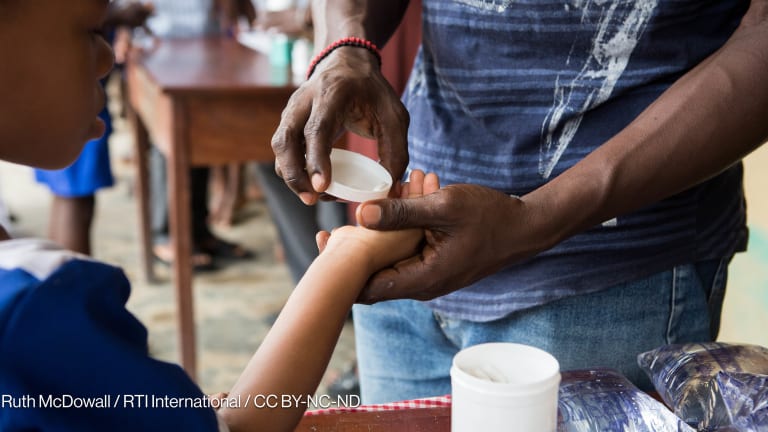
When it comes to medical products and pharmaceuticals, each country is required to have a system that regulates those products, authorizes what can enter their market, and prevents substandard and falsified medicines from reaching health care facilities and dispensaries. This can be a lengthy, demanding process that requires considerable financial and human resources.
One solution could be continental harmonization — the streamlining of regulation systems across multiple countries. While Europe fostered this approach many years ago through the European Medicines Agency, Africa still lags behind. Margareth Ndomondo-Sigonda, head of health programs at the New Partnership for Africa's Development Agency, asserts that this needs to change. Although medicine regulatory harmonization has achieved success over the past decade or so, there is a need to sustain this momentum, and use lessons learned and best practices from proven initiatives as a precursor to establishing strong continental regulatory institutions.
“If you don't harmonize, if each country is doing things in their own way, the chances are that — because of the capacity limitations in those countries — you have a situation where products needed by people in that country may not be easily available because they are not allowed to be marketed,” she said.
“Use the same standards, use the same procedures, conduct joint evaluations, agree that the product is authorized to go on the market across countries — that’s harmonization.”
— Margareth Ndomondo-Sigonda, head of health programs, NEPAD AgencyNdomondo-Sigonda explains that if a robust system for market authorization is not in place, new medicines cannot enter the market and people can be subjected to substandard products that could harm their health. The solution: pooling resources, speeding up the approval process, and getting people the care they need by harmonizing regulation and authorization systems across the African continent.
“You’re looking at the same things: whether the product is good and whether the product is actually effective — those standards are international,” she said.
Speaking to Devex, Ndomondo-Sigonda explains why improvement in medical products and pharmaceutical regulation is vital and how harmonization can be achieved.
Below are highlights from the conversation, edited for length and clarity.
What are some of the most pressing issues in Africa around the regulation of medical products?
As far as regulation of medical products is concerned, one of the pressing issues at the moment is really that of substandard and falsified medicines in circulation on the African markets. There is a prevalence of 25 to 30 percent of substandard and falsified products on the market and, of course, this is posing a big challenge in terms of public health because sometimes the public is subjected to these medicines, which can be very harmful.
Secondly, we have an issue around the different requirements for the registration of medicines. That means the industry finds it very difficult to get products into the market. This poses a challenge when it comes to availability of the most needed medicines, especially new products.
Generally speaking, all of this is compounded by the capacity limitations we see in most [African] countries — they either don't have appropriate frameworks to regulate medicines, the laws are outdated, or just not comprehensive enough. You also have countries that don't have enough resources to invest in institutions to regulate medical products and often there’s not enough human resources — in numbers but also in terms of competency — to be able to run these regulatory affairs.
What key actions have African stakeholders taken to address these problems thus far?
Various interventions have already been started and have been going on for many years. I recall back in the 1990s, in the Southern African development community, there were initiatives to harmonize the requirements for the registration of medical products through a methodical platform. This allowed countries to use the same set of standards. In the East African development community, in the early 2000s, policymakers also decided they needed to embark on harmonizing regulatory requirements, so countries began coming together through a platform to regulate medical products.
I think the challenge that these initiatives have experienced though is that there were no dedicated resources that would really assist countries in streamlining the requirements until 2009, when the African Medicines Regulatory Harmonisation program was started. A lot of partners came together and said, “We need to seriously look into this and see how best we can resolve this.”
What are the strategies for sustaining the momentum of medicines strengthening and harmonization?
African Medicines Regulatory Harmonisation program
The AMRH program aims to establish and improve standards and requirements related to the regulation of — and access to — safe, high-quality medicines for the African population. The program started in 2009 as a response to addressing challenges faced by National Medicine Regulatory Authorities in Africa. These challenges include weak or noncoherent legislative frameworks; sluggish medicine registration processes, and subsequent delayed approval decision; inefficiency and limited technical capacity; among others. The work of AMRH is guided by three focus areas: policy alignment, regional integration and harmonization, and human and institutional capacity development. The vision of AMRH is to ensure that African people have access to state-of-the-art medical products and technologies.
Harmonization could be a system that’s been agreed upon by two, three, or more countries. In the case of the AMRH program, we used African Union regional economic communities. For example the East African Community has six countries — Tanzania, Kenya, Rwanda, Burundi, Uganda, and South Sudan — that have come together and the idea is to now agree on a basic standard they're going to use when it comes to market authorization of medical products.
Similarly, the EAC served as a learning platform and other RECs also coming on board, i.e. the Zazibona initiative in the SADC region and newly funded projects in the economic community of the West African States region. Other regional blocs have also shown interest and embarked on similar work, like the Intergovernmental Authority on Development in the Horn of Africa.
Once that is agreed, the next thing is for guidelines to be used by the industry and then of course the regulators will be in a position to say if the product is safe and of good quality. Once that information is submitted to that agency in that region, you should be able to use a similar procedure for all assessment and marketing authorization. Use the same standards, use the same procedures, conduct joint evaluations, agree that the product is authorized to go on the market across countries — that’s harmonization. As long as countries agree to come together through a platform where they can harmonize, that’s the first step.
Looking ahead to the 3rd Biennial Scientific Conference on Medical Products Regulation in Africa in Accra, Ghana, on Nov. 27-28, what is your key message to attendees?
The key message is basically that it’s time for introspection, retrospection, and reflection, to look back and see where we’ve come from as a continent and analyze all the efforts that have been made in trying to get countries together to build capacity in medical products regulation. It’s to see where we are and be able to plan ahead, taking advantage of the investment and good work on the ground that has gone into this issue so far and to ask how we can go forward now that we have African leadership committed to establishing the African Medicines Agency.
For more information on regulatory harmonization across Africa, stay tuned for Devex’s coverage of the 3rd Biennial Scientific Conference on Medical Products Regulation in Africa 27-28 November.