My reflection on faith and work in health is that we suffer from a paradox of capacity. When there is no money, we do the work. When there is money, suddenly we don’t have capacity to spend the money. When the money finishes, suddenly the work is returned to the field,” Siame told USAID Deputy Assistant Administrator Alma Crumm Golden.
He cautioned that the “big decision in going local” was coming at a time when many organizations operating at a local level have developed a skeptical attitude about USAID funding and believe that “even when there’s a call for proposal, it’s just a formality. They’ve already decided.”
Siame related his organization’s experience of co-writing proposals with other USAID partners, only to see the funding picture change when those proposals get approved.
“When the proposal is approved, what you had proposed changes … then the funding comes out, and you find yourself out of the door, and the institution you wrote the proposal with gets all the money and starts implementing, and you are told, ‘USAID has said we can’t work with you,’” Siame said.
“From what I heard yesterday, and what I’m hearing today, you have very, very good intentions. The question is, how do we ensure that these good intentions get on the ground,” he said.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5