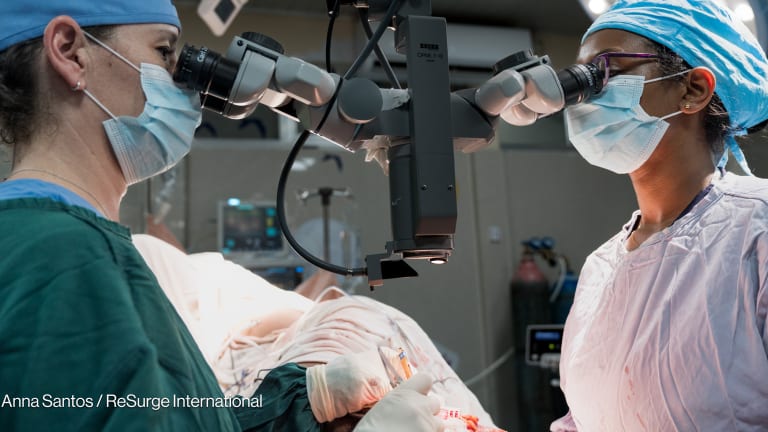
Across West Africa, the normal cycle of birth, life and death continues despite the distress and upheaval caused by the Ebola outbreak.
However, with many clinics and public hospitals closed as health workers are scared to come to report to work, the experience of giving birth or undergoing surgery that can already be complicated enough for many in Africa has become more dangerous. In fact, complications from pregnancy and malaria are now killing more people than Ebola.
When we talk about health in the developing world, it is often through this prism of emergency and the talk of vaccines and wonder drugs needed to bring malaria or HIV under control. These issues are of course vitally important, but we shouldn’t forget that being healthy is not just about being disease-free. It’s also about being free from injury and — where possible — pain.
Many people don’t realize that trauma is a leading cause of disability and death in developing nations and that injuries account for more deaths (around 1.24 million) per year than HIV and AIDS, tuberculosis and malaria combined. When injuries require surgery, that possibility is often unavailable to those living in low- and middle-income countries because of a lack of safe anesthesia.
For example, obstetric fistula is a horrendous injury that can result from prolonged obstructed labor without medical care. It can leave women doubly incontinent, making life a misery and often leading them to be stigmatized within their communities.
Surgical interventions are often vital, but many hospitals have variable electricity supplies and frequent power cuts, which can cause damage to electrical equipment such as overheating, shortened lifespan or even total failure.
At Diamedica we have developed Glostavent anaesthetic machines with this kind of scenario in mind, because their uninterrupted power supply acts as both a backup battery and as a voltage and frequency regulator to protect the equipment. The machines will even continue working during a power cut or when oxygen supplies run out, enabling safe anesthesia and surgery to continue.
We’ve been working to install such machines in hospitals in Liberia, but also in other hospitals across Africa where complications in pregnancy and childbirth are still all too common and dangerous. We’ve also developed a continuous positive airway pressure device driven by a modified oxygen concentrator that is an affordable way of treating newborns and infants with respiratory problems.
Training is as important as technology. The local staff we work with are committed, compassionate and curious. They are eager to learn, not just about just how to better treat their patients but also about how they can look after the equipment they work with.
Some of the methods I use are not always the most orthodox. On a recent trip to Rwanda I ended up using a bottle of cognac from my Air France flight to clean and repair one of the machines that had become clogged up, although I did then show the doctors and nurses how to prevent this from happening again.
For me, innovation in health means finding not just a new idea or solution to a problem, but an appropriate and sustainable one. When applied to development, it is crucial to think about who will be using this technology and whether it is affordable and sustainable over the long term. This can only be done by seeing firsthand the constraining factors that need to be overcome, and working with those that have to deal with those issues on a daily basis.
Only through affordable, appropriate, accessible health care facilities can we hope to give patients the treatment they need to lead healthy and productive lives.
Want to learn more? Check out the Healthy Means campaign site and tweet us using #HealthyMeans.
Healthy Means is an online conversation hosted by Devex in partnership with Concern Worldwide, Gavi, GlaxoSmithKline, International Federation of Pharmaceutical Manufacturers & Associations, International Federation of Red Cross and Red Crescent Societies, Johnson & Johnson and the United Nations Population Fund to showcase new ideas and ways we can work together to expand health care and live better lives.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5