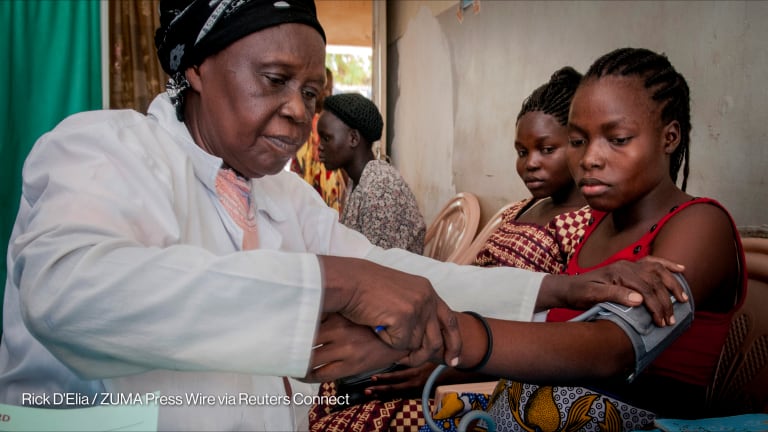Few people in the developed world would ever guess that pneumonia kills more children under the age of 5 than any other disease. This serious respiratory infection takes the lives of nearly a million children each year, with the vast majority of these deaths occurring in developing countries.
World Pneumonia Day on Nov. 12 reminds us of the urgent need to reduce health inequity around the world to ensure that no child dies from pneumonia or other vaccine-preventable disease.
As deputy CEO of Gavi, the Vaccine Alliance — a public-private partnership focused on saving children’s lives in the poorest countries — I am proud to say that since 2000, with the help of our many partners, Gavi has supported the immunization of more than 47 million children against pneumococcal disease. This has helped to almost halve the number of deaths caused by pneumonia.
This comes as part of a broader push that has taken global immunization coverage to an all-time high while cutting child mortality in half. By driving down vaccine prices and increasing access to immunization in the world’s poorest countries, Gavi and its partners have immunized more than half a billion children, preventing 7 million deaths in the process.
But our job is far from finished. More than 19 million children still miss out on the most basic package of vaccinations for common diseases each year, making them vulnerable to disease and death.
In the case of pneumonia what is needed is not major advances in technology, but access to that technology in the form of vaccines. Children are dying because health systems are weak and those who are most at risk are often not being reached with basic health care, including preventive interventions such as vaccines and treatments that they so desperately need when ill.
Access to vaccines is a fundamental human right and one of the most effective ways to protect people from disease and avert illnesses. For children living in the most remote places — whether urban slums, dense jungles or refugee camps — vaccines are often quite literally a lifeline.
Sadly, many of these children are still not being reached, which is all the more tragic given they represent the poorest and most vulnerable children in the world, and those who are most likely to be exposed to the pathogens that cause diseases like pneumonia and diarrhea.
Scaling up coverage
Increasing access to vaccines against childhood killers like pneumonia will increase protection rates in the world’s poorest countries and will, in turn, avert billions of dollars in treatment costs and productivity losses. A scale-up in pneumococcal vaccine coverage until 2020 has the potential to save nearly 3 million lives and prevent 52 million cases of illness.
Controlling childhood pneumonia does not just mean reaching the hardest to reach children with vaccines. Immunization often acts as a powerful platform to offer an integrated bouquet of primary health care services, in particular for women and children.
Overcoming obstacles
I have personally been struck by the ability of vaccination services to transcend barriers of physical infrastructure and reach children in community settings through a system of regular and reliable outreach sessions. Notwithstanding the absence of “bricks and mortar” health facilities, determined frontline health workers travel long distances to deliver vaccines to children in nontraditional settings — such as under a tree. Many even use this opportunity to offer a range of additional maternal and child health services including supplementation, deworming, weighing of babies, contraception and nutritional counseling.
The public health impact of vaccines is further bolstered when accompanied by complementary interventions such as messages around WASH — water, sanitation, and hygiene. Fortunately, many of the interventions targeted at pneumonia also help control other childhood diseases, such as diarrhea and malaria. These interventions should be part of a comprehensive approach to child survival and immunization sessions offer an ideal platform for integrated services.
An integrated approach
Last year, as part of the Global Action Plan for the Prevention and Control of Pneumonia and Diarrhea — an integrated approach to preventing and treating pneumonia and diarrhea — Bangladesh, India and Zambia piloted comprehensive programs aimed at ending the two major preventable causes of child death.
The GAPPD approach includes adequate nutrition, exclusive breastfeeding during the first six months of a child’s life, hand-washing with soap, safe drinking water and sanitation, treatment with oral rehydration solution, antibiotics and zinc as well as immunization.
This idea of bringing together critical health services and interventions to create the healthiest possible environments for children is not new, but it is urgently needed in many parts of the world. This is especially true as the poorest and most deprived children often suffer from myriad deprivations, multiple illnesses and conditions all at the same time — substantially increasing their risk of death, disease or disability.
The benefits of integrated health systems and pneumonia immunization are clear: healthier children and families, better education outcomes for vaccinated children, lower health care costs, increased productivity, stronger economies and thriving communities.
It is a blessing that in wealthier countries, children have access to the vaccines and health systems necessary for them to become healthy, self-sufficient members of society. Let’s work to ensure that children everywhere regardless of their circumstances get the prevention and treatment that they deserve.
Ending a Global Disease is a conversation hosted by Devex, in partnership with Rotary International, to explore successes in the fight against polio and identify lessons that can be applied to overcoming other global diseases. Visit the campaign site and join the conversation using #endpolio.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5