Sustainable development needs sustainable financing — tackling NCDs is no exception
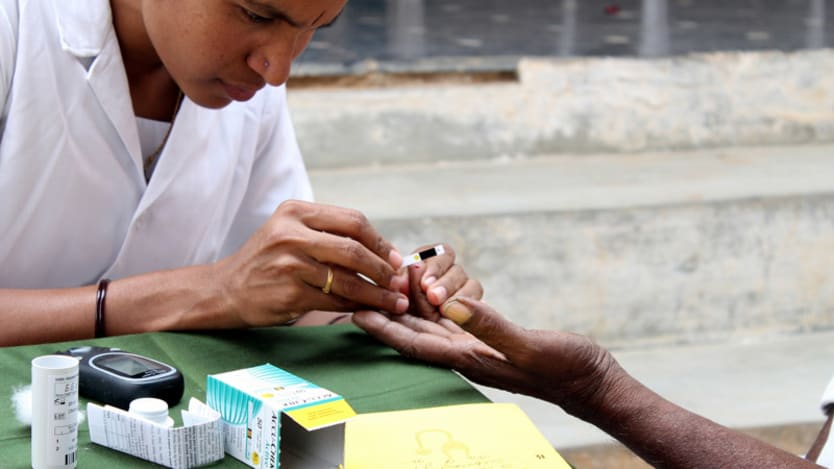
I recently heard the story of Evelyne Musera, a woman being treated for her Type 2 diabetes in Nairobi. Like many Kenyans, Evelyne pays out of her own pocket for the visit, plus the medicines she needs. On top of that, her taxi fares eat into her hard-earned money, and when she skips work to visit the hospital, she is not getting paid. Many others are not so lucky, and are missing out on care altogether due to the relatively high health care costs involved.
Evelyne’s example offers a glimpse of what millions of people — and the governments charged with their care — are confronted by worldwide when it comes to generating the finances needed to prevent and control diabetes and other noncommunicable diseases, namely cardiovascular and lung diseases, and cancers.
Each year, 16 million people die prematurely before the age of 70 from NCDs. Strikingly, 4 out of 5 of these deaths occur in developing countries like Kenya, making such diseases one of the major development challenges of the 21st century. If countries don’t change tack on NCDs, an estimated $7 trillion could be lost in developing countries over the next 15 years. This contrasts starkly with the cost of action: $11 billion a year to implement a set of NCD interventions in all developing countries.
Later this year, countries will gather in New York for the U.N. General Assembly. They will discuss the proposed sustainable development goals, which for the first time recognize the huge impact of NCDs worldwide. The aim is to decrease premature deaths from NCDs by one-third by 2030, and to strengthen implementation of the World Health Organization Framework Convention on Tobacco Control.
Achieving any SDG requires sustainable domestic and international financing. NCDs have long been hidden, misunderstood and underrecorded, and were omitted from the Millennium Development Goals. As a result, NCDs have traditionally struggled to gain significant financing. They have emerged relatively unnoticed in the developing world while the focus of the international community has been on combating HIV, AIDS, malaria and tuberculosis. But the explicit inclusion of NCDs and the WHO FCTC in the SDGs reflects the significant increase in momentum to tackle these diseases. This historic decision is grounded in the commitments made by world leaders in 2011 and 2014 at the United Nations to track the epidemic proportions of NCDs and its impact on development, make prevention the cornerstone of the global response, and strengthen health systems.
The third U.N. International Conference on Financing for Development, held July 13-16 in Addis Ababa, Ethiopia, resulted in the adoption of the Addis Ababa Action Agenda, a new framework to finance the SDGs. This agenda highlights the enormous burden NCDs place on both developed and developing countries. It emphasizes that price and tax measures on tobacco can reduce tobacco consumption and health care costs, as well as representing a revenue stream for financing the SDGs in many countries. It commits parties to the WHO FCTC to strengthen implementation of the convention.
The achievements of the Addis conference went beyond the action agenda. New initiatives to implement the SDGs were announced at six multistakeholder roundtables and 180 side events, including one on financing for health organized by WHO, Barbados and Thailand. The Working Group on Financing for NCDs of the WHO Global Coordination Mechanism on NCDs presented the findings of its interim report — “Financing National NCD Responses in the Post-2015 Era” — that builds on commitments made in Addis Ababa.
The report highlights that significant additional investments are required to meet, by 2030, the NCD-related targets included in the SDGs. For national NCD responses to be implemented and sustained, any new financing will rely primarily on domestic public resources. Reducing NCD deaths is not expensive: banning all forms of tobacco advertising, replacing transfats with polyunsaturated fats, restricting or banning alcohol advertising, preventing heart attacks and strokes, promoting breast-feeding, implementing public awareness programs on diet and physical activity, and preventing cervical cancer through screening are all low-cost and effective public health measures within the reach of most governments.
However, it is equally important that wealthy nations provide more and higher-quality resources to the most in-need countries to complement domestic resources for NCDs. NCDs continue to receive the smallest amount of official development assistance among all major global health areas, accounting for 1 percent of ODA dedicated to health.
The WHO report also highlights the need for a broader range of investors, including the private sector, which must become a key player in the NCDs fight. Contributions from philanthropists will continue to play an increasingly important role. Also, closer and more effective engagement with civil society is vital if we are to turn the tide against NCDs.
The report also highlights opportunities to align government policies in sectors like finance, investment, trade and development to, in turn, support government health policies striving to curb the NCDs epidemic.
Tobacco tax revenues were also identified in Addis as an important source of new sustainable funding for health. Governments already collect over $270 billion in tobacco excise tax revenues each year, according to the report. To date, at least 30 countries are earmarking tobacco tax revenues for health purposes. Thailand, for instance, has used revenues generated from a 2 percent surtax on tobacco and alcohol to fund the ThaiHealth Foundation, which supports health promotion activities.
If the world wants to live up to its promise that no country or person will be left behind, the international development community needs to support domestic efforts in the poorest countries to achieve the NCD-related SDG targets. This will require harnessing ODA to develop institutional capacity for NCDs. Donors must improve their efforts to raise public and private finances.
The call for increased investment in NCDs is growing louder, from rural hospital doctors to the 12 first ladies in Africa who are calling for more financing to fight cancer on the continent. These voices can no longer remain unanswered. They must be acted on, as people all over the world seek protection against NCDs. We must build a future that ensures that globalization becomes a positive force for all current and future generations.
Want to see more coverage of the SDGs? Check out Sustaining Development in partnership with Chevron, FXB, Global Health Fellows Program II, Philips, Pfizer, UNIDO, U.N. Volunteers and the U.S. Council for International Business. You’ll find more Devex news coverage of the SDGs like this article, plus opinion pieces, video interviews, and content provided by our partners.
Read more stories on noncommunicable diseases:
► Is domestic finance the future of TB financing?
► Include children in the SDGs for noncommunicable diseases
► Can tobacco excise taxes be a boon for NCD financing?
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5








