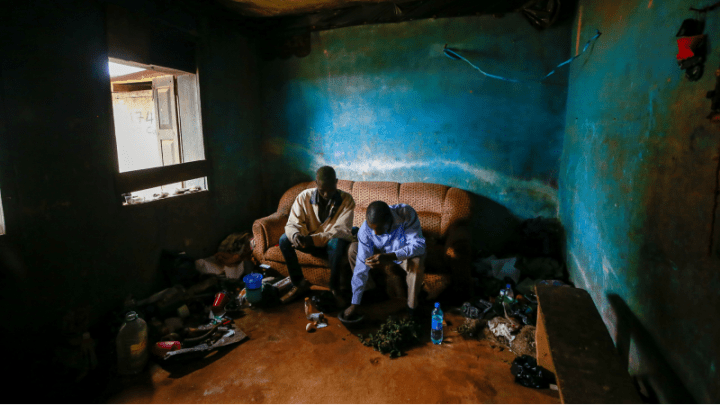
IBADAN, Nigeria — When Nigeria went into lockdown in March, 35-year-old civil engineer Joy Imisi found himself stuck in the country. He had made plans to travel to Ontario, Canada, to reunite with his wife and two sons, but the travel restrictions imposed to curb the spread of COVID-19 meant he had to postpone his plans until air travel resumed. The situation led to him experiencing depression and eventually turning to substance abuse as he struggled to sleep.
“I was all alone and I was unhappy. Probably the only time I wasn’t depressed was when I was under the influence of whatever I was smoking,” he told Devex.
In early July, Imisi — whose name has been changed to protect his identity — was referred to a primary health care facility for sleeplessness. The official on duty suspected that he may be suffering from mental health issues and referred his case to a secondary health facility where those suspicions were confirmed by a medical officer.
The officer gave him antidepressants and also recommended cognitive behavioral therapy with a psychiatrist. Imisi said the sessions, which were held virtually due to COVID-19, helped him to overcome his issues with substance abuse.
One in 4 Nigerians suffer from some sort of mental illness but according to Dr. Taiwo Sheikh, president of the Association of Psychiatrists of Nigeria, the country only has 250 psychiatrists to serve a population of over 200 million people.
Experts say an overhaul of the system is needed — but with this currently out of reach, Imisi benefited from a short-term attempt to solve Nigeria’s long-standing mental health care problems through a system known as task-sharing.
The model involves training other health personnel, such as community health workers, to identify mental health issues and provide basic interventions, thus reducing the number of cases that are brought to the very few specialists.
It is currently being tested in various parts of Nigeria and advocates hope that evidence on its efficacy will lead to a national rollout. Some challenges remain, however, especially around the integration of alternative health practitioners. These traditional healers are crucial due to their frequent interactions with mental health patients but often use controversial methods.
How it works
Victor Ugo, founder of the Mentally Aware Nigeria Initiative, a nonprofit organization fighting mental health stigma, explained that task-sharing relies on a working referral system, starting with the primary health care practitioners and alternative health service providers who often encounter patients with suspected mental illnesses first.
These practitioners then refer cases they cannot handle to secondary health centers, where there are medical officers who have also been trained using the task-sharing guidelines.
“We have ... bigger capacity to take on smaller cases because you have health care workers who are well versed in the knowledge of mental health and can ensure that early intervention is given from the start.”
— Victor Ugo, founder, Mentally Aware Nigeria InitiativeHealth practitioners “are trained in problem management and simple intervention therapy. They can provide you initially with some help,” Ugo said.
When the capacity of officers at the secondary health care level is inadequate to deal with a mental health case, it is referred to tertiary health facilities where there are specialists.
“That means you actually don’t have psychiatrists taking on every case, they only take the very serious cases. It means we have a much bigger capacity to take on smaller cases because you have health care workers who are well versed in the knowledge of mental health and can ensure that early intervention is given from the start,” Ugo said.
The challenge of alternative providers
Although task-sharing is not a complete solution for mental health care, research suggests it can be an effective intervention in resource-constrained settings, albeit with challenges, particularly around the impact on the workforce.
Olatunde Ayinde, a lecturer and consultant psychiatrist at the University of Ibadan, has been training primary health officers and alternative medicine practitioners in Ibadan, Nigeria’s third-biggest city, on how to integrate scientific methods in identifying and helping people with mental illnesses.
Ayinde believes the task-sharing model has proven highly successful within the public health referral system, despite challenges around the lack of resources to enforce a required standard of care, and that in the short-term it can improve access to care for individuals like Imisi.
He said the approach has been particularly helpful in addressing depression among expectant and new mothers.
“Under the program, psychiatrists train primary health care workers ... to deliver interventions for pregnant women and women who just gave birth and have depression. This has been shown to work in Ibadan. A lot of such interventions are going on around the country,” he explained.
But it is working with alternative medicine practitioners that has been the biggest challenge.
These practitioners are an important part of the program since relatives will often take mental health patients there first. However, there are concerns that the model could potentially validate their approach to managing mental illness.
Kolapo Mojeed heads a group of spiritual psychiatric healers in Ibadan. Even though he has received training from Ayinde’s team, he said he still believes that mental illness is caused either by spiritual affliction or by drug abuse. He remains actively involved in practices such as shackling patients — which is widely condemned by mental health experts — while brandishing certificates from training conducted by Ayinde’s team and other government intervention programs as evidence validating his methods.
More on mental health:
► Opinion: Depression, anxiety, insomnia — health workers and the side effects of COVID-19
► Health workers speak out on the need for better mental health support
Research done by Ayinde and his colleagues acknowledges that the harmful practices sometimes used by alternative practitioners are a major obstacle to their integration into mental health care in Nigeria. These practices include shackling or even beatings and scarification rituals, which “reflect erroneous beliefs … about the underlying causation of mental health problems,” according to their report.
Nonetheless, in some cases, the collaboration with alternative practitioners has worked, he said, and has greatly extended the program’s reach.
“There are way more traditional healers than psychiatrists in Nigeria. The available beds with them outnumber ours 10 to 1,” he said.
Ayinde said his team is closely monitoring their trainees and addressing issues on a case-by-case basis, but that they are still learning about how to handle this dilemma.
Despite the challenges, he believes task-sharing can be an effective solution to improving access to mental health care in Nigeria.
“We have demonstrated that task-sharing can happen in a control setting and in a real world setting and is cost effective. We are in the process of gathering all the evidence and ensuring that it will work before recommending that it be scaled up. All our results have been very encouraging so far,” he said.
Visit the Duty of Care series for more coverage on how health systems can function better so that health care workers are supported and protected. You can join the conversation using the hashtag #DutyOfCare.





