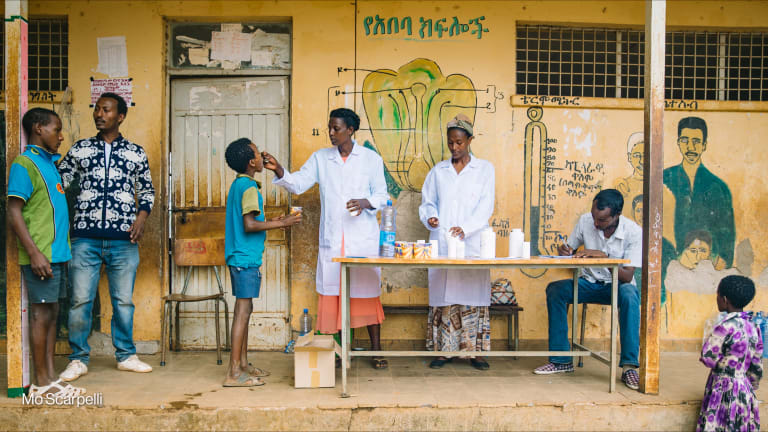
BARCELONA — South Sudan has succeeded in interrupting the transmission of Guinea worm disease, bringing the world closer to eradicating the incapacitating infection, it was announced last week.
The country’s minister of health, Riek Gai Kok, made the announcement on the sidelines of the Guinea Worm Eradication Program’s 22nd annual review, organized by The Carter Center and the World Health Organization in Atlanta, Georgia.
See more related topics:
► The rocky road toward disease eradication
► Exhibition aims to champion disease eradication as it happens
► Frontline workers push Guinea worm disease to the brink of eradication
► What lessons does polio eradication offer for global health?
South Sudan, which used to be the most Guinea worm-endemic territory in the world, reported no cases in 2017, down from 20,582 at the outset of the campaign in 2006. Because the parasite’s life cycle is about a year, a 15-month absence of cases indicates that transmission has stopped. The country now officially enters a three-year surveillance period that paves the way to certification as a Guinea-disease free country by WHO.
Guinea worm is one of two current disease eradication campaigns, alongside polio, and may become the second human disease in history — after smallpox — to be wiped out globally. Contracted by drinking contaminated water, worms of up to a meter long develop within the human body and emerge through painful blisters that leave patients unable to work or attend school.
Last year, only 30 human cases were reported from Ethiopia and Chad, compared to the 3.5 million cases in 21 African and Asian countries when The Carter Center began leading the international eradication campaign in 1986.
Speaking to Devex, Associate Director of The Carter Center’s Guinea Worm Eradication Program Adam Weiss talked about the keys to ending transmission in an unstable and low-resource environment; and what it will take to maintain the success. As the campaign strives for the finish line, he also discussed the biggest challenges, and how its approach can inspire efforts in global health and beyond. The conversation has been edited for length and clarity.
What have been the keys to stopping transmission in South Sudan, and to stopping it in spite of the instability and lack of infrastructure?
The most instrumental elements to the success of the initiative have been the leadership of the National Guinea Worm Eradication Program; the political commitment of the government; and the community health workers. Since the beginning, the program has been training local volunteers to identify people with the disease and to provide basic treatment and health education about how to prevent it.
You can have great leadership and all the political will in the world, but if you do not have the investment and buy-in from local communities, you are bound to fail.
How likely is it that the current conflict in South Sudan may have left cases undiscovered?
The political uncertainty and physical insecurity can make it difficult to access all parts of the country equally, so there is a valid concern about that. However, the authorities and the national program have implemented several interventions to ensure this is not the case. For example, there is open communication within the health system across invisible boundaries between opposition and government-controlled areas.
A national cash reward campaign has also launched to encourage people to come forward if they think they themselves or someone else might be infected. The campaign, which targets 80 percent of the population, offers the equivalent of $300 to $400 to any person that comes forward.
In addition to Guinea worm disease surveillance systems in both opposition and government-controlled health structures, there are a number of redundant mechanisms in place to help capture any potential case, should it occur.
“You can have great leadership and all the political will in the world, but if you do not have the investment and buy-in from local communities, you are bound to fail.”
— Adam Weiss, associate director of The Carter Center’s Guinea Worm Eradication ProgramThe international community, WHO, authorities and other partners, are leveraging any opportunity to ensure that no case would be missed. For instance, whenever they are working together to distribute bed nets, conduct immunization days for the eradication of polio or mass drug administrations for other programs, they are also asking about Guinea worm disease.
There is a great level of confidence within The Carter Center, the government, and the other partners that the country has done its job to ensure that transmission has not been missed.
How are you ensuring that there are no undiscovered cases among the South Sudanese that are currently displaced?
Surveillance mechanisms have been set up in all internally displaced people camps and in refugee camps, in collaboration with WHO and partners.
Over the last few days, we have received reports that all camps in neighboring countries are being screened on a regular basis for Guinea worm disease. No cases have been identified, so that is another positive sign that South Sudan has interrupted the transmission.
As South Sudan officially enters a three-year surveillance phase, what strategies will the national program and The Carter Center use to ensure certification as a Guinea worm free country?
Being in the precertification phase, South Sudan must now focus on the redundant surveillance systems that are available. This includes reporting structures within the ministry of health and across other organizations, whether they be NGOs, civil society organizations or bilateral partners working within the country or in refugee camps.
South Sudan must also focus on making sure there is a high-level of awareness about the basic signs and symptoms of the disease; how to report it should there be some case going forward; and what to do to make sure that person did not contaminate water sources.
The national program is going to shift its focus toward disease surveillance; cash-reward awareness; and to making sure that all surveillance structures and systems are documented, functioning at high levels, and have a monitoring and evaluation component.
What role will The Carter Center play in this precertification phase?
We will stand by the country as its key partner alongside WHO and our other partners. We will assist South Sudan technically, financially, and logistically to collect all the necessary information to support the surveillance systems so that we can validate that there are zero cases.
Globally, what is standing in the way of Guinea worm eradication, and what strategies is The Carter Center using to lead the international campaign to the finish line?
The greatest barrier is insecurity in the remaining endemic countries: Ethiopia, Mali, and Chad. International certification teams must be able to go and conduct assessments to evaluate the performance of national [Guinea worm eradication] programs and surveillance systems.
However, my personal opinion is that, even if insecurity persists, it is very likely that agreements can be found to give access to the certification teams when that becomes necessary.
A second challenge is [ensuring] the political will to support national programs in each country. If countries continue to increase their commitment and investment, they will see the dividends of that. Otherwise, that could delay the process.
Another setback is the Guinea worm infection in dogs, whose transmission must also be interrupted for a country to be certified as free of the disease. How are you addressing this challenge?
The biggest burden is in Chad, but smaller scale infections in animals are also being tracked in Ethiopia and Mali. We view it as a temporary setback, no different to discussions about monkeypox in the smallpox eradication campaign.
We are really starting to focus our attention on preventing infected animals from entering water sources so that we stop the [Guinea worm] cycle there. We cannot always control what a dog might eat, but we can work with the owners of infected animals to prevent them from going to the watersides.
Since its inception in 1986, the Guinea worm campaign has achieved a 99.999 percent annual case reduction. What strategies underpin this achievement, and up to what point can its principles and approaches be replicated by other global health initiatives?
A lot can be learned from how this campaign operates. It is an international campaign that is led by a Carter Center program, but that has been systematically embedded in governments [through national eradication programs].
First of all, it creates true partnerships with governments, not just partnerships on paper. That mutual respect and good will to work toward a common goal helps a program achieve its expected outcome.
Secondly, our program has proven that the community-based health care model is effective in implementing activities from the ground up. Because local agents already understand all the dynamics and social context of their community, you are able to expedite the process and also empower people from within to become leaders.
In addition, the [community-based health] structures that are put in place can then be leveraged by the greater health system. South Sudan, for example, is launching a Boma Health Initiative, akin to health extension workers in other countries.
Having very well-defined goals and standardized operational procedures and plans; maintaining strong supervision; and holding each other accountable are principles our program has maintained in each country over the years, and that helps you to be successful. That is a message that translates across and outside of global health.