Opinion: The secret to increasing global access to health care

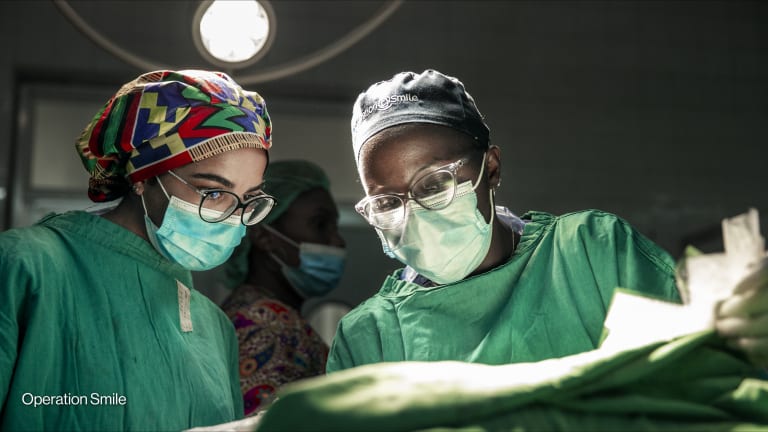
Nearly 5 billion people across the world lack access to safe and affordable surgical care. This burden is felt most acutely in low- and middle-income countries where — among many health emergencies and needs — untreated birth defects impact individuals’ abilities to pursue education or professional opportunities.
Globally, it is estimated that one child is born every three minutes with a cleft lip and/or palate — more than 170,000 a year, with 94 percent of these congenital anomalies occurring in low- and middle-income countries. In developed countries, with greater access to surgical and health care, a cleft lip and/or palate is often addressed at a very early age. But for many children in developing countries, where the correct surgical care can be a big task to provide, an untreated cleft leads to difficulties eating, breathing, hearing, and sometimes even speaking. As a result, these children are commonly ostracized from their communities.
Is it possible to deliver health care in developing countries and remote areas 365 days a year? Yes, by building local medical professionals’ capacity.
At Smile Train, we believe in this train-the-trainer approach. Our model has been proven to successfully deliver long-term surgical aid in developing countries, according to the Journal of Craniofacial Surgery. Researchers have found that a model that prioritizes empowering local medical professionals increases the number of procedures per hospital per year, decreases patient waiting lists, and accelerates patient follow-up.
At Smile Train, our partnership model and training approach has allowed us to provide more than 1 million children with life-changing, and free, surgeries since 1999, in more than 85 countries. Rather than swooping in to provide interventions and then leaving the communities, Smile Train works to elevate local expertise by strengthening surgeons’ skills and increasing the level of care in local hospitals.
Given our nearly 20 years of success, here are three key lessons Smile Train has learned about how to improve access to health care in developing countries, which we think could be applicable to any nongovernmental organization with a similar goal.
“Is it possible to deliver health care in developing countries and remote areas 365 days a year? Yes, by building local medical professionals’ capacity.”
— Susannah Schaefer, executive vice chair and CEO, Smile Train1. Bolster local health care capacities in developing countries.
Our model is not just about providing cleft repair surgery and comprehensive cleft care. Ultimately, we prioritize training local health care professionals on cleft repair procedures. We do this in part through our Virtual Surgery Simulator, a 3D simulation technology that simulates leading complex cleft surgical procedures. The software is multilingual and accessible to surgeons worldwide. By bolstering local surgeons’ skills, we also seek to improve the quality of care provided at partner hospitals beyond cleft repair surgery. To participate as a Smile Train partner hospital and receive our training resources, the quality of care across all treatments needs to meet a specific standard. This helps elevate care across the board at any of the participating facilities. We suggest that when and if possible, organizations assess how they can increase local capacities to ensure the community benefits long term.
2. Balance between a laser-focus on one key vision, while also providing additional supplementary patient resources.
Performing surgery is just one small part of helping children living with untreated clefts. The recovery process and ongoing care is equally important. That’s why we don’t just focus on getting the surgeries done; we have identified other health care and therapeutic resources that help cleft patients recover faster. For example, where the resources are available, we offer post-surgery speech therapy for patients who may continue to experience language delay challenges with speaking. If needed, we provide dental and orthodontic care. And recognizing that some patients may be so malnourished that they cannot safely receive surgery, we provide adequate food and nutrition support as needed. We can — and do — have a singular focus, but we remain aware of the other issues that impact the patients we serve and recommend that all nonprofit organizations take a similar approach.
3. Emphasize the importance of local relationships.
Training local surgeons to deliver cleft repair surgeries increases the likelihood of patients benefiting long term. Each community and culture has its own set of unique needs, concerns, and customs. Empowering partners at the local level allows us to focus on context-specific problems and solutions, rather than employing a one-size-fits-all approach to global health. Encouraging the development of local relationships, in our experience, leads to long-term solutions for patients and communities alike.
All in all, we have offered local doctors 40,000 virtual cleft training opportunities and have reached tens of thousands of medical professionals worldwide since inception. And as the Journal of Craniofacial Surgery found, the results speak for themselves, with an increase in the number of surgeries performed and in the complexity of cleft repairs that have been able to be addressed. This model has also seen decreased waiting lists for treatment and improvements in follow-up care over time.
Our approach has helped us change the lives of so many children and their families, and we work every day to increase our reach. But ultimately, with Smile Train’s model, we work to empower communities to become less dependent on outside aid over time, creating a sustainable response not just to cleft lip and/or palate — but other pressing global health care issues as well.
To learn more about Smile Train, click here.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5